Hospital patients that are prescribed antibiotics are more likely to get fungal infections because of disruption to the immune system in the gut. Immune-boosting drugs could reduce the health risks from complex infections.
Patients prescribed antibiotics in the hospital are more likely to get fungal infections because of disruption to the immune system in the gut.
Using immune-boosting drugs alongside the antibiotics could reduce the health risks from these complex infections, according to a new study from the University of Birmingham and the National Institutes of Health.
The life-threatening fungal infection invasive candidiasis is a major complication for hospitalized patients who are given antibiotics to prevent sepsis and other bacterial infections that spread quickly around hospitals (such as C. diff). Fungal infections can be more difficult to treat than bacterial infections, but the underlying factors causing these infections are not well understood.
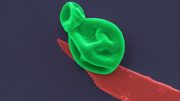
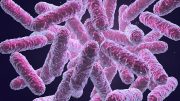
Candidiasis is a fungal infection caused by a yeast (a type of fungus) called Candida. Some species of Candida can cause infection in people; the most common is Candida albicans. Candida normally lives on the skin and in places on the body, such as the mouth, throat, gut, and vagina, without causing any problems. Candida can cause infections if it grows out of control or if it enters deep into the body (for example, the bloodstream or internal organs like the kidney, heart, or brain).
A team in the University’s Institute of Immunology and Immunotherapy, in conjunction with researchers at the National Institutes of Health, discovered that antibiotics disrupt the immune system in the intestines, meaning that fungal infections were poorly controlled in that area. Unexpectedly, the team also found that where fungal infections developed, gut bacteria were also able to escape, leading to the additional risk of bacterial infection.
The study, published in Cell Host and Microbe, demonstrates the potential for immune-boosting drugs, but the researchers also say their work also highlights how antibiotics can have additional effects on our bodies that affect how we fight infection and disease. This in turn underscores the importance of careful stewardship of available antibiotics.
Lead author Dr. Rebecca Drummond said: “We knew that antibiotics make fungal infections worse, but the discovery that bacterial co-infections can also develop through these interactions in the gut was surprising. These factors can add up to a complicated clinical situation – and by understanding these underlying causes, doctors will be better able to treat these patients effectively.”
In the study, the team used mice treated with a broad-spectrum antibiotic cocktail and then infected these animals with Candida albicans, the most common fungus that causes invasive candidiasis in humans. They found that although infected mice had increased mortality, this was caused by infection in the intestine, rather than in the kidneys or other organs.
“These factors can add up to a complicated clinical situation – and by understanding these underlying causes, doctors will be better able to treat these patients effectively.”
— Dr. Rebecca Drummond, Institute of Immunology and Immunotherapy
In a further step, the team pinpointed what parts of the immune system were missing from the gut after antibiotic treatment, and then added these back into the mice using immune-boosting drugs similar to those used in humans. They found this approach helped reduce the severity of the fungal infection.
The researchers followed up the experiment by studying hospital records, where they were able to show that similar co-infections might occur in humans after they have been treated with antibiotics.
“These findings demonstrate the possible consequences of using antibiotics in patients who are at risk of developing fungal infections,” added Dr Drummond. “If we limit or change how we prescribe antibiotics we can help reduce the number of people who become very ill from these additional infections – as well as tackling the huge and growing problem of antibiotic resistance.”
Reference: “Long-term antibiotic exposure promotes mortality after systemic fungal infection by driving lymphocyte dysfunction and systemic escape of commensal bacteria” by Rebecca A. Drummond, Jigar V. Desai, Emily E. Ricotta, Muthulekha Swamydas, Clay Deming, Sean Conlan, Mariam Quinones, Veronika Matei-Rascu, Lozan Sherif, David Lecky, Chyi-Chia R. Lee, Nathaniel M. Green, Nicholas Collins, Adrian M. Zelazny, D. Rebecca Prevots, David Bending, David Withers, Yasmine Belkaid, Julia A. Segre and Michail S. Lionakis, 13 May 2022, Cell Host & Microbe.
DOI: 10.1016/j.chom.2022.04.013




This is what I lived through with my daughter in the late 80’s with the addition of total disbelief from the medical community. Thirty years later all I can say is it’s about time!
Yes. , that’s what antibiotics do.
And a lot of people have experienced the effects.
We all have some fungus in us ,which at a balance in the body it’s ok.
But when taking strong or several courses it seems your skin and / or gut will be irreparable and prone to have issues for a very very long time.
It’s too bad the doctor’s think the short term effect in too many cases is needed.
I wonder if this is the reason i lost my leg to a fungal infection. I was in the hospital with pnemonia and after i went home,ten days later, i ended up back at the hospital with MRSA. I hope that doesnt happen now when I take antibiotics because I just had to take two antibiotics in a row.
Yet our blind faith in the medical profession lingers. Use common sense. Take the natural approach whenever possible. Your doctor wants the most convenient solution to problems. It makes their job much easier. They’re human. They don’t know everything. They know almost nothing actually when you think of what we don’t know. So read a LOT about your condition from a variety of sources (not idiot conspiracy sources of course). Pure food, lots of exercise, clean environment, good sleep…these are the cornerstones of a long, pain free life.