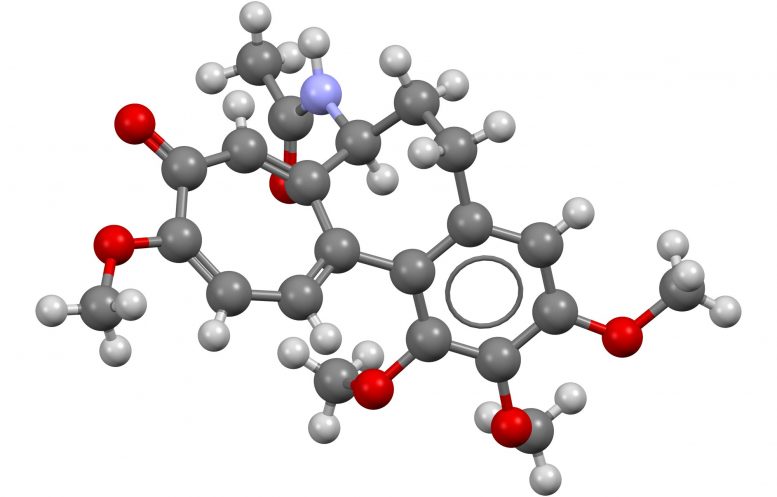
Ball-and-stick model of the colchicine molecule, C22H25NO6. Grey: Carbon, White: Hydrogen, Blue: Nitrogen, Red: Oxygen.
Colchicine worth adding to standard treatment for moderate to severe infection, says researchers.
Colchicine, a cheap drug normally used to treat gout, helps to cut the need for oxygen therapy and hospital stay in COVID-19 patients, reveal the results of a small clinical trial, published in the online journal RMD Open.
The findings prompt the Brazilian researchers to suggest that although it’s not possible to confirm whether colchicine can alter the risk of death, it may nevertheless be worth adding it to standard treatment for hospital patients with moderate to severe COVID-19 infection.
Colchicine has been successfully used to treat and prevent systemic inflammatory conditions, including gout; systemic inflammation is a cardinal feature of moderate to severe COVID-19 infection.
The researchers therefore wanted to find out if adding it to standard treatment might reduce the need for supplemental oxygen, length of hospital stay, including in intensive care, and risk of death in patients with moderate to severe COVID-19 infection.
Moderate disease was defined as fever, breathing difficulties, and pneumonia; severe disease was defined as all of the above, plus a rapid breathing rate of 30 or more times a minute and low levels of oxygen in the body (oxygen saturation of 92% or less).
Between April and August 2020, they randomly assigned 75 patients admitted to hospital with moderate to severe COVID-19 infection to receive either standard treatment plus 0.5 mg colchicine three times a day for 5 days, followed by the same dose twice a day for 5 days, or standard treatment plus a dummy (placebo) drug.
Standard treatment comprised doses of the antibiotic azithromycin, the antimalarial hydroxychloroquine, and the blood thinner heparin, plus a steroid (methylprednisolone) if the need for supplemental oxygen was considerable — equal to 6 liters/minute or more — and intensive care required.
Only five patients were within a healthy weight range: overweight and obesity are known risk factors for more severe COVID-19 infection.
The results are based on 72 patients (36 in each group). The average length of time patients needed oxygen therapy was 4 days for those treated with additional colchicine compared with 6.5 days for those in the standard treatment plus placebo group.
Similarly, the average length of hospital stay was 7 days for the colchicine group compared with 9 for the standard treatment group.
By day 7, fewer than 1 in 10 (9%) of those treated with colchicine needed maintenance oxygen compared with more than 4 out of 10 (42%), in the standard treatment group.
Two patients died, both of whom were in the placebo group. Overall, colchicine was safe and well tolerated, with few side effects; diarrhea was more common in those taking colchicine.
The researchers caution that only a small number of patients were included in the trial, and that they weren’t able to find out if colchicine might avoid the need for intensive care or lessen the risk of death.
Nor is it entirely clear how the drug might help to combat COVID-19 infection. Colchicine is “very unlikely” to have some direct antiviral properties, but it may lessen the body’s inflammatory response and help ward off damage to the cells lining vessel walls (endothelial cells), they suggest.
“Whatever the mechanism of action…colchicine seems to be beneficial for the treatment of hospitalized patients with COVID-19,” they write, adding that it wasn’t associated with serious side effects, such as heart or liver damage or immune system suppression — side effects that have sometimes been linked to some of the other drugs used to treat the infection.
Reductions in the need for oxygen therapy and length of hospital stay are not only good for patients but they cut healthcare costs and the need for hospital beds, added to which colchicine is not an expensive drug, they conclude.
Reference: “Beneficial effects of colchicine for moderate to severe COVID-19: a randomised, double-blinded, placebo controlled clinical trial” by Maria Isabel Lopes, Leticia P Bonjorno, Marcela C Giannini, Natalia B Amaral, Pamella Indira Menezes, Saulo Musse Dib, Samara Libich Gigante, Maira N Benatti, Uebe C Rezek, Laerte L Emrich-Filho, Betania A A Sousa, Sergio C L Almeida, Rodrigo Luppino Assad, Flavio P Veras, Ayda Schneider, Tamara S Rodrigues, Luiz O S Leiria, Larissa D Cunha, Jose C Alves-Filho, Thiago M Cunha, Eurico Arruda, Carlos H Miranda, Antonio Pazin-Filho, Maria Auxiliadora-Martins, Marcos C Borges, Benedito A L Fonseca, Valdes R Bollela, Cristina M Del-Ben, Fernando Q Cunha, Dario S Zamboni, Rodrigo C Santana, Fernando C Vilar, Paulo Louzada-Junior and Rene D R Oliveira, 5 February 20201, RMD Open.
DOI: 10.1136/rmdopen-2020-001455
Funding: FAPESP, CNPq, CAPES








Be the first to comment on "Cheap Gout Drug Help Cuts Need for Oxygen Therapy and Hospital Stay in COVID-19 Patients"