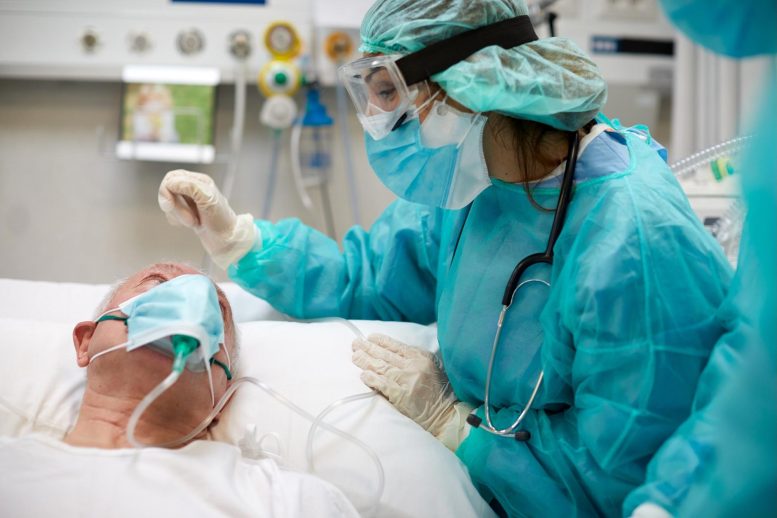
A new study suggests that in patients with COVID-19, a high body mass index (BMI) is linked to an increased risk of death and prolonged stay in the intensive care unit (ICU).
High BMI independently associated with death and longer ICU stay for COVID patients.
Obese patients (BMI >35 kg/m2) were twice as likely to experience a prolonged ICU stay or die, in a large Swedish cohort study.
In patients with COVID-19, a high body mass index (BMI) is associated with an increased risk of death and prolonged intensive care unit (ICU) stay, according to a new study published this week in the open-access journal PLOS ONE by Lovisa Sjögren of Sahlgrenska Academy at University of Gothenburg, Sweden, and colleagues.
Previous studies have shown that a high BMI is a risk factor for severe COVID-19. Obesity increases the risk of comorbidities such as type 2 diabetes and hypertension, and has been shown to increase the need for mechanical ventilation in association with other respiratory infectious diseases such as influenza and pneumonia.

Sahlgrenska Hospital and the Sahlgrenska Academy. Credit: Johan Winborg, CC-BY 4.0
In the new study, Sjögren and colleagues analyzed data on 1,649 COVID-19 patients from the Swedish Intensive Care Registry, a national quality registry which covers all ICUs in Sweden. The patients included in the study were admitted to ICUs during the first wave of the COVID-19 pandemic, between March 6 and August 30, 2020, 96% had a positive PCR test for the SARS-CoV-2 virus or a clinical diagnosis of COVID-19, were all over the age of 18, and had current weight and height data available.
A majority of the study cohort had a high BMI; 78.3% were overweight or had obesity. There was a significant association between increasing BMI and the composite outcome of death during intensive care, or an ICU stay of longer than 14 days in survivors (OR per SD increase: 1.29 95%CI 1.16–1.43 adjusted for age, and sex). Individuals with a BMI of 35 kg/m2 or more were twice as likely to have one of the outcomes of death or prolonged ICU stay, adjusted for age and sex. Moreover, this association remained after adjusting for the presence of cardiovascular disease, hypertension, diabetes mellitus, liver or kidney disease, as well as after adjusting for severity of illness at ICU admission (OR 2.02 [1.39-2.94] versus normal weight). The authors conclude that obesity is an independent risk factor for severe outcome from intensive care in patients with COVID-19 and suggest that BMI be included in the severity scoring for COVID-19 ICU patients.
The authors add: “In this large cohort of Swedish ICU patients with COVID-19, a high BMI was associated with increasing risk of death and prolonged length of stay in the ICU. Based on our findings, we suggest that individuals with obesity should be more closely monitored when hospitalized for COVID-19.”
Reference: “Impact of obesity on intensive care outcomes in patients with COVID-19 in Sweden—A cohort study” by Lovisa Sjögren, Erik Stenberg, Meena Thuccani, Jari Martikainen, Christian Rylander, Ville Wallenius, Torsten Olbers and Jenny M. Kindblom, 13 October 2021, PLoS ONE.
DOI: 10.1371/journal.pone.0257891






Be the first to comment on "COVID Patients With High BMI Face Longer ICU Stay and Increased Risk of Death"