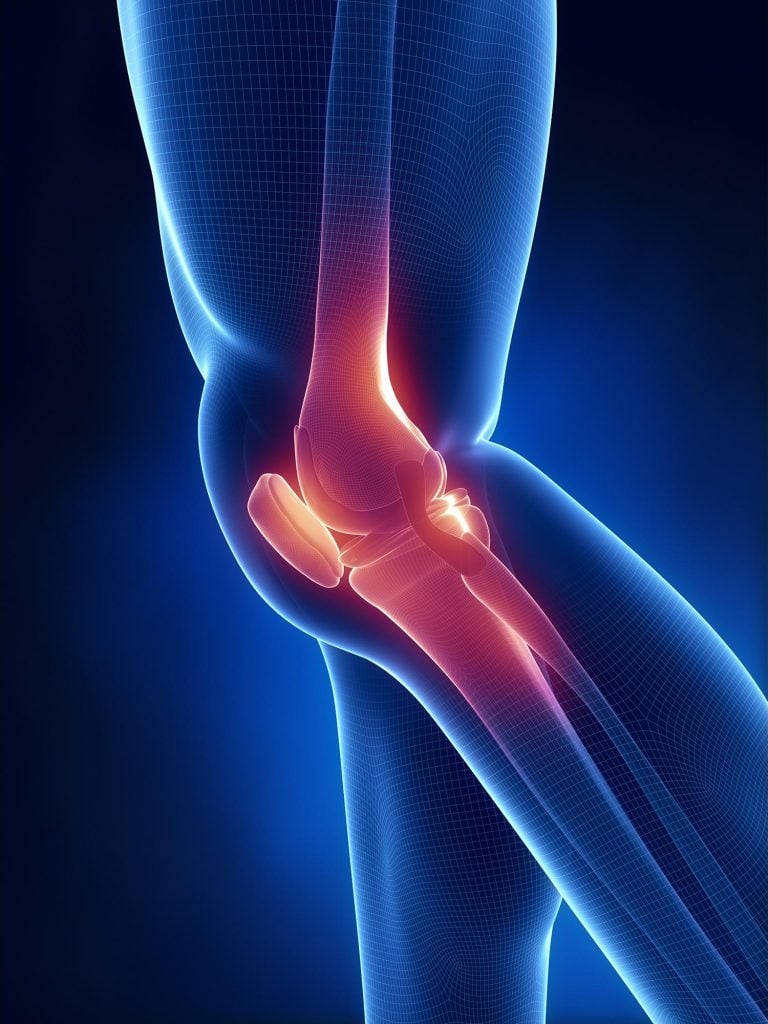
A gel-based cartilage replacement for sore knees has been created by Duke researchers. It is stronger and more long-lasting than the real thing.
The team hopes to conduct clinical trials next year (2023).
Some patients have tried everything to cure their knee pain, including over-the-counter painkillers, physical therapy, and steroid injections. However, their pain persists.
Osteoarthritis, which affects 867 million individuals globally and is estimated to impact one in six of all adults, is often the cause of knee pain. Those who wish to avoid replacing the entire knee joint may soon have another alternative that will allow them to get back on their feet quickly, pain-free, and stay that way.
A Duke University-led team claims in a paper published in the journal Advanced Functional Materials that they have developed the first gel-based cartilage substitute that is even stronger and more durable than the real thing.
Mechanical testing demonstrates that the hydrogel developed by the Duke researchers, which is composed of water-absorbing polymers, is three times more durable than natural cartilage and can be pressed and pulled with more force.
Sparta Biomedical is currently developing and testing implants made of the material on sheep. Researchers are preparing to start human clinical trials next year.
“If everything goes according to plan, the clinical trial should start as soon as April 2023,” said Duke chemistry professor Benjamin Wiley, who led the research along with Duke mechanical engineering and materials science professor Ken Gall.
The Duke scientists took thin sheets of cellulose fibers and infused them with polyvinyl alcohol, a viscous goo made up of stringy chains of repeating molecules, to form a gel in order to create this material.
According to Wiley, the cellulose fibers provide the gel strength when stretched, much like the collagen fibers in natural cartilage. The polyvinyl alcohol helps it return to its original shape. The end product is a Jello-like substance that is 60% water and surprisingly strong.
Before breaking, natural cartilage can endure a stunning 5,800 to 8,500 pounds per inch of pulling and squishing, respectively. Their lab-created version is the first hydrogel capable of handling even more. It is 26% stronger in tension than natural cartilage, which is comparable to dangling seven grand pianos from a key ring, and 66% stronger in compression, which is similar to parking a car on a postage stamp.
“It’s really off the charts in terms of hydrogel strength,” Wiley said.
The team has already made hydrogels with remarkable properties. In 2020, they reported that they had created the first hydrogel strong enough for knees, which feel the force of two to three times body weight with each step.
Putting the gel to practical use as a cartilage replacement, however, presented additional design challenges. One was achieving the upper limits of cartilage’s strength. Activities like hopping, lunging, or climbing stairs put some 10 Megapascals of pressure on the cartilage in the knee, or about 1,400 pounds per square inch. But the tissue can take up to four times that before it breaks.
“We knew there was room for improvement,” Wiley said.
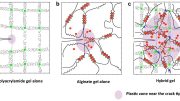
In the past, researchers attempting to create stronger hydrogels used a freeze-thaw process to produce crystals within the gel, which drive out water and help hold the polymer chains together. In the new study, instead of freezing and thawing the hydrogel, the researchers used a heat treatment called annealing to coax even more crystals to form within the polymer network.
By increasing the crystal content, the researchers were able to produce a gel that can withstand five times as much stress from pulling and nearly twice as much squeezing relative to freeze-thaw methods.
The improved strength of the annealed gel also helped solve a second design challenge: securing it to the joint and getting it to stay put.
Cartilage forms a thin layer that covers the ends of bones so they don’t grind against one another. Previous studies haven’t been able to attach hydrogels directly to bone or cartilage with sufficient strength to keep them from breaking loose or sliding off. So the Duke team came up with a different approach.
Their method of attachment involves cementing and clamping the hydrogel to a titanium base. This is then pressed and anchored into a hole where the damaged cartilage used to be. Tests show the design stays fastened 68% more firmly than natural cartilage on bone.
“Another concern for knee implants is wear over time, both of the implant itself and the opposing cartilage,” Wiley said.
Other researchers have tried replacing damaged cartilage with knee implants made of metal or polyethylene, but because these materials are stiffer than cartilage they can chafe against other parts of the knee.
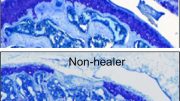
In wear tests, the researchers took artificial cartilage and natural cartilage and spun them against each other a million times, with a pressure similar to what the knee experiences during walking. Using a high-resolution X-ray scanning technique called micro-computed tomography (micro-CT), the scientists found that the surface of their lab-made version held up three times better than the real thing. Yet because the hydrogel mimics the smooth, slippery, cushiony nature of real cartilage, it protects other joint surfaces from friction as they slide against the implant.
Natural cartilage is remarkably durable stuff. But once damaged, it has limited ability to heal because it doesn’t have any blood vessels, Wiley said.
In the United States, osteoarthritis is twice as common today than it was a century ago. Surgery is an option when conservative treatments fail. Over the decades surgeons have developed a number of minimally invasive approaches, such as removing loose cartilage, making holes to stimulate new growth, or transplanting healthy cartilage from a donor. But all of these methods require months of rehab, and some percentage of them fail over time.
Generally considered a last resort, total knee replacement is a proven way to relieve pain. But artificial joints don’t last forever, either. Particularly for younger patients who want to avoid major surgery for a device that will only need to be replaced again down the line, Wiley said, “there’s just not very good options out there.”
“I think this will be a dramatic change in treatment for people at this stage,” Wiley said.
Reference: “A Synthetic Hydrogel Composite with a Strength and Wear Resistance Greater than Cartilage” by Jiacheng Zhao, Huayu Tong, Alina Kirillova, William J. Koshut, Andrew Malek, Natasha C. Brigham, Matthew L. Becker, Ken Gall and Benjamin J. Wiley, 4 August 2022, Advanced Functional Materials.
DOI: 10.1002/adfm.202205662
The study was funded by Sparta Biomedical and by the Shared Materials Instrumentation Facility at Duke University. Wiley and Gall are shareholders in Sparta Biomedical.


Where in Washington state or closet vicinity will this procedure be available? Approximately how much does this procedure cost? Is any type of insurance acknowledged to pay for or help in the expense of the procedure? I look forward to your response and am very excited for the prospect of type of healing and pain relief. Thank you!
How would the surgery take place? Can you describe it perhaps with a diagram? Would it be necessary to cut a lengthy part of the thigh and leg? Thanks 😊
How do you sign up for being a test subject
What is the criteria to be candidate for this type pain relief. Age , weight level of damage etc??
I am have been suffering from knee pain for a long time because I don’t have any cartilage on my knees I need to know how can I sign up as a candidate for the trials
I had my ACL replace in 2018 and they removed my interior meniscus because they were damaged when I torn my ACL and I
Also chip my patella, I went back to running and playing soccer but I am not the same because I don’t have any meniscus in the interior of my knee sometimes I feel pain I that area, I am not doing much running anymore but I have stay fit and my finest level is still very good, this days I do more bicycle and strength training at 57 I can still do 20 pull ups and my core muscle are very strong because of the finest level that I have always keep myself I have been able to return to do physical activities,I run do cycling I swim and I work out my whole body but I know that I don’t have the strength and agility that I had before I torn my ACL and this is because of the pain in my interior meniscus which were removed because they were torn, I would like to participate in the trials in April and I think I would be a good candidate because it is in me, please let me know if I could be one, thank you
Yes, how can I sign up to be a test subject for the surgery trials?
Yes, I’m interested in the information clinical trials for the hydrogel implant. I am on the verge of getting a knee replacement, but find this may be worth waiting for.
What qualifies one to be considered for this clinical trial?
I too am interested in being considered for the trial
I would like to be considered for the trial.
Where and when will this procedure be available? I’d travel to NC if needed.
My right knee has a “shredded” Meniscus and depleted cartilage as verified by X ray, MRI imaging and described per two independent knee surgeons here in MN. Approximately how much does this procedure cost? I’m with United Health and Medicare, which will defray help in the expense of the procedure. No On-going pain except climbing up & down stairs and when twiating my right leg.
I’m an active person, in good health, and like working outrside !
Thank you.