A new study finds that flu vaccination was associated with a 40% reduced risk for Alzheimer’s disease over a four-year period.
Over the course of four years, those who received at least one influenza vaccine were 40% less likely than their non-vaccinated peers to acquire Alzheimer’s disease, according to a new study from the University of Texas Health Science Center at Houston.
Researchers compared the risk of Alzheimer’s disease incidence between patients with and without prior flu vaccination in a large nationwide sample of U.S. adults aged 65 and older. The study was led by first author Avram S. Bukhbinder, MD, a recent alumnus of McGovern Medical School at UTHealth Houston, and senior author Paul. E. Schulz, MD, the Rick McCord Professor in Neurology at McGovern Medical School.
An early online version of the paper detailing the findings is available in advance of its publication in the August 2, 2022, issue of the Journal of Alzheimer’s Disease.
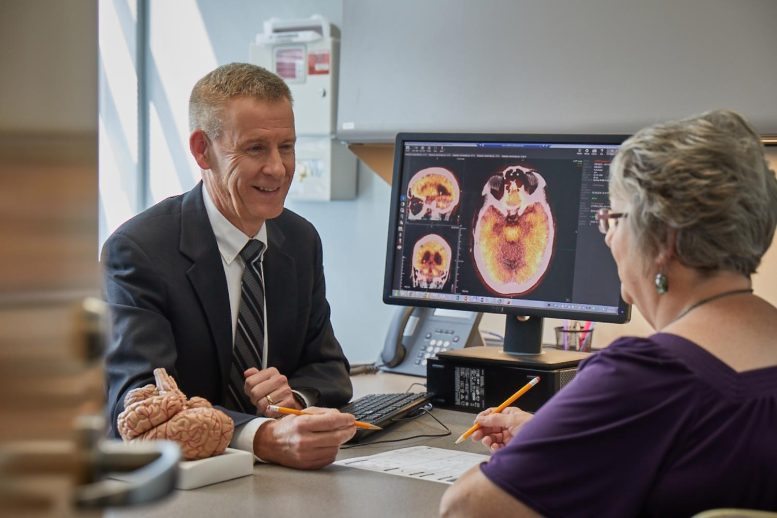
A team of researchers including Paul E. Schulz, MD, found that flu vaccination was associated with a reduced risk for Alzheimer’s disease over a four-year period. Credit: UTHealth Houston
“We found that flu vaccination in older adults reduces the risk of developing Alzheimer’s disease for several years. The strength of this protective effect increased with the number of years that a person received an annual flu vaccine – in other words, the rate of developing Alzheimer’s was lowest among those who consistently received the flu vaccine every year,” said Bukhbinder, who is still part of Schulz’s research team while in his first year of residency with the Division of Child Neurology at Massachusetts General Hospital. “Future research should assess whether flu vaccination is also associated with the rate of symptom progression in patients who already have Alzheimer’s dementia.”
The research study – which comes two years after UTHealth Houston researchers found a possible link between the flu vaccine and reduced risk of Alzheimer’s disease – analyzed a much larger sample than previous research, including 935,887 flu-vaccinated patients and 935,887 non-vaccinated patients.

Avram S. Bukhbinder, MD, a recent alumnus of McGovern Medical School at UTHealth Houston, was first author on the study. Credit: Avram Bukhbinder/UTHealth Houston
During four-year follow-up appointments, about 5.1% of flu-vaccinated patients were found to have developed Alzheimer’s disease. Meanwhile, 8.5% of non-vaccinated patients had developed Alzheimer’s disease during follow-up.
These results underscore the strong protective effect of the flu vaccine against Alzheimer’s disease, according to Bukhbinder and Schulz. However, the underlying mechanisms behind this process require further study.
“Since there is evidence that several vaccines may protect from Alzheimer’s disease, we are thinking that it isn’t a specific effect of the flu vaccine,” said Schulz, who is also the Umphrey Family Professor in Neurodegenerative Diseases and director of the Neurocognitive Disorders Center at McGovern Medical School. “Instead, we believe that the immune system is complex, and some alterations, such as pneumonia, may activate it in a way that makes Alzheimer’s disease worse. But other things that activate the immune system may do so in a different way — one that protects from Alzheimer’s disease. Clearly, we have more to learn about how the immune system worsens or improves outcomes in this disease.”
Alzheimer’s disease affects more than 6 million people living in the U.S., with the number of affected individuals growing due to the nation’s aging population. Past studies have found a decreased risk of dementia associated with prior exposure to various adulthood vaccinations, including those for tetanus, polio, and herpes, in addition to the flu vaccine and others.
Additionally, as more time passes since the introduction of the COVID-19 vaccine and longer follow-up data becomes available, Bukhbinder said it will be worth investigating whether a similar association exists between COVID-19 vaccination and the risk of Alzheimer’s disease.
Reference: “Risk of Alzheimer’s Disease Following Influenza Vaccination: A Claims-Based Cohort Study Using Propensity Score Matching” by Avram S. Bukhbinder, Yaobin Ling, Omar Hasan, Xiaoqian Jiang, Yejin Kim, Kamal N. Phelps, Rosemarie E. Schmandt, Albert Amran, Ryan Coburn, Srivathsan Ramesh, Qian Xiao and Paul E. Schulz, 13 June 2022, Journal of Alzheimer s Disease.
DOI: 10.3233/JAD-220361
Co-authors from McGovern Medical School included Omar Hasan, research coordinator in the Department of Neurology and student at The University of Texas MD Anderson Cancer Center UTHealth Houston Graduate School of Biomedical Sciences; Kamal N. Phelps, fourth-year medical student; Srivathsan Ramesh, PhD, first-year resident in the Department of Orthopedic Surgery; and alumni Albert Amran, MD, and Ryan Coburn, MD. Co-authors from UTHealth Houston School of Biomedical Informatics included Yaobin Ling, graduate research assistant; Xiaoqian Jiang, PhD, the Christopher Sarofim Family Professor in Biomedical Informatics and Engineering; and Yejin Kim, PhD, assistant professor. Qian Xiao, PhD, MPH, assistant professor in the Department of Epidemiology and Disease Control with UTHealth School of Public Health, also co-authored the study.



I wonder how or if they corrected for a selection bias effect, in which individuals with a certain temperament or level of intelligence might be more or less likely to seek out vaccinations. I.E. perhaps seniors with enough presence of mind, foresight, compliance, etc. to accept or request a yearly vaccination are predisposed to a reduced incidence of Alzheimer’s based on those factors, and nothing to do with the vaccination itself.
You are exactly right. The article shows correlation, not causation. There may be a hidden factor that causes both Alzheimer’s and skipping of the flu vaccine.
That said, even correlation is something. For one thing, there is a probability that skipping the flu vaccine is the true cause. Secondly, there’s a chance that forcing oneself to take the flu vaccine indirectly prevents the hidden factor. Imagine the person now starts taking flu vaccine, maybe he also happens to use the blood pressure machine while waiting for the nurse. And finds out he has hypertension. Turns out that the hidden factor is hypertension – by finding out he has hypertension, now there’s a higher chance that he’ll attend to it.