
James Leidner spent three nights in a high-tech sleeping bag that unloads pressure in the brain by suctioning fluids into the lower body. NASA hopes the sack can be used by astronauts in space to alleviate the vision problems they commonly endure during longer missions. Credit: UT Southwestern Medical Center
UTSW brain pressure project critical to Mars mission, NASA says.
A subtle smile emerged on Dr. James Leidner’s face as he envisioned telling people of the unusual contribution he made to mankind’s mission to Mars.
For 72 straight hours, the study volunteer lay in a bed at UT Southwestern, the monotony broken only at night when researchers placed his lower body in a sealed, vacuum-equipped sleeping bag to pull down body fluids that naturally flowed into his head while supine.
New research published in JAMA Ophthalmology shows that by suctioning these fluids and unloading brain pressure, the specially designed sleeping bag may prevent vision problems astronauts endure in space, where fluids float into the head and continually push and reshape the back of the eyeball.
The phenomenon has vexed scientists for more than a decade and remains one of the biggest health dilemmas of human space exploration. But the findings from UT Southwestern – which NASA enlisted to seek answers to astronauts’ vision problems – suggest the high-tech sacks may provide a solution.
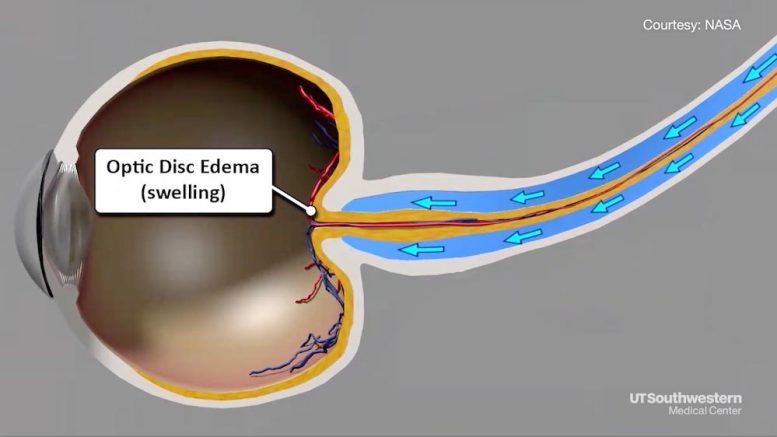
Body fluids in zero gravity apply constant pressure behind the eyes, causing progressive flattening of the eyeball, swelling of the optic nerve, and vision impairment. Credit: UT Southwestern Medical Center
Notably, researchers found that while just three days of lying flat induced enough pressure to slightly alter the eyeball’s shape, no such change occurred when the suction technology was used.
“We don’t know how bad the effects might be on a longer flight, like a two-year Mars operation,” said Benjamin Levine, M.D., a UT Southwestern cardiologist who is helping NASA address the health risks of brain pressure and abnormal blood flow in space. “It would be a disaster if astronauts had such severe impairments that they couldn’t see what they’re doing and it compromised the mission.”
Reshaping eyeballs
NASA hopes the sleeping bag can address a disorder called spaceflight-associated neuro-ocular syndrome, or SANS. The condition is characterized by progressive flattening of the eyeball, swelling of the optic nerve, and vision impairment.
Previous studies by UT Southwestern and the Institute for Exercise and Environmental Medicine at Texas Health Presbyterian Hospital Dallas showed SANS is likely caused by the constant pressure that body fluids apply to the brain.
SANS is not a problem on Earth, where gravity pulls fluids down into the body each time a person gets out of bed. In space, the lack of gravity prevents this daily unloading process, allowing more than half a gallon of body fluids to gather in the head and apply pressure to the eyeball.

Dr. Benjamin Levine of UT Southwestern has researched the effects of space travel since the early 1990s, when he implanted the first catheter to monitor the heart pressure of an astronaut in space. Credit: UT Southwestern Medical Center
NASA has documented vision problems in more than half of the astronauts who served for at least six months on the International Space Station. Some became farsighted, had difficulty reading, and sometimes needed crewmates to assist in experiments.
“You can’t stand up in space to unload the pressure. That’s the problem,” said Michael Stenger, Ph.D., a scientist with NASA’s Human Health Countermeasures Element.
Other risks
Perhaps the best remedy so far has been the use of special space glasses with adjustable lenses that correct astronauts’ changing vision aboard the space station. But this strategy does little to alleviate concerns about the long-term effects on the eyeball, nor the potential cardiovascular complications that Dr. Levine’s team is uncovering.
A 2018 study, for instance, showed that spending six months in zero gravity may increase the odds of developing a common heart arrhythmia called atrial fibrillation. This condition can lead to blood clots, heart attacks or stroke.
“And it’s certainly possible there are other effects of brain pressure we haven’t documented yet,” Dr. Levine said. “The astronauts report something they call the ‘space stupids.’ They make more mistakes than they think they should. Whether that has anything to do with the inability to lower the pressure, we don’t know.”
Although some effects of SANS appear temporary – vision returns to normal shortly after astronauts return to Earth – Dr. Stenger said UT Southwestern’s research is vital to the manned Mars flight that NASA hopes to launch in the 2030s. The sleeping bag technology, in particular, could address both the brain and heart issues.
“What are the long-term health consequences (of SANS)?” Dr. Stenger said. “There’s a large team on the ground working to counteract a lot of these risks.”
Measuring brain pressure
The sleeping bag prototype is the culmination of several phases of research conducted by UT Southwestern to help NASA better understand the disorder, including a 2017 study that provided compelling evidence that constant pressure may indeed contribute to SANS.
To test his theory on brain pressure, Dr. Levine recruited cancer survivors from across the country who still had ports on their heads where they had received chemotherapy. These ports offered researchers rare access to measure pressure directly in the brain.
The volunteers each went on a zero-gravity airplane flight into the upper atmosphere where their body fluids floated upward. A neurosurgeon from UT Southwestern’s Peter O’Donnell Jr. Brain Institute measured the brain pressure by inserting special equipment into the port.
“It was hard,” recalled Wendy Hancock, a leukemia survivor from Philadelphia who agreed to go on more than three dozen up-and-down maneuvers into zero gravity. “But NASA is awesome, so, heck yeah, I was going to jump at the chance to help. … I did it for the astronauts.”
The resulting study showed that brain pressure in a person who lies down on Earth is actually higher than in space. However, on Earth the pressure is unloaded when the person stands and gravity pulls the fluids down. Space provides no such relief for astronauts.
A new remedy
With this crucial insight, Dr. Levine’s team started working with the outdoors equipment retailer REI to develop a high-tech sleeping bag that could be used by astronauts each night to unload pressure in the brain. Although similar lower body negative pressure technology has been used for decades to maintain muscle and bone mass in space, previous prototypes were not designed for many hours of use or tested as an antidote for SANS.
The bag has a solid frame – aptly shaped like a space capsule – and is designed to fit over a person from the waist down.
About a dozen people volunteered to test the technology, including Dr. Leidner, an internal medicine hospitalist in San Antonio who is interested in pursuing a career in aerospace medicine.
He made two visits – three days each – to a UT Southwestern research room where he lay in bed. Only during the second visit was he placed in the sleeping bag for eight hours each night. Researchers compared changes in the brain after each stint.
“Being productive has gone out the window,” he joked, pointing out the awkwardness of typing on his laptop while lying flat. “But it’s an experience I could tell my kid one day if it helps humans land on Mars.”
Several questions need to be answered before NASA brings the technology on the space station, including the optimal amount of time astronauts should spend in the sleeping bag each day.
But Dr. Levine said his latest findings indicate SANS hopefully won’t be a health risk by the time the space agency is ready to launch to the Red Planet.
“This is perhaps one of the most mission-critical medical issues that has been discovered in the last decade for the space program,” Dr. Levine said. “I’m thankful for the volunteers who are helping us understand, and hopefully, fix the problem.”
Long-term research
Dr. Levine has researched the effects of space travel since the early 1990s, when he implanted the first catheter to monitor the heart pressure of an astronaut in space. Since then, he has worked with NASA on various projects and advises its flight surgeons on cardiovascular medical issues. NASA recently awarded him $3.8 million in direct and indirect funding over 13 years to study the effects of space travel on the heart.
Reference: “Effect of Nightly Lower Body Negative Pressure on Choroid Engorgement in a Model of Spaceflight-Associated Neuro-ocular SyndromeA Randomized Crossover Trial” by Christopher M. Hearon Jr, PhD; Katrin A. Dias, PhD; Gautam Babu, MD; John E. T. Marshall, MD; James Leidner, MD; Kirsten Peters, BS; Erika Silva, MS; James P. MacNamara, MD; Joseph Campain, BS and Benjamin D. Levine, MD, 9 December 2021, JAMA Ophthalmology.
DOI: 10.1001/jamaophthalmol.2021.5200
Other key members of Dr. Levine’s team included Christopher Hearon, Ph.D., first author on the JAMA study and Assistant Instructor in the Department of Applied Clinical Research at UT Southwestern; and Tony Whitworth, M.D., a neurosurgeon from the O’Donnell Brain Institute who measured patients’ brain pressure in zero gravity.
Dr. Levine is Professor of Internal Medicine and Director of the Institute for Exercise and Environmental Medicine at Texas Health Presbyterian Hospital Dallas, a partnership between UT Southwestern and Texas Health Resources. He holds the Distinguished Professorship in Exercise Sciences at UT Southwestern.
About UT Southwestern Medical Center
UT Southwestern, one of the nation’s premier academic medical centers, integrates pioneering biomedical research with exceptional clinical care and education. The institution’s faculty has received six Nobel Prizes, and includes 25 members of the National Academy of Sciences, 16 members of the National Academy of Medicine, and 14 Howard Hughes Medical Institute Investigators. The full-time faculty of more than 2,800 is responsible for groundbreaking medical advances and is committed to translating science-driven research quickly to new clinical treatments. UT Southwestern physicians provide care in about 80 specialties to more than 117,000 hospitalized patients, more than 360,000 emergency room cases, and oversee nearly 3 million outpatient visits a year.








So… What… you are saying is that Humans are poorly adapted to ((SPACE)) the purported ((FINAL FRONTIER)). May be… The ((GIANT LEAP)) for Mankind into ((OBLIVION)). Yep. Damn the Earth. Full speed ahead… at twice the price: What profit it a Man to LOSE the EARTH and GAIN a VOID? (Aka: A hole in the Cosmic Ground where one is but a shadow FIGURE, an outline far more voided than the surrounding ((SPACE))(.) Period
Like NOWHERE MAN: “We’ll” get there eventually. EVERY BODY does. In the INTERIM we will SETTLE, for NOTHING more-or-less-is-more than SMOKE AND MIRRORS… and ASH.
“The Expanse” (Tee-hee V x MC²=Cosmic Joke) comes to mind: Humanity has pushed the envelope, FAR INTO ((THE FUTURE!)) Still CRAZY, still MAKING WAR… After All These Years. The RETURNING WARRIOR (untimely retirement) comes down to Earth: Blind as a stone, bow-legged, shrunken and bent by unfamiliar gravity, perpetually dizzy, and crazier than a Loon… Endlessly repeating: Go for it! Go for it! Go for it…
And NOW, Cats and Kittens, a message from our SPONSOR…
👇
⚡
🙈
((BAD MONKEY!))