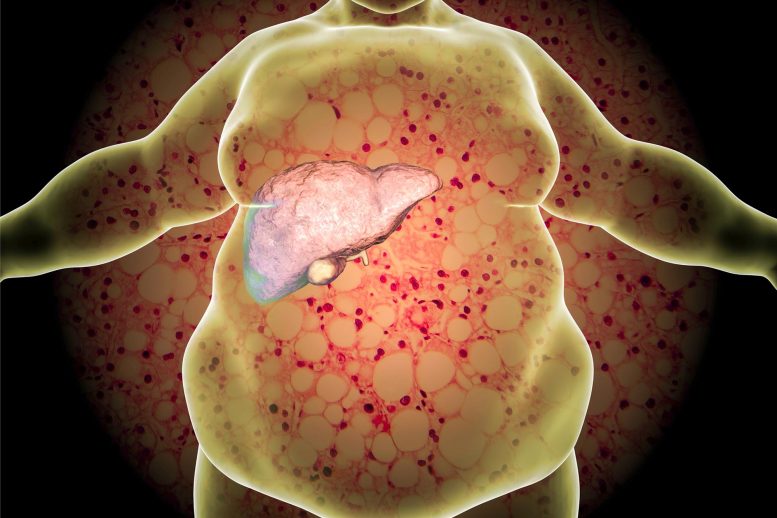
Research from scientists at the Yale School of Medicine suggests that obesity and chronic liver disease from altered populations of microbes in the stomach may be infectious. While studying healthy mice, they found that the mice developed susceptibility to the development of liver disease and obesity when co-housed with mice containing the altered gut microbes. The researchers hope to use these findings to further the research of NAFLD and metabolic syndrome.
Obesity and chronic liver disease can be triggered by a family of proteins that alter populations of microbes in the stomach, a discovery that suggests the condition may be infectious, Yale scientists report. The study, in the advance online publication of Nature, expands on earlier Yale research that showed how similar microbial imbalances caused by the same family of proteins increases the risk of intestinal diseases such as colitis.
The Yale scientists’ most extraordinary finding, they said, was that the altered intestinal environment that led to obesity and liver disease was infectious among the community of mice. “When healthy mice were co-housed with mice that had altered gut microbes, the healthy mice also developed a susceptibility for development of liver disease and obesity,” said senior author Richard A. Flavell, professor of immunobiology at Yale School of Medicine and a Howard Hughes Medical Institute investigator.
The proteins in question are called inflammasomes. They are responsible for launching the immune system’s inflammatory response. Inflammasomes act as sensors and regulators of the microbial environment of the intestines.
The Yale team found that a deficiency in components of two particular inflammasomes in mice resulted in the development of an altered microbial community associated with increased bacteria. This determined the severity of non-alcoholic fatty liver disease (NAFLD) and obesity in the mice.
NAFLD is the result of metabolic syndrome, a collection of disorders that includes obesity and diabetes, and is the leading cause of chronic liver disease in the western world. It is estimated that up to 30 million people suffer from NAFLD in the United States alone. Twenty percent of people with NAFLD develop chronic liver inflammation, placing them at risk for cirrhosis and liver cancer, but the causes have been unclear.
The next step, Flavell said, is extending this research to humans and to identify more precisely the bacteria involved in the progression to liver disease. “We found, in mice, that targeted antibiotic treatment brought the microbial composition back to normal, and thus eased the liver disease. Our hope is that our findings may eventually lead to a treatment for humans.”
Reference: “Inflammasome-mediated dysbiosis regulates progression of NAFLD and obesity” by Jorge Henao-Mejia, Eran Elinav, Chengcheng Jin, Liming Hao, Wajahat Z. Mehal, Till Strowig, Christoph A. Thaiss, Andrew L. Kau, Stephanie C. Eisenbarth, Michael J. Jurczak, Joao-Paulo Camporez, Gerald I. Shulman, Jeffrey I. Gordon, Hal M. Hoffman and Richard A. Flavell, 1 February 2012, Nature.
DOI: 10.1038/nature10809
The researchers who led this project in Flavell’s laboratory are Jorge Henao-Mejia, Eran Elinav, and Chengcheng Jin. Other participating researchers were Liming Hao, Wajahat Z. Mehal, Till Strowig, Christoph A. Thaiss, Stephanie C. Eisenbarth, Michael J. Jurczak, Joao-Paulo Camporez, and Gerald I. Shulman of Yale; Andrew L. Kau and Jeffrey I. Gordon of Washington University School of Medicine; and Hal M. Hoffman of the University of California at San Diego.
The study was supported by grants from the Howard Hughes Medical Institute, United States-Israel Binational Foundation, the Crohn’s and Colitis Foundation of America, the National Institutes of Health, a VA Merit Award, and the Claire and Emmanuel G. Rosenblatt Award from the American Physicians for Medicine in Israel Foundation. Postdoctoral fellowships were provided by The Cancer Research Institute, and the Leukemia and Lymphoma Society.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.