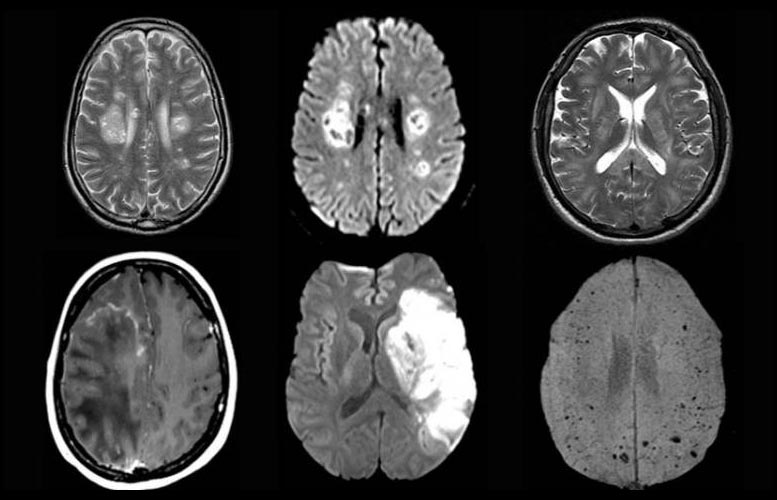
Neurological complications of COVID-19 can include delirium, brain inflammation, stroke, and nerve damage, finds a new UCL and UCLH-led study.
Published in the journal Brain, the research team identified one rare and sometimes fatal inflammatory condition, known as ADEM, which appears to be increasing in prevalence due to the pandemic.
Some patients in the study did not experience severe respiratory symptoms, and the neurological disorder was the first and main presentation of COVID-19.
Joint senior author Dr. Michael Zandi (UCL Queen Square Institute of Neurology and University College London Hospitals NHS Foundation Trust) said: “We identified a higher than expected number of people with neurological conditions such as brain inflammation, which did not always correlate with the severity of respiratory symptoms.
“We should be vigilant and look out for these complications in people who have had COVID-19. Whether we will see an epidemic on a large scale of brain damage linked to the pandemic – perhaps similar to the encephalitis lethargica outbreak in the 1920s and 1930s after the 1918 influenza pandemic – remains to be seen.”
The study provides a detailed account of neurological symptoms of 43 people (aged 16-85) treated at the National Hospital for Neurology and Neurosurgery, UCLH, who had either confirmed or suspected COVID-19.
The researchers identified 10 cases of transient encephalopathies (temporary brain dysfunction) with delirium, which corresponds with other studies finding evidence of delirium with agitation. There were also 12 cases of brain inflammation, eight cases of strokes, and eight others with nerve damage, mainly Guillain-Barré syndrome (which usually occurs after a respiratory or gastrointestinal infection).
Most (nine out of 12 cases) of those with brain inflammation conditions were diagnosed with acute disseminated encephalomyelitis (ADEM). ADEM is rare and typically seen in children and can be triggered by viral infections: the team in London normally sees about one adult patient with ADEM per month, but that increased to at least one per week during the study period, which the researchers say is a concerning increase.
The virus causing COVID-19, SARS-CoV-2, was not detected in the cerebrospinal brain fluid of any of the patients tested, suggesting the virus did not directly attack the brain to cause the neurological illness. Further research is needed to identify why patients were developing these complications.
In some patients, the researchers found evidence that the brain inflammation was likely caused by an immune response to the disease, suggesting that some neurological complications of COVID-19 might come from the immune response rather than the virus itself.
The findings add clinical descriptions and detail to another recent study, which also involved Dr. Zandi and co-author Dr. Hadi Manji (UCL Queen Square Institute of Neurology and UCLH) identifying 153 people with neurological complications from COVID-19. This paper also confirms the previously reported findings of a higher than expected number of patients with stroke which results from the excessive stickiness of the blood in COVID-19 patients.
Joint first author Dr. Ross Paterson (UCL Queen Square Institute of Neurology) said: “Given that the disease has only been around for a matter of months, we might not yet know what long-term damage COVID-19 can cause.
“Doctors need to be aware of possible neurological effects, as early diagnosis can improve patient outcomes. People recovering from the virus should seek professional health advice if they experience neurological symptoms,” he added.
Joint first author Dr. Rachel Brown (UCL Queen Square Institute of Neurology and UCL Infection & Immunity) said: “Our study advances understanding of the different ways in which COVID-19 can affect the brain, which will be paramount in the collective effort to support and manage patients in their treatment and recovery.”
Joint senior author Dr. Hadi Manji said: “Our study amalgamates, for the first time, the clinical presentations of patients with COVID-19 neurological disease with MRI and laboratory features including, in one case, a brain biopsy.
“This now sets up a template for other researchers around the world, facilitating coordinated research to optimize the diagnosis and treatments of these complications, which to date, has proved difficult. In addition, patients are going to require long term follow up.”
Reference: “The emerging spectrum of COVID-19 neurology: clinical, radiological and laboratory findings” by Ross W Paterson, Rachel L Brown, Laura Benjamin, Ross Nortley, Sarah Wiethoff, Tehmina Bharucha, Dipa L Jayaseelan, Guru Kumar, Rhian E Raftopoulos, Laura Zambreanu, Vinojini Vivekanandam, Anthony Khoo, Ruth Geraldes, Krishna Chinthapalli, Elena Boyd, Hatice Tuzlali, Gary Price, Gerry Christofi, Jasper Morrow, Patricia McNamara, Benjamin McLoughlin, Soon Tjin Lim, Puja R Mehta, Viva Levee, Stephen Keddie, Wisdom Yong, S Anand Trip, Alexander J M Foulkes, Gary Hotton, Thomas D Miller, Alex D Everitt, Christopher Carswell, Nicholas W S Davies, Michael Yoong, David Attwell, Jemeen Sreedharan, Eli Silber, Jonathan M Schott, Arvind Chandratheva, Richard J Perry, Robert Simister, Anna Checkley, Nicky Longley, Simon F Farmer, Francesco Carletti, Catherine Houlihan, Maria Thom, Michael P Lunn, Jennifer Spillane, Robin Howard, Angela Vincent, David J Werring, Chandrashekar Hoskote, Hans Rolf Jäger, Hadi Manji, Michael S Zandi, the UCL Queen Square National Hospital for Neurology and Neurosurgery COVID-19, 8 July 2020, Brain.
DOI: 10.1093/brain/awaa240
The researchers were supported by the National Institute for Health Research UCLH Biomedical Research Centre, Medical Research Council, Alzheimer’s Association, and the UK Dementia Research Institute.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
How many were vaccinated with mRNA shots? Where is the limitations section ?