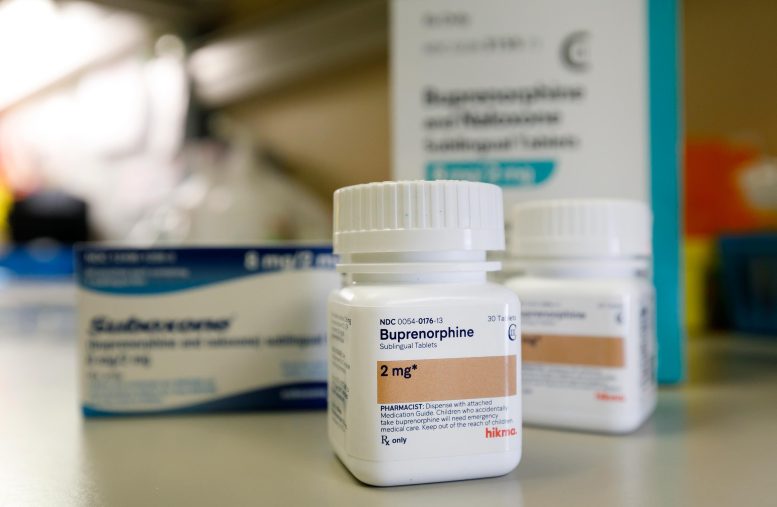
A new study sheds light on resistance to using buprenorphine — a proven tool in fighting opioid epidemic.
New research reveals that only one in four adolescent residential treatment centers across the United States provides a medication used to treat opioid use disorder, despite an ever-rising number of overdose deaths among young people nationwide resulting from a surge of illicit fentanyl.
The study, led by researchers at Oregon Health & Science University, was published on June 13 in the Journal of the American Medical Association.
Researchers say the lack of buprenorphine in adolescent residential treatment centers undercuts U.S. efforts to alleviate an overdose epidemic that claimed more than 109,000 lives in 2022, according to predicted provisional statistics from the Centers for Disease Control and Prevention, or CDC. Recognizing the particular vulnerability of young people, especially as fentanyl now contaminates other illicit substances, OHSU researchers set out to determine how many adolescent treatment centers in the U.S. were providing buprenorphine to treat addiction.
Buprenorphine is one of three medications for opioid use disorder (MOUD) approved by the Food and Drug Administration (FDA). Methadone and naltrexone are the other two MOUDs, which may be the right treatment options for certain patients depending on their preferences and circumstances.
“These residential treatment centers see some of the most vulnerable adolescents in our communities,” said lead author Caroline King, M.D., Ph.D., who conducted the research as a medical student at OHSU and is now an emergency medicine resident in the Yale School of Medicine. “But they don’t offer the standard of care for these kids. With rising fentanyl-related overdoses among adolescents, we really need these centers to provide the best care.”
The surge in illegal fentanyl is reaching young people nationwide and in the Pacific Northwest, dramatically increasing the number of overdose deaths in recent years, according to data from the CDC.
Barriers to Buprenorphine Adoption in Adolescents
Buprenorphine is one of three medications approved by the Food and Drug Administration to treat opioid dependence. It normalizes brain function by acting on the same target in the brain as prescription opioids, heroin or fentanyl — all highly addictive substances.
“It’s the one medication that’s approved for use in adolescents, and it’s underused in facilities taking care of kids with the most severe opioid use disorder,” said co-author Todd Korthuis, M.D., M.P.H., head of addiction medicine in the OHSU School of Medicine. “It’s hard to imagine getting adolescents with opioid use disorder off fentanyl without buprenorphine.”
Although buprenorphine is not approved in the U.S. for people younger than 16, there is no evidence to suggest major safety concerns for use at younger ages. The American Society of Addiction Medicine recommends that buprenorphine be considered for the treatment of opioid use disorder in younger people.
Korthuis acknowledged that some treatment providers have resisted using buprenorphine even with adult patients, claiming it’s replacing one drug for another.
“It’s a big issue,” he said. “But it’s something that we can change by supporting these treatment centers with education and technical assistance about buprenorphine, advocating for better funding to staff these centers, and by letting the public know that buprenorphine is necessary treatment in healing brains.”
Results of the new study suggest that most adolescent residential treatment centers could benefit from such support.
King and three other OHSU medical students conducted the study by cataloging treatment centers that serve adolescents in the U.S., primarily through a database maintained by the U.S. Substance Abuse and Mental Health Services Administration, or SAMHSA. They identified 354 residential treatment centers nationally, but fewer than half of them served adolescents.
Researchers posed as the aunt or uncle of a 16-year-old seeking treatment after a recent non-fatal fentanyl overdose. Between October and December of last year, they began making calls.
After connecting with 160 residential treatment facilities serving adolescents nationwide, the researchers found:
- 39 offered buprenorphine, including through partnership with outside prescribing clinicians. Only 12 of those offered it to adolescents younger than 16.
- Among the other 121 facilities that did not offer buprenorphine or weren’t sure, 57 indicated adolescents prescribed buprenorphine by their own clinician could stay on it at least temporarily, although some stated they would discontinue it before discharge.
- 27 residential treatment centers required adolescents to be off buprenorphine at admission — meaning these “abstinence-only” centers actually refuse to admit adolescents receiving proven medication-assisted therapy.
In sum, only one of four adolescent residential treatment centers offered buprenorphine at all — and even fewer offered buprenorphine for ongoing treatment.
“The average parent would need to call nine facilities on the SAMHSA list to find one that offered buprenorphine,” the authors write. “To find one for an adolescent under 16, they would need to call 29 facilities.”
Reference: “Treatments Used Among Adolescent Residential Addiction Treatment Facilities in the US, 2022” by Caroline King, PhD, MPH; Tamara Beetham, MPH; Natashia Smith, MD; Honora Englander, MD; Scott E. Hadland, MD, MPH, MS; Sarah M. Bagley, MD, MSc and P. Todd Korthuis, MD, MPH, 13 June 2023, JAMA.
DOI: 10.1001/jama.2023.6266
For more information on substance and mental health treatment programs in your area, call the free and confidential National Helpline 1-800-662-HELP (4357) or visit www.FindTreatment.gov.
The research was supported by the National Institute on Drug Abuse of the National Institutes of Health, award K23DA045085, R01DA057566, K23DA044324 and UG1DA01581; the Agency for Healthcare Research and Quality award T32HS017589; and the Oregon Clinical and Translational Research Institute award UL1TR002369 from the National Center for Research Resources, a component of the NIH and the NIH Roadmap for Medical Research.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
Before aspirin was invented and became popular everybody that had access the world over used opiates and opium because there were no other good treatments. In US between 1920 and 1930 when opiates were still available the US census says that an average of only 35 people a year died of opiate overdoses. Acetaminophen(Tylenol) has 500 deaths a year and the current population is about 3 times the population at that time.
People have turned to alcohol and cigarettes to release the opium-like compound called beta-endorphin that our bodies make to provide them with the pleasure that opiates and opium used to provide and that is causing about 12 million deaths a year, about 9 million from smoking cigarettes and about 3 million from drinking alcohol.
The main effect of opiates and opium is to increase a persons ability to concentrate. They can not concentrate on pain and they won’t feel it as much and it is bearable or they concentrate on something pleasurable like music and hear every note. Different people have different tolerances so that some people like it a lot and some do not like it at all. apparently the main reason for making opiates and opium illegal to start with was to keep Chinese immigrants from getting rich off of Americans.