Duke engineers have grown the first functioning human muscle from non-muscle cells — in this case skin cells reverted to their primordial stem cell state. The ability to start from cellular scratch using non-muscle tissue will allow scientists to grow far more muscle cells, provide an easier path to genome editing and cellular therapies, and develop individually tailored models of rare muscle diseases for drug discovery and basic biology studies.
Biomedical engineers have grown the first functioning human skeletal muscle from induced pluripotent stem cells.
The advance builds on work published in 2015 when researchers at Duke University grew the first functioning human muscle tissue from cells obtained from muscle biopsies. The ability to start from cellular scratch using non-muscle tissue will allow scientists to grow far more muscle cells, provide an easier path to genome editing and cellular therapies, and develop individually tailored models of rare muscle diseases for drug discovery and basic biology studies.
“Starting with pluripotent stem cells that are not muscle cells, but can become all existing cells in our body, allows us to grow an unlimited number of myogenic progenitor cells,” said Nenad Bursac, professor of biomedical engineering at Duke University. “These progenitor cells resemble adult muscle stem cells called ‘satellite cells’ that can theoretically grow an entire muscle starting from a single cell.”
In their previous work, Bursac and his team started with small samples of human cells obtained from muscle biopsies, called “myoblasts,” that had already progressed beyond the stem cell stage but hadn’t yet become mature muscle fibers. They grew these myoblasts by many folds and then put them into a supportive 3-D scaffolding filled with a nourishing gel that allowed them to form aligned and functioning human muscle fibers.
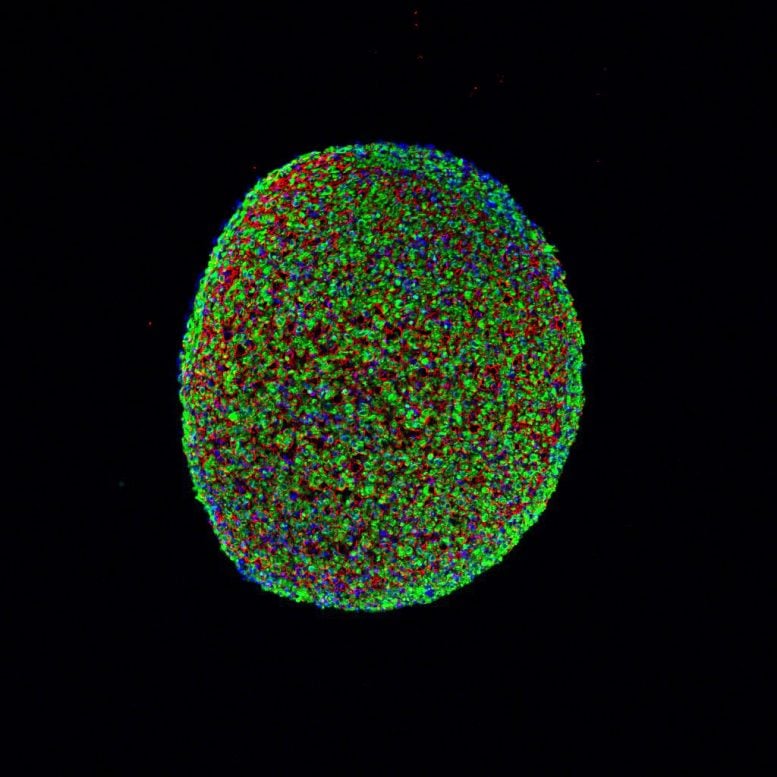
In the new study, the researchers instead started with human induced pluripotent stem cells. These are cells taken from adult non-muscle tissues, such as skin or blood, and reprogrammed to revert to a primordial state. The pluripotent stem cells are then grown while being flooded with a molecule called Pax7 — which signals the cells to start becoming muscle.
As the cells proliferated they became very similar to –but not quite as robust as — adult muscle stem cells. While previous studies had accomplished this feat, nobody has been able to then grow these intermediate cells into functioning skeletal muscle.
The Duke researchers succeeded where previous attempts had failed.
“It’s taken years of trial and error, making educated guesses and taking baby steps to finally produce functioning human muscle from pluripotent stem cells,” said Lingjun Rao, a postdoctoral researcher in Bursac’s laboratory and first author of the study. “What made the difference are our unique cell culture conditions and 3-D matrix, which allowed cells to grow and develop much faster and longer than the 2-D culture approaches that are more typically used.”
Once the cells were well on their way to becoming muscle, Bursac and Rao stopped providing the Pax7 signaling molecule and started giving the cells the support and nourishment they needed to fully mature.
In the study, the researchers show that after two to four weeks of 3-D culture, the resulting muscle cells form muscle fibers that contract and react to external stimuli such as electrical pulses and biochemical signals mimicking neuronal inputs just like native muscle tissue. They also implanted the newly grown muscle fibers into adult mice and showed that they survive and function for at least three weeks while progressively integrating into the native tissue through vascularization.
The resulting muscle, however, is not as strong as native muscle tissue, and also falls short of the muscle grown in the previous study that started from muscle biopsies. Despite this caveat, the researchers say this muscle still holds potential that the stronger, older relative does not.
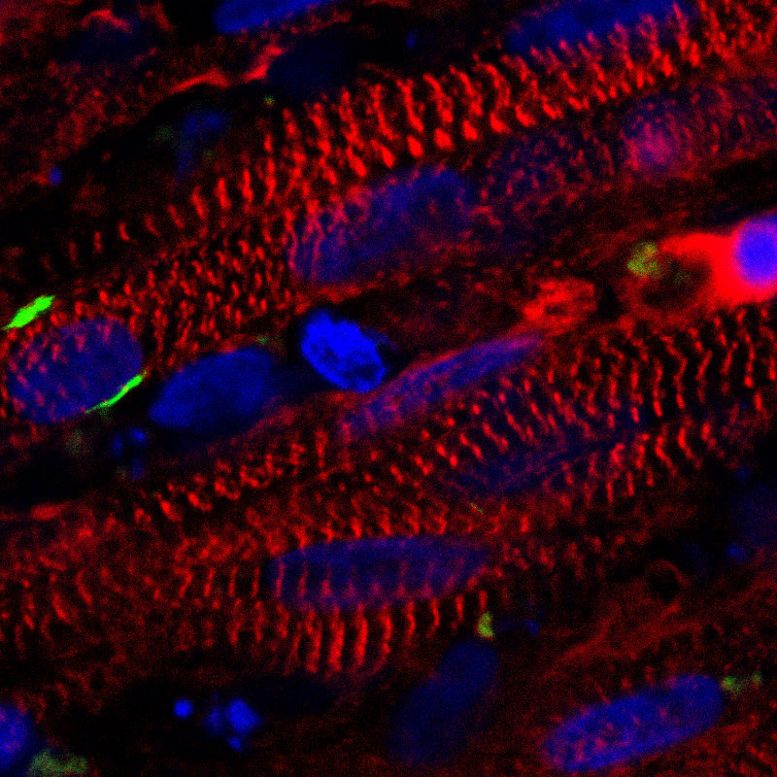
The pluripotent stem cell-derived muscle fibers develop reservoirs of “satellite-like cells” that are necessary for normal adult muscles to repair the damage, while the muscle from the previous study had much fewer of these cells. The stem cell method is also capable of growing many more cells from a smaller starting batch than the biopsy method.
Both of the advantages point toward a possibility of using this new method for regenerative therapies and for creating models of rare diseases for future studies and individualized health care.
“The prospect of studying rare diseases is especially exciting for us,” said Bursac. “When a child’s muscles are already withering away from something like Duchenne muscular dystrophy, it would not be ethical to take muscle samples from them and do further damage. But with this technique, we can just take a small sample of non-muscle tissue, like skin or blood, revert the obtained cells to a pluripotent state, and eventually grow an endless amount of functioning muscle fibers to test.”
The technique also holds promise for being combined with genetic therapies. Researchers could, in theory, fix genetic malfunctions in the induced pluripotent stem cells derived from a patient and then grow small patches of completely healthy muscle. While this could not heal or replace an entire body’s worth of diseased muscle, it could be used in tandem with more widely targeted genetic therapies or to heal more localized problems.
The researchers are now refining their technique to grow more robust muscles and beginning work to develop new models of rare muscle diseases.
Reference: “Engineering human pluripotent stem cells into a functional skeletal muscle tissue” by Lingjun Rao, Ying Qian, Alastair Khodabukus, Thomas Ribar & Nenad Bursac, 9 January 2018, Nature Communications.
DOI: 10.1038/s41467-017-02636-4
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
4 Comments
I’m fascinated by the current articles I’m wondering if there or have been current science pertaining to aneurysm repair
TWO HYPERBARIC OXYGEN TREATMENT FACILITIES.IN ANCHORAGE ALASKA AND IN PALMER WASILLA AREA 40 MILES OUTSIDE OF ANCHORAGE.Smile
Maureen – Look into hyperbaric oxygen chamber therapy. I think the pioneering work is being done in Israel.
The stuff I read about had to do with recovery of function in victims of stroke, and brain damage from severe accidents. Even 20 years after the original damage occurred.
People were regaining some ability to walk and talk where they weren’t able to previously, with improvements happening on a progressively upward climb and showing marked positive results within several sessions.
I don’t know if any of the work is specific to your question. Arent strokes caused by aneurysms?
Forgive my ignorance if Im wrong.
I also don’t know if anyone has picked up on it and is using it in the US. I doubt it. Regulatory FDA has a track record of shutting down those methods that actually heal people.
Another possibility for healing, is a stem cell clinic in panama, where people are being successfully treated for many different health issues relating to damaged tissue and its repair. Even old age and massive organ failure.
You won’t find the info from doing a general search cuz the FDA is in big pharmas back pocket, so the treatments are illegal in the US.
(Big pharma doesn’t like cures. They like monthly scripts that treat the symptoms of the cause while never curing it.)
Anyway, to start your journey down that path, I would ask you to look up on youtube, these search words…
Joe rogan, Mel gibson, stem cells.
That should help you decide if you want to pursue it any further.
Once you get specific info like the doctors name, the clinics name, the type of stem cells used, then you can do searches on those terms, and you will get specific results for further info.
Hope this info helps you and brings your attention to the fact that your gov is not for the people by the people but is instead for the profit for the corporation, at the expense of the peoples health, wealth, and spiritual well being. And freedom.
[All of the following doesn’t pertain to healing aneurysms, but further proves my point (I was on a roll and i went with it) that there are real cures out there for some of this countries biggest killers of its citizens.
And that even though they are cheap and readily available, you cant have them.]
As long as im on this rant, and that the odds of you, or a loved one getting cancer is 1 out of 3 and rising…
look up on youtube again, DCA cancer cure, and learn about a cure that is already FDA approved 40 years ago, that you wont be treated with if you get cancer, cuz its patent went generic long ago and there’s no profit in prescribing it.
It has no permanent side effects and cures metastatic lung, brain, and colon cancers 100%. Cures. Not treats.
I sound like a cheap infomercial or like im selling a product for personal gain. I am not.
I just hate to see people suffer. Especially when that suffering is caused by greedy evil politician puppets of large corporation cash, when they are aware of the cures and choose to suppress them.
Good luck and good health to you and anyone else that reads this.
Your government is corrupt. Both parties are complicit. Two sides of the same coin.
Change it. Legally and peacefully.
The cost of allowing it to continue is your very lives. Make people aware they can’t enjoy a long healthy life cuz their government works for corporate objectives that suppress and make illegal the cures. New and old.
Its all about profits, not peoples lives.
Here’s another one! (Sorry)
For the opiate abuse epidemic that could be cured but isn’t cuz there is too much money being made on both ends of it…
The drugs that get them hooked and addicted, and the methadone they use the rest of their lived when they quit.
And the private for profit treatment centers that have a success rate of 8%, insuring repeat customers who are most often court ordered to go vs a prison sentence.
Guess who the primary investors are in building these treatment centers? The judges who do the sentencing. The county prosecutors and defense attorneys.
A typical 30 day sentence to a full (the waiting list is back logged for a year) 60 bed facility, at $10,000 a head per month, is $600,000 a month. I think that comes out to 7.2 million a year.
A $20 million in patient clinic would be paid off in 3 years. Low overhead in the counselors are all “recovering” addicts, without degrees in anything.
Means the investors that financed its construction, and sit on the board of its operation, (remember the 8% success rate?) Are splitting 7.2 million a YEAR after operational expenses. I call that kick back and stack.
And its all based on the unnecessary misery of other people.
Anyway, the cure for opiate addiction is a drug that comes from the iboga plant
Its taken one time, under clinical supervision.
Its legal pretty much everywhere except the good old USA.
You can go to Canada or Mexico to take it under the care of trained medical professionals.
The name of the drug is… Ibogain.
Disclaimer. Im not a doctor or politician or scientist or salesman or any thing else of any significance, and as such, none of the stuff I write should be taken as medical, legal, or political action or activist advise.
In fact, everyone should completely ignore everything written here and just go on about living your normal, everyday, short lives. Politics as usual. Heads or tails, its all the same in the end.
Thank you, I appreciate this comment soooo much (and I’m being completely serious) I say this all the time and people never want to believe me. The fda is not for the people it’s all about money. There’s a whole documentary on YouTube about this doctor who literally spent his whole life and found the cure to cancer and it’s got literally 100% success rate no symptoms no harsh chemicals and the fda for decades had tried getting this guy in prison they’ve took him to court multiple times to say he was “illegally” treating people but they couldn’t get him and then when they couldn’t win they proceeded to steal his cure. The government in the US is so corrupt and will continue to be corrupt until the citizens get their heads out of their ass and wake tf up.