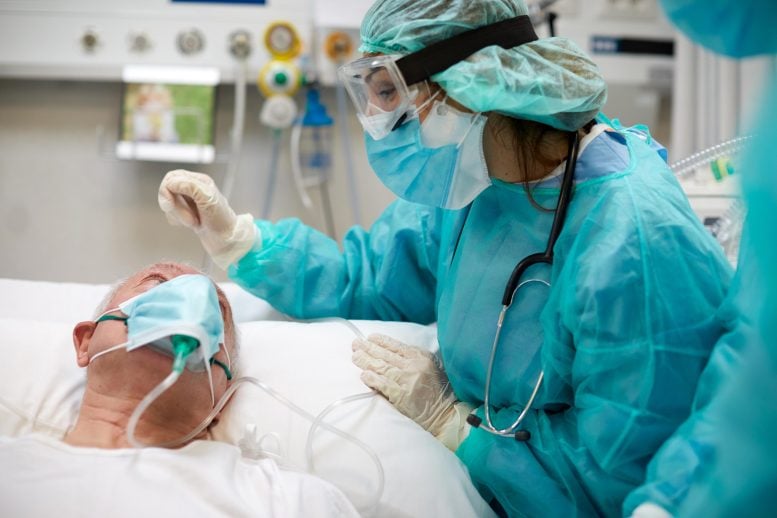
Brensocatib failed to improve outcomes in severe COVID-19 patients but showed a strong anti-inflammatory effect on neutrophils.
Brensocatib did not improve the clinical status of patients hospitalized with severe SARS-CoV-2 infection in the double-blind randomized, placebo-controlled STOP-COVID19 multicenter clinical trial, according to research published at the American Thoracic Society’s ATS 2022 international conference. Brensocatib is an oral medication being developed by Insmed for the treatment of patients with bronchiectasis and other neutrophil-mediated diseases.
The study, which began in June 2020, took place at 14 hospitals in the UK, where participants were randomized to receive 25 mg daily of brensocatib or a placebo for 28 days. One hundred ninety patients received brensocatib, while 214 received a placebo.
All patients in the study had confirmed SARS-CoV-2 infection and at least one risk factor for severe COVID-19, such as requiring supplemental oxygen. Individuals on mechanical ventilation were excluded from the study. All participants received standard-of-care treatment.
Targeting Neutrophilic Inflammation in COVID-19
“Treatments currently available to treat COVID-19, such as dexamethasone and anti-IL-6 antibodies, reduce inflammation, but their effect is not primarily on neutrophils or neutrophilic inflammation,” said presenting author Holly Keir, PhD, postdoctoral researcher, University of Dundee School of Medicine, Dundee, United Kingdom. “We performed the STOP-COVID trial to test the hypothesis that directly targeting neutrophilic inflammation by inhibiting dipeptidyl peptidase-1 (DPP1) would provide additional benefits to patients with severe COVID-19 on top of standard of care.”
Severe COVID-19 infection is primarily caused by an excessive and damaging immune response to the virus. A number of different immune cells are involved in this response, including neutrophils. Neutrophils release enzymes and other substances that cause severe lung damage. Studies have consistently shown that high levels of neutrophilic inflammation are associated with worse outcomes in COVID-19.
Brensocatib is an investigational oral inhibitor of DPP1, an enzyme responsible for the activation of neutrophil serine proteases.
Study Results: No Significant Differences in Outcomes
In STOP-COVID19, time to clinical improvement and time to discharge were not different between groups. Mortality was 10.7 percent and 15.3 percent in the placebo and brensocatib treated groups, respectively. Oxygen and new ventilation use were also numerically greater in the brensocatib treated patients. Prespecified subgroup analyses based on age, sex, baseline severity, co-medications and duration of symptoms supported the primary results. Adverse events were reported in 46.3 percent of placebo treated patients and 44.8 percent of brensocatib treated patients.
The researchers also conducted a sub-study at two study sites to directly measure inflammation in patients receiving DPP1 inhibition or placebo. They observed a strong anti-inflammatory effect of DPP1 inhibition on neutrophil protease enzymes. Active blood neutrophil elastase levels were reduced by day eight in the treatment group and remained significantly lower up to day 29.
“Although we did not find a beneficial effect of treatment in this population, these results are important for future efforts to target neutrophilic inflammation in the lungs. STOP-COVID19 is the largest completed trial of DPP1 inhibition in humans and we have performed extensive characterization of how DPP1 inhibition affects the immune system’s response,” noted Dr. Keir. “Using state-of-the-art proteomics (the study of the structures, functions, and interactions of proteins) we have already seen important changes in neutrophils with DPP1 inhibition that will help us to better understand the potential role of this treatment in other diseases.”
One of these diseases is bronchiectasis, where a phase 2 trial published in 2020 showed that brensocatib reduced the risk of exacerbations.
The STOP-COVID19 study was an investigator-initiated study sponsored by the University of Dundee and funded by Insmed Incorporated.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.