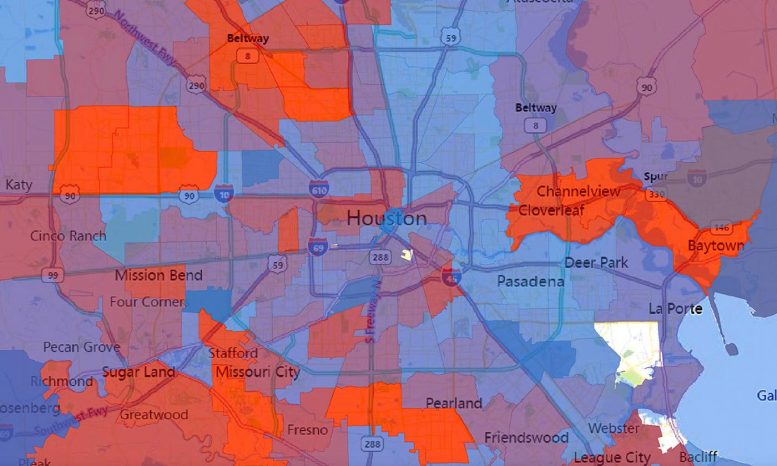
The number of virus strains present in each zip code in Houston during the second wave of COVID-19 cases in summer 2020. Number of strains is represented by a spectrum of colors from blue (0 strains) to red (50 strains). Credit: Houston Methodist/University of Texas at Austin. Credit: Houston Methodist/University of Texas at Austin
A study involving more than 5,000 COVID-19 patients in Houston finds that the virus that causes the disease is accumulating genetic mutations, one of which may have made it more contagious. According to the paper published in the peer-reviewed journal mBIO, that mutation, called D614G, is located in the spike protein that pries open our cells for viral entry. It’s the largest peer-reviewed study of SARS-CoV-2 genome sequences in one metropolitan region of the U.S. to date.
The paper shows “the virus is mutating due to a combination of neutral drift — which just means random genetic changes that don’t help or hurt the virus — and pressure from our immune systems,” said Ilya Finkelstein, associate professor of molecular biosciences at The University of Texas at Austin and co-author of the study. The study was carried out by scientists at Houston Methodist Hospital, UT Austin and elsewhere.
During the initial wave of the pandemic, 71% of the novel coronaviruses identified in patients in Houston had this mutation. When the second wave of the outbreak hit Houston during the summer, this variant had leaped to 99.9% prevalence. This mirrors a trend observed around the world. A study published in July based on more than 28,000 genome sequences found that variants carrying the D614G mutation became the globally dominant form of SARS-CoV-2 in about a month. SARS-CoV-2 is the coronavirus that causes COVID-19.
So why did strains containing this mutation outcompete those that didn’t have it?
Perhaps they’re more contagious. A study of more than 25,000 genome sequences in the U.K. found that viruses with the mutation tended to transmit slightly faster than those without it and caused larger clusters of infections. Natural selection would favor strains of the virus that transmit more easily. But not all scientists are convinced. Some have suggested another explanation, called “founder’s effects.” In that scenario, the D614G mutation might have been more common in the first viruses to arrive in Europe and North America, essentially giving them a head start on other strains.
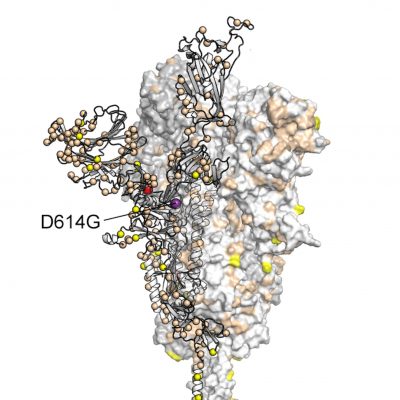
Most coronavirus strains circulating in Houston in the summer of 2020 had the D614G mutation in the spike protein. Credit: Houston Methodist/University of Texas at Austin
The spike protein is also continuing to accumulate additional mutations of unknown significance. The Houston Methodist-UT Austin team also showed in lab experiments that at least one such mutation allows spike to evade a neutralizing antibody that humans naturally produce to fight SARS-CoV-2 infections. This may allow that variant of the virus to more easily slip past our immune systems. However, it is not clear yet whether that translates into it also being more easily transmitted between individuals.
The good news is that this mutation is rare and does not appear to make the disease more severe for infected patients. According to Finkelstein, the group did not see viruses that have learned to evade first-generation vaccines and therapeutic antibody formulations.
“The virus continues to mutate as it rips through the world,” Finkelstein said. “Real-time surveillance efforts like our study will ensure that global vaccines and therapeutics are always one step ahead.”
The scientists noted a total of 285 mutations across thousands of infections, although most don’t appear to have a significant effect on how severe the disease is. Ongoing studies are continuing to surveil the third wave of COVID-19 patients and to characterize how the virus is adapting to neutralizing antibodies that are produced by our immune systems. Each new infection is a roll of the dice, an additional chance to develop more dangerous mutations.
“We have given this virus a lot of chances,” lead author James Musser of Houston Methodist told The Washington Post. “There is a huge population size out there right now.”
Several other UT Austin authors contributed to the work: visiting scholar Jimmy Gollihar, associate professor of molecular biosciences Jason S. McLellan, and graduate students Chia-Wei Chou, Kamyab Javanmardi, and Hung-Che Kuo.
The UT Austin team tested different genetic variants of the virus’s spike protein, the part that allows it to infect host cells, to measure the protein’s stability and to see how well it binds to a receptor on host cells and to neutralize antibodies. Earlier in the year, McLellan and his team at UT Austin, in collaboration with researchers at the National Institutes of Health, developed the first 3D map of the coronavirus spike protein for an innovation that now factors into several leading vaccine candidates’ designs.
The researchers found that SARS-CoV-2 was introduced to the Houston area many times, independently, from diverse geographic regions, with virus strains from Europe, Asia, South America, and elsewhere in the United States. There was widespread community dissemination soon after COVID-19 cases were reported in Houston.
Reference: “Molecular Architecture of Early Dissemination and Massive Second Wave of the SARS-CoV-2 Virus in a Major Metropolitan Area” by S. Wesley Long, Randall J. Olsen, Paul A. Christensen, David W. Bernard, James J. Davis, Maulik Shukla, Marcus Nguyen, Matthew Ojeda Saavedra, Prasanti Yerramilli, Layne Pruitt, Sishir Subedi, Hung-Che Kuo, Heather Hendrickson, Ghazaleh Eskandari, Hoang A. T. Nguyen, J. Hunter Long, Muthiah Kumaraswami, Jule Goike, Daniel Boutz, Jimmy Gollihar, Jason S. McLellan, Chia-Wei Chou, Kamyab Javanmardi, Ilya J. Finkelstein and James M. Musser, 30 October 2020, mBio.
DOI: 10.1128/mBio.02707-20
This study was supported by the Fondren Foundation, Houston Methodist Hospital and Research Institute, the National Institutes of Health, the National Institute of Allergy and Infectious Diseases, the Welch Foundation, the National Science Foundation and the Defense Advanced Research Projects Agency. Ilya Finkelstein is a CPRIT scholar in cancer research, funded by the Cancer Prevention and Research Institute of Texas.
An earlier version of the paper was posted in September to the preprint server medRxiv.




The lengths you will go to in an effort to validate the fake ass flu is unbelievable. You disgrace yourselves and invalidate your professions by continuing to pretend that 1. This was anything more than the flu.
And 2. That it was ever lethal.
The FACT is that NOBODY has died from it that would NOT have died anyway.
FACT: People have died from this. FACT: Theres the flu and then theres Covid 19. Shut up
Everyone should be copying this post and sending it to every email contact and social media contact they have so that your friends and family know what is coming with this poison they call a vaccine!
Here is the CDC link where they admit the “COVID” test may only prove that the recipient has antibodies from an infection with a virus from the same family of corona viruses that cause the common cold:
https://www.cdc.gov/coronavirus/2019-ncov/testing/serology-overview.html
It is found under this section:
If you test positive
A positive test result shows you may have antibodies from an infection with the virus that causes COVID-19. However, there is a chance a positive result means that you have antibodies from an infection with a virus from the same family of viruses (called coronaviruses), such as the one that causes the common cold.
Please be advised that the CDC test kits are faulty and are thus more than likely to find you false positive if you ever had a cold and/or flu!
The disgusting smirks on Bill and Melinda Gates in this 42 second video tells us they know the next phase of this plandemic will be 10 times worse and will get the attention of the whole world by this winter:
https://www.youtube.com/watch?v=ZmP6_gy-MIE&feature=youtu.be
Please watch this 2 minute video where Bill Gates himself explains his plans for your genome made up of your DNA and RNA:
https://www.youtube.com/watch?v=9BWHHxJuuUM&t=2s
If you think science has not reached the point where they understand how your genome works please watch this 3 minute video:
https://www.youtube.com/watch?v=YdjERhTczAs
Bill Gates in this 2 minute video hints that Moderna(modern ~ RNA) will be the likely producer of this vaccine which will require more than one vaccine to get you “cured”:
https://www.youtube.com/watch?v=9abpjSrQxAw
As they distract you with civil unrest, rumors of war, election chaos, and arguing over the relevance of face masks; they plan on beginning the process of changing your genome so you can be uploaded to the cloud called the world wide WEB:
https://www.youtube.com/watch?v=L0gNiICDmiE&feature=emb_title
The governments of the world will make this vaccine voluntary by next year and allow the corporations to begin shutting the doors on who can access their businesses to buy or sell if your not “vaccinated”.
“C.O.V.ID”=Certificate Of Vaccine ID!
Accepting their mark to operate in this world will be permanent so make your choice wisely:
https://sumofthyword.com/2016/10/04/the-rapture-of-the-church-is-after-the-tribulation/
Another Q-anon wacko
Please hurry your local psych ward is waiting for you
True that!
Sorry but I do not follow Q!
I’m gathering information from every Source I possibly can. Not just the ones you are suggesting. Just so you know.
Nowhere in your thoughts is there mention of tin foil or aliens. Obviously you don’t have a clue.
Rob is a blob!Bio U dumb! May Darwin claim your soul, the sooner the better! (That’s a reference to natural selection U dumbass!) Bye bye, see U in the morgue idiot.
I’ve had another type before and flu and colds plenty. I still test Negative . Hand washing and wearing a mask is my jam. I work in Sanitation.
Hey wacko, stop scaring people. May God have mercey on your soul. You have no idea what you are saying. You are pulling scriptures from here and there to suit your purposes. You need to read the whole passage to understand. Jesus says you will be held at a higher judgement because you are manipulating the word of God. I will pray for you. NO ONE PLEASE BELIEVE THIS POOR SOUL. HE JUST WANTS ATTENTION, BECAUSE HE LOVES TO CAUSE UNREST AND DIVISION, JUST LIKE TRUMP AND THE DEVIL
How can you say Coronavirus is fake? People are dying from it every day. I had a friend in New York who died of it this past summer. It’s not the same as the flu.
Why does something people don’t want to hear about always “ fake “ these days?
Sorry— always HAVE TO be fake ?
My post does not say that the corona viruses are fake! What it does imply is the FACT that the CDC, WHO, Bill Gates, along with many other “elites” have hijacked the corona virus to implement their global 2030 agenda. Ask yourself why this monument exists:
https://lastdaysglobalism.wordpress.com/2019/09/02/the-sinister-georgia-guidestones/
Myself and 4 members of my family were extremely sick. I stayed sick the longest. From December until May I coughed very very hard, non-stop. My 10 yr old daughter was second to get sick and
we had to take her to the hospital when her lymph nodes got very swollen and they tested her then for the flu. She tested negative. Never has anyone in my family experienced any illness like this before. We are all currently being treated for low vitamin D and zinc levels. These low levels likely contributed to the severity of our illnesses. I felt as if a thick sludge was sloshing from side to side in my lungs whenever I rolled over in bed. I had to sleep sitting upright. I used an oximeter to be sure all of our oxygen levels didn’t fall below 93%. We would start to get a little better at times, just to come back full force again. I had a viral rash from December to May. We suffered from severe sore throats, coughs, headaches, body aches,chills, fevers, visible eye lid twitches,
severe chest congestion and shortness of breath, diarrhea, nausea, dizziness and my toes turned purple a bit. It was an extremely scarey 5 months. God help you should you find out the hard way how very wrong you are.
Did you repeatedly test positive or were your symptoms from getting the virus lingering for all those months. Did you quarantine the whole time. I have much compassion. I have been suffering with numerous symptoms and tested positive 2x over past month. I am waiting for the results from 3rd test now. I am only half convinced it will be negative. I have some lingering symptoms that make me uncomfortable and have anxiety about returning to work.
You cannot rationalize with ignorance, fear, or hate. Almost 4 years of Trump should have taught everyone but the ignorant, fearful, and hateful people. Evil should have no place in America. Unfortunately we are being governed by them right now and looks like half of our population is behind the evil in charge. Pray that they are just ignorant like Germans that voted for Hitler and not truly evil like trump, Kushner and they Republicans that are enabling then to succeed.
you are another democrat baby killer with blood on your hands. all of you will face judgement by Jesus Christ our Lord and Savior!!
Well people are quick to Judge. No one said politics was perfect. Yes I am a Democrat but I do believe in the rights of the unborn and we should not kill after a heart beat after 3weeks. Look at the Republicans, they lie,cheat,steal,will do whatever to stay in power. Now God has judged the Republican party that’s why Trump is gone. With a indictment from the southern district of new York. All of you that support him. You condom his behavior by voting for him your hands are as bloody as his. I KNOW RAISE YOUR KIDS TO BE LIKE TRUMP. YOU WILL SEE YOUR KIDS IN JAIL
Wow ,Thank You for sharing Amy,It mostly hits older people and ones with sickness and disease, I guess that’s why most dont pay it any attention, To hell with those other folks seems to be the motto ,but perhaps when they are older ,Karma will give them a dose of what they are giving now ,I was born with a lung disease so I pay attention to the virus, if your obese ,or have diabetes, asthma ,copd ,or other issues that affect the immune system, you have to pay attention to the virus, and just not pay the naysayers any attention, they may get it and it be nothing more than a cold ,or it could be like what happened to youb,either way they don’t care and never will till they get a wakeup call in life.Im glad your family got thru it .I lost a brother who was very healthy and exercised a lot ,ran at least 5 miles couple times week ,and still it took his life
You might as well be talking to a wall trying to tell folks about the virus, they just dont believe it ,not to mention the conspiracy theories that are rampid on here .
Tell that to my coworker. Oh right, you can’t because she’s dead. Tell it to her three kids, then.
Why don’t u bring a*! to work with me one day? Then when the day is done, tell me what u think.
Nazi denier covidiot
Admit it, you’re terrified. Does it help you coming here to vent and discredit the scientific work being reported here?
The science is lying face masks do not work unless you throw them away each time you use them,when you touch your face or touch your face mask you will get the virus on your hands if there is such a thing!? As for me I believe in God and if this is God’s way so be it!! Godspeed and God bless!
God’s will? So many others in history have used God as an excuse to stand by and watch atrocities happen. This isn’t a holy sanctioned disease. Don’t label your will as God’s. Your not God.
Boi U Dumb
indeed ! Make up enough garbage and declare its peer reviewed. Love the Spike protein LMAOF ! I know they are LTAO at us for believing this BS
As you lay there dying all alone, I hope the last thing you remember is this asinine comment you just made. They buried my best friends brother yesterday who died of Covid-19. He had NO underlying conditions. Maybe you should tell him 3 children that were grieving the loss of their daddy of which 1 of his children caught it from him and was deathly sick for 2 weeks where she couldn’t even get out of bed. Just remember all of this when YOU lay DYING ALL ALONE!! MAY GOD HAVE MERCY ON YOUR SOUL!!!
Oh my God. The stupidity of people during this time has been flabbergasted me more than any other. But, somehow, you have become king of the Idiots. Congratulations and may Darwin claim your soul soon.
Since you obviously lack the basic comprehension skills needed to understand a plague:
1.Covid 19 is not the flu,learn to read biology book
2.Being male, automatically cuts your chance survival by 50%,dumbass(remember that plague that killed 1/2 of the world’s population of men long ago in egypt? This is it ,dumbass)
3.Did i say 50% of all men? That is right,half of men do not have the genetics to survive
4.this ancient bug targets your genetics, if you are modern neanderthal,you get repeated attacks until the covid19 kills you,that is correct,it will hit you until you die,this is proven,stupid people do not survive this.
5.Oh,also,i got two more words for you to try to comprehend,TRIAGE, BITCH,bcause you obviously don’t have the genetics.
“ONLY REAL WOMEN GIVE BIRTH TO REAL MEN”
I guess “faking it till you make it”
doesn’t cut it in the real world!!
Since you obviously lack the basic comprehension skills needed to understand a plague:
1.Covid 19 is not the flu,learn to read biology book
2.Being male, automatically cuts your chance survival by 50%,dumbass(remember that plague that killed 1/2 of the world’s population of men long ago in egypt? This is it ,dumbass)
3.Did i say 50% of all men? That is right,half of men do not have the genetics to survive
4.this ancient bug targets your genetics, if you are modern neanderthal,you get repeated attacks until the covid19 kills you,that is correct,it will hit you until you die,this is proven,stupid people do not survive this.
5.Oh,also,i got two more words for you to try to comprehend,TRIAGE, BITCH,bcause you obviously don’t have the genetics to survive this.
“ONLY REAL WOMEN GIVE BIRTH TO REAL MEN”
I guess “faking it till you make it”
doesn’t cut it in the real world!!
You out of you god dam mind !
Check out Johns Hopkin’s website, you really think everyone there is complicit in faking this disease? The numbers being reported from hundreds of countries around the world have all been co-ordinated? Come on…
A person with preexisting conditions have a hard time fighting the China virus !!!! I pray for others who have experienced the horrible effects of this virus , inflammation allover , terrible nerve pain , insomnia,short term memory loss, shortness of breath, fatigue, I’ve had the flu , you need to educate yourself !!!!!
I agree.
Fauxvid is a scam.
You insult those that have suffered and lost loved ones. What is wrong with you?
Thank you Andrew!! Bill Gates and his friends planned this from 2017. Now they are training people to get used to a socialist take over!
I you dont believe it just go to you local morgue.
Have you been living under a rock?
Well, you are certainly entitled to believe in whatever you want. That said, what about you? Do you have any hard verifiable facts backing your claim? Sounds like you’re just another conspiracy nut repeating other peoples unfounded accusations about something they know little to nothing about. Why don’t you go talk to someone who actually lost someone from this virus and get the facts strait from them. You shouldn’t have any problem finding someone. They are everywhere. Have a pleasant day.
Please do us all a favor and crawl back up Trump’s ass and don’t come out anymore. Your polluting the world with your selfish ignorance and stupidity.
The Wu-Flu virus was made in a lab.
It is man- made
A mutation is not possible it will stay what it was originally made to be.
The death rates per capita in Europe and the US are 700 times higher than in Asia because here in Asia we do not pretend that we are better at determining what actual science is than actual scientists. We don’t have a preference for focusing on whatever is convenient to our point of view. The scientists give us advice and we follow it because what kind of idiot would not follow their advice?
Well said. Thank you
There in Asia is where your commie “scientists” created the virus. Of course you listen to them without question. You don’t want to get beat with a bamboo stick.
You really do not pay attention do you?
Your correct. Man made cannot mutate.
Some of the information here in the comments are not correct. The Black Plague is caused by Yersinia. It is a gram negative bacteria . It’s annanaerobic microbe. Not a flu. Must have direct contact to acquire. Vector borne , zoonotic. Bubonic plague.
Remember the Ebola virus scare of 2014? OBAMA was ready to roll out martial law , etc .but the virus isn’t easy to acquire. It didn’t take . Whenever tptb want to experiment on population control the WHO heads towards the poorest parts of Africa. Just like the unrealized dreams of dead infants from the so called Zika virus , hopes of mass deaths through Ebola , etc,. People who are educated through Globalist mass media liars don’t realize the awfulness and depravity of the type of character these Globalists possess. They too are indoctrinated into believing a false doctrine. Mass depopulation is the first step into realizing their eternal Utopia here on Earth. It. Has been written about , and touted in academia, teaching a false religion of death , racism, and entitlement for hundreds of years. Through elitist universities , pupils just accept what is being taught as truth , thus taking with them through their lives and careers , and this ideal to implement the goals of the illuminated , so called educated , 1% of the world population , the most wealthy , and use that wealth to realize their Lucifarien dream of Trans humanist immortality on an Earth scoured of most , 92% of her inhabitants. So do you understand that it’s goal , the Beast system wants to depopulate the Earth of 92% OF us?… Whatever means necessary. The tentacles of this diabolical plan are many , so many it’s overwhelming to comprehend . The utter wickedness of this plan is incomprehensible to most people , because regular folks do not think in those kind of terms . So when these facts present themselves to us , we dismiss it as paranoid or impossible . It sounds crazy because it is . However , sounding crazy does not make something untrue .it just shows your instinctual revulsion to such an idea that is much easier to dismiss than to ponder and investigate.
This global tyranny is now upon us. By censoring our ability to obtain information , to purposefully lie using media outlets , to using our medical institutions , they will stop at nothing. Gates parents worked for Planned parenthood. No matter your stance on abortion , research what they have been caught doing . What motivated the founder of Planned Parenthood from her own words ? you must look deep , because there is a concentrated effort to rewrite and change , censure correct and factual information . Google will not help you , and will disinform you so don’t bother . You need to seek where there is open source of info , and many varied sources . The parable of ” those who have eyes to see will see , those who have ears to hear , will hear ” . This is in reference to understanding the hidden meaning of events played out in our world,past and present. Also , you will know them by the results of what they do . Fear is a liar , and controling people by outlawing their freedoms, their God given rights of free agency to do what one so freely chooses to do is overcome by a soulless entity that restricts freedom , imposes unjust laws , and covertly , cunningly, intentionally seeks to deceive you into submission.Offers up everything it can to distract and confound you , puts you to sleep and in flames your passions.Dull the mind and inflame your passions .. I wish it wasn’t so ..but there is no mistake here , this ‘system’has been the progenitor of all that influences the minds of those who think they know better than the rest of us , and will seek to force upon us their will , their ideals . We have been greatly deceived , through the epochs of time . Question everything . Deception counts on your ignorance of the truth. The outcome is very bleak if it does not stop . My hopes for this is almost nil . Take of it what you will. Government won’t and can’t fix this . Government is part of the evil combination to take your human freedoms away from you , and kill you.it’s what those 1% have been taught they are entitled to . Immortal life on Earth through technology and eradication of those who aren’t worthy to inherit the Godless Utopia as a counterfeit Garden of Eden.
So the fact that COVID-19 actually has been mutating disproves your hypothesis.
Viruses constantly mutate, as long as they’re reproducing, and the more people who are infected, the more mutations there will be. While this mutation happened early on, there have been lots of other mutations, most of them trivial, and fortunately none that seem to make the virus much worse for people who’ve been infected. And there’s been enough mutation to trace where the US infections mainly came from (Europe to the US East Coast, while Trump was blaming China.)
The excessive lockdown and quarantine procedures have resulted in the virus staying in the world populations longer and that longer period has allowed more mutations. Each mutation affects different subgroups of persons. If the virus had been let to run through the worlds population when it first came, only persons in the initial subgroup would have suffered. Now, many more subgroups will suffer.
You must be new to the world… Did they do they same thing for the black plague or.. Did people lock down and stay away?
Your herd immunity is really working for that one country in Europe /s.
Are you for real? Stupidest idea ever shared. You really need to do some scientific research yourself. Most uninformed yet
BS!
The planet is going to kill off the dumbest among us. The only problem are all the great people caught in between these idiots.
AGREED!!
More contagious comes at the benefit of being less lethal. When a virus doesn’t kill the host, it can spread more quickly. I prefer to focus on the fact that the virus is now significantly less lethal, even when accounting for how much more contagious it is. But of course politics is all about what we place the focus on. Science should not be tainted with politics, and it’s sad that so much of the scientific community are hell bent on manipulating public opinion than on doing actual science.
Look up the long term affects of coronavirus and you’ll see why the death rate is the least of our issues with a more contagious virus. Respiratory, cognitive, and circulatory issues to name a few. You say that the science shouldn’t be politicized but then you spread one Trump’s biggest talking points. If you want to tout science then read the damn science.
Though most singular celled platerplysims would like to beleive the virus is going to wipe out the majority of human life it is not certain to do so .. I would be more apt to belive in a great cataclisim to be the culprit ..the Earth will only sustain our existence on her terms no matter how greedy we may get or how we choose to profit from depleting her sustainability .. 🙏 Pray and God Bless the World and its people ..
4 of my family members, all had the coronavirus, it is real. Mine started around on December 15 2020. I had severe headache’s for 3 weeks, then the fever then chills, sweating. Nausea stomach problems, then vomiting & diarreahu. I have been having eye problems ever since symptoms started. Fatigue lasted for 5 months, & still have boughts, of symptoms. Loss of smell & appetite, countinues my mother died from the coronavirus she was 93. She was fine, then she started coughing, 4 days later she was hospitalized, & 4 days later we were told she was doing better & would be home in a couple days. Then we got the call she passed, my sister, myself & daughter were seriously sick. & Told not to come visit my mother. My mother was healthy for her age. My doctor said I couldn’t get the antibody test, cause I couldn’t have had the coronavirus as early as mid December, I did. Wear a mask when you go out, and don’t go out to parties, distance yourself. Anyone who doesn’t believe this isnt serious has oviously not lost a loved one or been sick from this. You feel like death has taken over except your still breathing.
Just use common sense, wear the mask, wash your hands (often) stay away from crowds of people. Dont be stupid, I have talked to people who have been infected and the virus is awful. Months of sickness death of loved ones of all ages and permanent injury ftom it. Thats good for me to believe its better to be inconvenienced and bored then sick and dying (or feeling like you’re dying)
This is no flu, people have Permanent health problems that will follow them the rest of their (probably) shortened lives!
I’d tell you a Covid joke, but 99.97% of you won’t get it!
Best comment of the day.
9-10.5 percent of the US population has already had it, based upon antibody tests. 236.5k are dead with an enormous death gap (look up death gap if you’re unaware). 350k will be dead by early next year, around 350-500k will die before we achieve immunity through vaccine,and spread, which may even be delayed further due to lack of confidence in a vaccine (Depending on what we do to impede this current wave).
Funny.
I had this all the way back in mid February. This isn’t just “a flu* like some morons out there espouse- this thing is a steamroller. It’s not a joke and not to be taken lightly, but instead it’s a serious illness. It laid me out and I’m in decent enough condition/shape.The fatigue, hardcore fever (especially after eating) , and overall lack of appetite were all pretty unique. This isn’t a standard flu which kills in the neighborhood of 30k a year, but will kill around 300k even with a modicum of preventative measures in place.
So, you survived…?
Trump voters in these comments I swear, y’all are brain dead please f*** off right into the sun
You realize it’s not just trump voters, right? It’s the young college age people (who majority are liberal and live carefree because they don’t know debt yet). It’s both sides on this bs. It’s people in general who dont care… Look where the major spikes are happening again. Everywhere in the US including “majority liberal states”. Again, it’s both sides.
Just look at everyone who partied on Halloween including the hollywood stars, mask free.
You are on point. Well said. May truth prevail. Stay well.
Trump 2020 bitch, deal with it
Just stay inside your house clutching your toilet paper like the coward that you are. We’ll let you know when it’s safe to come out.
One Doesn’t have to be a Trump fan to mistrust the Covid caper weaponized for top down control. Similar to the surveillance and controls controls implemented after false flag 9/11 with the PATRIOT ACT to keep all the terrorized minions “safe.”
IF the commenters on this site had such episodes of catastrophic illness as they described here diagnosed as COVID, why weren’t they immediately hospitalized? Apparently none of them were? It sounds like they were at death’s door, but they werent put in the hospital??? And here we had surgeries cancelled and a lockdown extending past the original two weeks to months and months to supposedly “flatten the curve” so as not to “overwhelm” the hospitals (many of which stayed
nearly empty) based on a dumb*ss model numbers projection that was WAAAAAY off from a prognosticator who had a poor previous track record. Bad fallout from locking down EVERYONE. But HEY! IT didnt get rid of the terrible horrific virus like it did the ECONOMY, now did it?
Now apparently The sky’s the limit as far as new “STUDIES” and “scientific projects” involving thousands of test subjects DIAGNOSED with the “novel” coronavirus, coming out of the woodwork from as far back as early last spring when they hadnt apparently even isolated the virus yet. The thing was barely off the ground then and now all these new studies from that time are coming to light?
There are lots of people out there in addition to Dick that apparently will believe anything at all as long as it has the label “SCIENCE” attached to it. Maybe that’s why all these “STUDIES”are suddenly being unearthed from 9 months ago and publicized with considerable hoopla? Evidently
“ITS EASIER TO FOOL FOOLS THAN IT IS TO CONVINCE FOOLS THEY HAVE BEEN FOOLED.”
Its the end of times not all of us will make it pray
The virus is real folks
I am a nurse in Illinois at a skilled nursing facility. I do the covid testing on 110 staff every week,and on approx 105 residents once am month. I have been doing this since February. In that time 5 staff and 3 residents had positive results. No one had any symptoms at all. The 3 residents were in their 80s and 90s. They are all still alive. I guess we are lucky to have come into contact with several very weak viri.
Polity that the average American lacks a college degree yet thinks he/she is more qualified than a trained virologist. God help you poor fools.
You are so correct. Well said.
You need to stop writing all this bulls*** that scares people. DO You want to wear a mask for the rest of your life? You contribute to bankrupting business, crippling the economy and causing tHe cost of living to skyrocket! Stop it already!!! How do you sleep at night? You’re not helping anyone by writing content that creates fear.
You’re an idiot. Businesses are recovering, even in areas with rules and the ones that aren’t are due to the governments inability to look past party lines in the middle of a pandemic to appropriate relief. States and countries handling the pandemic have clearly shown simple things followed (Social distancing, esp in enclosed areas, masks, and not gathering in large numbers, esp indoors.) You’re response lacks logic, and screams drama. Grow up. You don’t have a wear a mask forever, you have to wear a cloth on your face for between 6-12 more months (Only when in public, inside, gathered with strange people). You’re a child. Have some respect for 40% of our population susceptible to strong forms of the virus.
Can the world get a break??? This is demoralizing…..no good news at all. We need people who can handle this.
Wow
Hahaha…buuuulllllshhiiiiiit. “experts” “scientists”
This is all bs. Talk to the virologists…the ones who actually work with these viruses and they’ll tell you, mutation rate is extremely slow, no deadlier than the common flu, easily treatable, masks do nothing to do contaminants, hard to contract, not airborne, etc. So lying to fear monger the people into a new normal designed for a political agenda.
Stop*
I truly appreciate your sense of humor and for speaking up the Truth!
Bravo! Respects
A M E N !
Trump 2020 !
Vote for your peace of **** draft dodger he only cares about donald an that he has proven himself!!
I know it’s real! I don’t care who wins election. I live in a neighborhood where I see PPL not following the rules and it makes me very sad. Soon they will be dying..I stay away at home and I think my husband and I had it from end of February until June and lungs (sob) just stopedp a month ago Oct..yup!! But the testing wasn’t great when we got it so we will never know..we take no chances. I’m in 50s husband in 60s..it angers me about kids in Uni too!! Plus my community are PPL 50 and over!! No one wears MASKS outside either!! I see them invite everyone in community in their homes w/o MASKS. I’m disgusted..so I’m on no side but I see PPL from all walks of life acting uncaring about everyone. Only caring about themselves.Where is the love. I am so sorry to those who have lost loved ones!! We’ve lost our hair..rashes..appetite. And more…I guess we are considered weak and dumb…I was upset when I heard young PPL say on news shouting “let the weak die”…well type A blood PPL are not weak they have something different in their blood..read ppl…about the virus and learn to protect your brothers and sisters and what about the elderly..come on!!!.I only ask, what you’d ask if you’d been hit w it.
So sorry if I sound angry but I am watching PPL hate each other and so divided…I blame that on PPL we all have choices to make..but love your neighbor and at the end of the day agree to disagree..but lives matter all lives so we should care and be caring to others no matter what!! And sorry I typed name wrong..its Tess not Tests …omygoodness!
I find it tragic that so many fellow humans are hell bent on mass suicide and murder by denying reality staring them in the face. and typically being very nasty radical know-it-alls in their response to Truth, vilely attack all who work hard to understand this new disease in an attempt to help humanity. sadly and ironically many of these same people claim to be conservative, highly religous God fearing people who’s religion is supposed to be based on peace and love yet who would rather believe false prophets, who profiting off their ignorant, but not stupid, flocks entertain mad hopes of a second coming. the Truth is far deeper and infinitely more mysterious than anything written in their blood-stained blackbook,for each and everyone of us is the Savior – that is if we are brave enough not to follow the corrupted path but to peer into the very depths of our own soul to see that we are all one.
Bravo
Do not buy into this covid bs they are taking about now. It’s not becoming more contagious . This is all planned . It’s in a file on the Rockefeller website in a report on guidelines and outcome of a global outbreak. If this virus was as bad as they say it is like from the beginning we would all be dead by now . The entire human race would have been wiped out if it was that deadly and contagious . The report states that during this time this year they were going to increase hype over the virus to put fear in the population and lock us all down again .. it’s bull s*** it’s a lie .. don’t fall for it .. f*** off bill gates
Real virus, fake pandemic. Change my mind 🙂
Nice add on to the featmongering. Since mutations make vaccines ineffective the government will have no “choice” other than to put further controls on people in order for them to be “safe”.
Viruses mutate when they’re not controlled. It’s science not fear mongering you festering wound of a person. If you don’t want the science don’t read the article.
Got a different rare virus 30 years ago and I’m still fighting the effects, one being extreme fatigue everyday, so it’s hard for me to understand how a person thinks this is the flu. A virus is no flu. I know this first hand. Mine left me paralyzed.
The flu is also a virus; its effects on humans (and other animals, such as pigs and birds) depends a lot on how similar it is to previous flus that their immune systems have dealt with before. COVID-19’s a generally nastier virus, and (along with SARS and MERS) one that humans have much less experience with (though some coronaviruses include the common cold.)
But yes, the “It’s just a flu” is deliberate disinformation, whether by Trump’s fear that if there’s a serious problem he couldn’t handle then the voters won’t respect or re-elect him (so it must not be serious!) or by other groups who think it’s advantageous for Americans to disrespect science and also get sick and die.
In 2000 my wife died from an unknown VIRUS. It took a year and a half to kill her. She was f***ing tough. Pray that this virus don’t turn into something horrible. I’m not trying to scare any one. Just enlighten. Conspiracy theories dime store novels it’s entertaining.
I’m so tired of all the “it’s fake” people putting my life at risk! How can you be so dense to think that this is something to steer the American election. Its hit every country in the world. Open your eyes and ears. No wonder that Americans are hated by everyone. You actually believe a worldwide pandemic was created to influence one country’s outcome. Total arrogance. Arrogance that’s slowly wiping our country out. The virus is real! If you think China created this to hurt us then all of you that do nothing to protect yourselves and others are only helping. What’s the issue with wearing a mask? Do you all think your so great looking we need to see your face? It really all comes down to American arrogance. “F the others I’m going to do what I want”. This virus isn’t political, it isn’t social, its medical! Time to start treating it that way.
Dear, you ARE waring the mask and probably gloves…SOOO you are protected and safe. Stop worrying about those, who educate themselves about the risks and choose NOT TO! Many of us DO NOT watch CNN and live stess free lives. I suggest to you : – TURN OFF tv for a few weeks and things will start making more sense. Best of luck!
You didn’t educate yourself about risks. You listened to an Orange Tyrant lie to you about it’s effects and you believed him because it’s too inconvenient for you to consider the wellness of anybody but yourself. YOU can still spread it to other people if I wear a mask you jackass.
Rasa, just your one comment about “wearing a mask and your safe, so it’s ok for others not to”, just proves your ignorance of science fact. Unless you’re wearing a fitted N95, the mask you wear prevents you from infecting someone else not the other way around.
Here we go with “The sky is falling” BS again.
Give it a rest.
I am not going to take unnecessary chances with my. health. I can’t afford to. No one can really. 1) I am elderly and 2) I have COPD. I stay away from crowds, I wear a mask wherever I have to go, and I wash my hands numerous times a day. I just got a flu shot too as another layer of protection because of my age. I am also following the 6-foot- distancing rule. It makes sense to do whatever you can to protect yourself and others’ health. Why take foolish risks? The virus does mutate. It is very contagious and it is deadly. Please heed the warnings.
Divide and conquer, made super easy with generations of x box infused idiocy. When you live in fear your brain quits working normally. We can’t unite when we are fractured apart. I’m not a conspiracy person. Just a guy watching American self destruct.
My wife died in 2000. From an unknown very aggressive VIRUS. Our son was 8. All you non believers better get on your knees and pray this virus don’t turn bad. She died horribly. Took a year and a half. A VIRUS
The Corona virus is the flu like all flu’s such as H1N1 and all the ones that came before it you get body aches, fever etc. and if you’re not in good shape you can die from it. The total number of US deaths versus the total number of people in the US is less than significantly less than 1% of the United States population. While this fact provides little comfort to those now suffering or those who have lost people it is nonetheless a fact. Moreover because it is a virus it mutates constantly a single vaccine will not work against all possible strains of it just like with the H1N1 viruses. Additionally it should be noted that no politician no matter what the level of government is going to legislate the virus out of existence. Like AIDS and stink bugs both appear to be here to stay.
Carjackson and you received your PHD where?
As a medical professional all I want to say is: SHUT THE F*** UP! YOU UNEDUCATED Ignorant MORONS. IF YOU DON’T BELIEVE IT EXISTS THEN COME WORK IN THE HOSPITAL WARDS. WE NEED PEOPLE TO CLEAN OUR COVID ROOMS AND TRANSPORT THE SICK, ETC…
What did you say?-oh that’s right YOUR TOO AFRAID TO EVEN HELP!!!!
SO…..SHUT THE F*** UP
If I do not wear a mask and you do wear a mask how am I endangering you? If the mask protects you the only person at risk is me, right?
The fact that people act otherwise is proof that the propaganda behind this is working. Use your head and think about the rules and regulations they have implemented. Much of it makes no sense.
Again another moron who doesn’t know his arse from his head. Have you NOT been listening to the mask information put out??? Masks prevent YOU from spreading it!!!
Oh my lord, I am so suck of stupid ppl
Donald J Trump is responsible for the manufacturing of covid-19 him in the Chinese. They’re making a fortune off items you need to protect yourself.
Congratulations…you win the “dumbest” comment on the Internet today 11/2/2020!
Really, that one’s pretty special. If Trump had taken the problem seriously instead of denying it for months, he could have sold $100M worth of $20 MAGA Masks to his followers, deaths would have been an order of magnitude lower, and he’d look like the strong leader his followers thought he was when they elected him.
Your method of “taking care of others” has created the largest epidemic of mental health to date. You are not saving lives, you are causing suicides and depression and life that feels as if death from Covid was the better option. Those suicides could have been prevented, while the current science on Covid was only ever designed to slow the spread, slow the inevitable deaths. You claim to “love others” by protecting their health, but I’m telling you that you are causing (I hope unintentionally) preventable deaths for the sake of unpreventable ones. You might say the mental health epidemic was before Covid, which it was. It was because your rhetoric of “loving others” has always been based out of your own self interests rather than a true love for others, you’ve been trying to use this rhetoric to force others choices for a long while now. You hurt way more than you help when you try to control someone else’s situation. Let each person have their own responsibility which in turn leads to their own consequences and get your own biases and beliefs out of the personal life decisions of others who hold different beliefs than you. Otherwise you create a life you would choose to live for someone who would never choose to live that way. Regardless of how well intentioned the choice, forcing it will always have a negative effect. Law is based on preventing consequences of one person’s actions from affecting another which is why murder is looked at as evil, one person’s actions having the ultimate price on another’s life. Covid was inevitable but your laws to react to it are actually “murdering” others. The “law” and accepted rhetoric of “taking care of others” has actually been so backwards as it is a law designed to have consequences on others! So stop murdering people with your stay home, mask up, and stay away from others “law” that is causing more problems than Covid ever could on it’s own. I don’t need two epidemics, I’d be fine accepting just the one and waiting for science like from this article to get us to a greater understanding of Covid and to a vaccine, an actual solution. Thank you, sincerely someone who needs you to truly love others and not just yourself.
dear anonymous animal, sure forget you’re a human and remember you’re a dirty rat in a dirty rat race and all that matters is your bank account [which will be worthless] forget about all the people that tried to make you into a real human being go on being the lowest of the low and then when you need help one day and are spurned by neo-darwinian dregs [like yourself] remember you’re just dingleberry on a worm and deserve no more
Omg Anonymous, go back to the 69s, the hippie movement is over
They forgot the,”and less deadly”, bit…
You’re a dumbass.
And yet we can’t get Hydroxychloroquine in this state! Nor is there a home treatment protocol in the US! But there is in Greece, India and Bangladesh!!!
Trumpanzees please continue to attend your Nazi rallies….and spread the virus amount you…Yes all a liberal joke….I’ve know of 2 that have died one was 73 the other a 44 year old women who was in perfect health lasted 16 days before dying….right now a 41 year old male has it I know of and said he feels like crap and has a nasty cough…..I’m 63 and in poor health and stay inside for weeks at a time….I’d rather be bored than dead
If the CDC and the FDA (Among others) admitted that they never isolated the “Virus”, what exactly are they testing?
For all who do not know it can get into the eye ducts as well so why arent goggles stressed to wear like masks. Smh.
Two reasons –
– The primary protection masks provide is to keep mask-wearing infected* people from exhaling droplets near you, not to protect mask-wearing you from them. Yes, especially if you’re a medical person around lots of infected people, the masks and goggles and gloves and other surgical barrier are important, but goggles aren’t going to reduce the amount of virus infected people spread.
– Most of the transmission is respiratory, through exhaled droplets. Yes, it’s possible to catch it through your eyes, or skin, or airborne non-droplet transmission, but the vast majority of cases and much higher probabilities of having enough virus cells reaching susceptible cells in your body aren’t from those, so masks are the main protection for you.
Actually John, in the hospitals everyone IS wearing face shields AND masks. And at my hospital ALL staff have been wearing both. It’s been well known in the most informed circles, who by the way, believe and take science seriously, that covid can be spread airborne like TB. Not our fault idiots won’t listen to science.
What really bothers me about this story is that the headline leaves one to believe that the Corona virus has recently mutated to become more contagious. When you read the article what you find is that the mutation that they are talking about existed from the beginning. It’s only become more prevalent because it’s more contagious. It’s not a matter of the virus actively currently mutating. Which it probably is doing that all organisms do.
Now looking through the comments here I see some people have making the claim that no one has died from this virus. I’m not going to make that claim. But if you look at this from a purely objective perspective and you look at the high incidence of other causes of death listed besides Corona virus then what you find is that the cases where only Corona virus is listed as the cause of death is lower than the cause of death from the seasonal flu. I believe the official CDC statistics is that 94% of deaths in the US that have Corona virus listed as a cause of death also have something else listed. That to me says that this virus has been overhyped. And when you look at the way our freedoms are being taken away and that much of the age of the same things that were attempted under the guise of 911 yes I do believe that the people who really control this world are trying to manipulate this.
99.9% survival rate .
Fact, covid was developed as population control.
Fact, the earth is overpopulated
Fact, EVERYONE ON THIS PLANET WILL GET COVID, just like everyone has has a common cold.
Request, please let this thing do what it’s intended to do. THIN THE HERD
I like this. Makes sense. Man mightve created it but mother earth/god whatever made man. Looks like she/he came up with a vaccine of her own! 😆
Are you ready to be “ thinned ?”
Hatred. Thats all I see here. People that once upon a time cared for each other. I wouldnt give a crap if it had a 50% mortality rate, I wouldn’t loose my humanity over it. I respect everyone’s beliefs whether I think its stupid or not. I didn’t grow up in their shoes. Secondly, I’ve been wrong more than I’ve been right in my life. The people you hate live on unaffected but the haters soul will be taxed and collected.
Self Destruction… Hard Words that TRADUCES The Core Fact of The Moment we’re living now: As Human Beings we must take conciousness and action Without political
or conspiranoid manipulation of People, Unite Ourselves in A Human Society of Logically Feared Persons at Risk of Death (Assuming our Fears and Trying to Drive Them The Best we can) and Plan An Strategically Thinked Act and Decisions for our Survival of our Human Specie and don’t carrying so not sense Partisannism of the Elections (Will Biden or Trump be responsible for our Wealth and survival of our Survival?).
The News I’ve Been Keeping After This Words of Hope is That What We’re Found as Research Group : You Must Know That Cuban Admixtured Population is Well Known (Indigenous From Early Migration from Pacific Ocean Coasts of Mexico that migrate to Northern South America as of part of the Actual Guyana, Venezuela and a little north From Colombia) African Admixture (During The Selling of African Slaves,Near to 1.4 M of Them) and The 900 K of Chinese Slaves, in both Trading, Europe Slave Traders.
A recent Research (And others in the past years since 2008) have stated that the Admixture of Races as Complex to Understand and Probe.
The last One Found in 2018 That Admixture was Biased in Men and Women (More European Blood Types in Men and Mora African in Women, Based on Mitochondrial DNA(Mother) and DNA From Y Gene (Father). Lesser are the genetic traces of Asiatic and Other Ethnic Groups.
Can you See the number of Contagions and Deaths That are Taking maybe All The SubSaharan African Countries, Venezuela and Guyana?… QUITE OUTSTANDING !!!
The stress you all are going through gonna take more than the virus
We still are only at the Germ Theory of disease level ?
Most everyone just accepts that an early 19th century idea floated by Pasteur is a proven fact. Why are there only images of viruses and not photomicrographs ? answer; its impossible to view them and a TEM is not able to nor an SEM because the process itself would obliterate a tiny organism due to the high tor vacuum and the heat of the electron beam. This after you’ve successfully isolated the virus in the first place. another highly questionable feat. After all how do you isolate what you cannot see and or verify its presence alone. Science, not wacky ideas and religious like faith in those unproven ideas
How do you think the pictures were taken? God I hate people who think they’re smart
Hahahaha Professor, best response ever
Editors – Your comment section is being abused by the “Covid is fake” weaponized disinformation groups. Please clean it up.
It would also be helpful if you could identify the locations the fraudulent posters are posing from.
“fraudulent”, because they don’t agree with YOU…because YOU are always right and any OTHER OPINION IS WRONG! So “remove the comments that I don’t like” is your DEMAND! Lol, you fit right in with the politicians you support…they believe in the same “totalitarian tenets” as you! Yet, Trump is called the “nazi”, “fascist”, etc. The “projection” and “hypocrisy” coming from you fools is entertaining!
Oh Bobby, Bobby, Bobby. It has nothing to do with opinion LMAO. It’s about science and facts. Go back to your cave.
This fearmongering from an “Alleged” Science publication….the Left has bought virtually all of the “journalists” and some of the scientists! Scientifically, most of this is probably accurate, but what’s glaringly absent is: “who cares, virtually nobody is dying anymore!”
We don’t need fearmongering, we don’t need a vaccine, and we don’t need any shutdowns!
We’ve all heard the tapes of Trump saying how deadly Covid-19 is and that it’s airborne …. so was he lying then or is he lying now???
More overexaggerated fake democratic propaganda.
Another stupid trumptard parroting his great leader
If you’re stupid enough to follow a xenophobic homophobic racist conman…….
The Chinese are laughing!!
I think we should send this new virus mutations back to China they’re the ones that created it let them suffer the same casualties
This virus was created in the lab in Wuhan China. Time to phase out all trade with Red China and leave Red China a pariah Nation. Also deduct the cost of this virus damage from the amount of debt that we owe Red China. Let them stew in their Wonton juices.
Stop the fear mongering.
Jesus people the mask STOPS you from spreading the virus. So if you have the virus you can spread it to people WEARING the mask. So stop being ignorant and wear the mask.
Funny, just when they began rolling out 5g, huh?
Blathers, They’re looking for you in the museum. I think you better leave scientific evidence and facts the the REAL scientists
Why don’t you leave the facts? No hospital investigation, no verified body counts, they had to close up the tents months ago because nobody showed up sick. Test kits are 90% false positives. Hospitals are all dead around me. No wambulance from people shaking and falling on the gound like in China to SCARE ya. You hear only TURD party reports of so-called deaths.
More likely is that this not do novel, novel coronavirus was made more contagious, and made to jump species easier, through the recently banned in America “gain of function research” that Dr. Fauci did to it in the Wuhan lab, with your tax dollars Obama gave to the program.
Hahahaha omg..their coming to take you away haha heehee, their coming to take you away haha heehee. To the funny farm where life is sweet all day long ……..
What is most interesting is the current research being done in these responses to human suffering. What becomes most apparent is one group of responses obviously has not had a family member or acquaintance who was in good health Day-1 and died Day-5. Otherwise, I know of no one in generally good health who succumbed to death in 5 days due to the common cold or flu. Remember the grieving who knew the health status and pray that we are all ready for the next level of Pestilences. P.S. Man-made sugar lowers the immune system. So we should look for an unprecedented number of young people and children entering the grave due to the Holiday sweets/sugar laden foods. Let’s all get knowledgeable about good health and nutrition and by the way encouraging the grieving tends to better health.
EVILDROID:appropriately named. Definitely one of the healthcare professional legions brainwashed by the MedicalPharmaceutical Cartel. You can tell by the way he makes fun of and namecalls everyone who refuses to genuflect before weaponized “SCIENCE” Namecalling is the last resort of someone who has nothing better to say. So very professional
Says someone who’s not in the trends, so to speak. So shut up and go back to your cave, and leave the rest of us alone!
Trenches, not trends.
Stay home, stay masked, stay clean and take vit D and don’t waist energy arguing with idiots.
Fear mongering. And it’s all Trump’s fault. Even when all these so called experts dont know what’s going on. Constant changing their minds. Chinas fault. 188 countries.
Trump all the way!
The above bus what democracy is made of, the salient issue is states’ rights and so many have died for that…
But this is a war. FYI TAIWAN in early Dec. Got whiff of Wuhan and sent people byo China..who immediately locked down their country. Today 7 deaths, less than 500 cases, no new cases in 200 days BUT ABD READ THIS A $300,000 USD FINE FOR NOT WEARING A MASK
Is that interesting? Is that evidence? It is not politics …IT IS THE TRUTH
Science is what should inform influence and guide policy not ignorance and greed.
Yes, the number of covid cases has increased but if you do your research the death rates are down significantly because we have effective treatment. People will still die because some people have multiple comorbidities that make their overall immune system weaker. This is the same as the flu. I will not be receiving a vaccine once it is available. Keep yourself healthy. It’s funny that the same people who are generally against vaccines in general are all for this one.
All you people should go back to bed and stay there.
I would also like to remind everyone this is typical of a democratic stand. Scare everyone into submission so we can get what we want out of them. Another lockdown will kill more people than coronavirus. Please do your families a justice and vote. It is crucial to our lively good. Nothing is free and whatever they offer you for free; food stamps, unemployment, healthcare, ECT, all comes at the cost of people who work hard to keep they’re families afloat. The people who make minimum wage and make too much money for assistance, because that makes sense!
Millions spent on controversial study that only 50 % agree on lmfao. New scientific study millions spent have proven friday comes after thursday. These boundaries nknow no limits.
How many are following this train wreck for entertainment value or to validate our lack of faith in humanity? Our neighbors only have their own backs. You can’t change someone’s opinion by belittling them or trolling. F***ing hilarious! I came here hoping to find something positive and I have read some things that make sense. Thank you!
I recognize the stress we are all experiencing for SEVERAL reasons and the references to increased suicide rates bc of the ‘shutdowns’, but where are the actual statistics of suicide v COVID fatalities? All l have seen are threatening references, but where are the numbers?
If staying apart or isolated from others for a set number of days IS a legitimate way to keep us safe (and l believe it is), l would like to know how many have suicided and the rate of increase since restriction…or bc of the stigma of suicide, do we have any actual facts?
I recognize the stress we are all experiencing for SEVERAL reasons and the references to increased suicide rates bc of the ‘shutdowns’, but where are the actual statistics of suicide v COVID fatalities? All l have seen are threatening references, but where are the numbers?
If staying apart or isolated from others for a set number of days IS a legitimate way to keep us safe (and l believe it is), l would like to know how many have suicided and the rate of increase since restriction…or bc of the stigma of suicide, do we even have any actual facts? Could it be hyperbole?
I just read ur comments out of pure comedy. Everyone is allowed to have their own opinion. Why belittle eachother if they believe in a certain thing. Fact is nothing! No one knows if anyone is telling the truth these days. It’s the world we live in. Sad but true. God can’t save u. Cuz he really doesn’t exist. But if u want to pray to “him” so be it. Everyone needs to mind their own business and quit watching the news!
Foreign troll alert!
Gotta couurption problem in data analysis? —- you pay me.
I think by now everyone knows, That this is a real contagious virus
Yeah, retro viruses mutate. What else is new? Total bs from start to finish. Media and politically-driven crap and resulting panic by ignorant, uneducated populace, nothing more.