Research has found that a popular weight-loss surgery, sleeve gastrectomy, negatively impacts bone health in adolescents and young adults. Two years after surgery, although patients’ BMI significantly dropped, bone marrow fat increased, and bone density and strength reduced. The research highlights the need for monitoring and managing bone health post-surgery, potentially informing novel therapies.
A common weight-loss surgery for obese adolescents and young adults is found to have harmful effects on bones, according to a study published in Radiology, a journal of the Radiological Society of North America (RSNA).
“Childhood obesity is on the rise and weight-loss surgery is the most effective way to reduce weight and improve cardiometabolic comorbidities,” said the study’s lead investigator, Miriam A. Bredella, M.D., professor of radiology at Harvard Medical School in Boston, Massachusetts, and vice chair for Faculty Affairs and Clinical Operations, Department of Radiology Massachusetts General Hospital in Boston. “This is the first study in adolescents and young adults that examined the long-term effects of sleeve gastrectomy, the most common type of weight-loss surgery, on bone strength and bone marrow fat.”
Sleeve gastrectomy removes approximately 75% to 80% of the stomach to restrict food intake and induce weight loss. It results in a typically round stomach taking on the shape of a tube or sleeve. The estimated number of sleeve gastrectomy procedures performed each year increased from over 28,000 surgeries in 2011 to over 122,000 in 2020, according to the American Society for Metabolic and Bariatric Surgery. Sleeve gastrectomy has overtaken gastric bypass as the primary weight-loss operation.
For the study, participants between the age of 13 and 24 years were enrolled from 2015 to 2020. The adolescents and young adults had moderate to severe obesity. The young adults had a body max index (BMI) of 35 or above. A BMI of 30 or above is considered obese. Adolescent participants were at 120% of the 95th age- and sex-specific percentile.
There were 54 participants, 25 who underwent sleeve gastrectomy and 29 who were in the control group. Forty-one study participants were female. The surgical group included participants with at least one obesity-related co-morbidity, or a BMI at or above 40. The control group had obesity but did not plan to undergo sleeve gastrectomy but received dietary and exercise counseling.
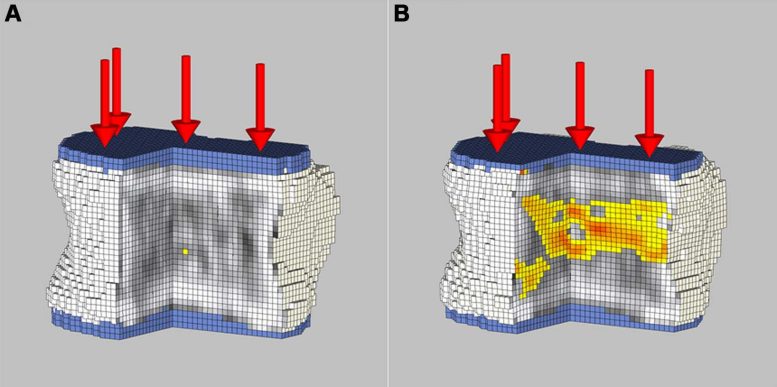
Before and 24 months after sleeve gastrectomy, participants underwent a physical examination, blood tests and quantitative CT of the lumbar spine, to quantify volumetric bone mineral density and to perform finite element analysis, a technique that can estimate bone strength. Quantitative CT is a highly accurate technique for detecting changes in volumetric bone mineral density after extreme weight loss.
Studies have shown that bone marrow fat responds to changes in nutrition and may serve as a biomarker for bone quality. Therefore, patients underwent proton MR spectroscopy to quantify bone marrow fat of the lumbar spine.
Bone Health Impacts: Weakened Strength and Increased Fat
Two years following surgery, BMI in the adolescents and young adults dropped (-11.9, on average), while there was a slight rise in BMI in the control group (+1.5, on average). Compared to the controls, sleeve gastrectomy patients had a significant increase in bone marrow fat and a decrease in bone density and strength estimates in the lumbar spine.
“We found that bone strength was lower two years after weight-loss surgery, while bone marrow fat, a marker of bone weakening, was increased, suggesting that weight-loss surgery has negative effects on bone health,” Dr. Bredella said.
Dr. Bredella points out that the adolescent years are a critical time for building up bone mass, and deficits in bone accrual during these years could have a long-term impact on bone health and fracture risk in this younger population later in life.
Long-Term Health and Physician Awareness
“As bariatric surgery is increasingly performed in adolescents, its effect on bone health needs to be emphasized, especially to the physicians who will continue to provide routine medical care for these patients,” Dr. Bredella said. “We hope that our study will raise awareness on the effects of weight-loss surgery on bones in adolescents with obesity.”
Raising awareness of the importance of bone health will allow for monitoring and management of low bone mass, optimal dietary supplementation with vitamin D and calcium, and the initiation of appropriate therapy, if necessary, Dr. Bredella noted.
“Our observed effects of weight-loss surgery on bone strength and bone marrow fat might also identify new targets for novel therapies,” she said.
Reference: “Two-year Skeletal Effects of Sleeve Gastrectomy in Adolescents with Obesity Assesses with Quantitative CT and MR Spectroscopy” by Florian A. Huber, Vibha Singhal, Shubhangi Tuli, Imen Becetti, Ana Paola López López, Mary L. Bouxsein, Madhusmita Misra and Miriam A. Bredella, 13 June 2023, Radiology.
DOI: 10.1148/radiol.223256
Collaborating with Dr. Bredella were Florian A. Huber, M.D., Vibha Singhal, M.D., M.P.H., Shubhangi Tuli, M.B.B.S., Imen Becetti, M.D., Ana Paola López López, M.D., Mary L. Bouxsein, Ph.D., and Madhusmita Misra, M.D., M.P.H.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
3 Comments
Thank you for sharing this valuable article highlighting the potential impact of sleeve gastrectomy on bone health in adolescents and young adults. It’s crucial to consider all aspects of weight-loss surgeries, including their long-term effects on different aspects of health.
The findings of this study shed light on the need for monitoring and managing bone health post-surgery, especially considering the increase in bone marrow fat and the reduction in bone density and strength observed two years after sleeve gastrectomy. This information can inform healthcare professionals and patients about potential risks and the importance of implementing strategies to support bone health during the weight-loss journey.
For individuals who are still facing challenges with weight loss or considering different weight-loss options, it’s essential to seek comprehensive solutions that address overall health and well-being. If you’re looking for effective strategies and personalized guidance, I recommend exploring the resources available at [https://o-trim.co/nxL3zz]. Our platform offers valuable insights, support, and practical tips to help individuals achieve their weight-loss goals while prioritizing their overall health.
Remember, weight loss is a complex journey, and it’s crucial to approach it holistically, considering various factors such as bone health. By clicking the provided link, you can access further information and resources that may contribute to your weight-loss success and overall well-being. Start your transformation today and prioritize your health every step of the way!
What incompetent parent has 1) allowed their child to become a whale and 2) authorizes optional adolescent surgery? This is child abuse!
Did they really think severely restricting nutrient intake in a growing/developing body would have no negative impacts?
Never have blind faith in a doctor or anything medical related, I learned the hard way.
Its more about making money than it is making you healthy.