COVID-19 infection can cause changes in calcium channels that can affect how the heart beats, it can also trigger inflammation and oxidative stress in the heart.
Potentially life-threatening heart issues can be caused by COVID-19 infections. Scientific studies suggest that people with COVID-19 are 55% more likely to suffer a major adverse cardiovascular event, including heart attack, stroke, and death, than those without COVID-19. They’re also more likely to have other heart issues, like arrhythmias (abnormal heart rhythms) and myocarditis (inflammation of the heart muscle).
Andrew Marks, a cardiologist and biophysics professor at Columbia University, Steven Reiken, a research scientist in Marks’ lab, and colleagues, have studied some of the changes that occur in the heart that could lead to these problems. Reiken will present their work on Monday, February 20 at the 67th Annual Biophysical Society Meeting in San Diego, California.
Molecular Changes in Hearts
In heart tissue from patients who had COVID-19, the team observed increases in oxidative stress (harmful production of unstable molecules) and signals of inflammation, as well as changes in calcium. They also detected adverse changes to a protein called RyR2, which is responsible for regulating the heart’s calcium ion levels. The heart muscle, like all muscle cells, needs calcium ions to contract. The heart’s system for managing calcium ions is essential for the coordinated contractions of the atria and ventricles that pump blood throughout the body. When calcium in the heart becomes dysregulated, it can cause arrhythmias or heart failure.
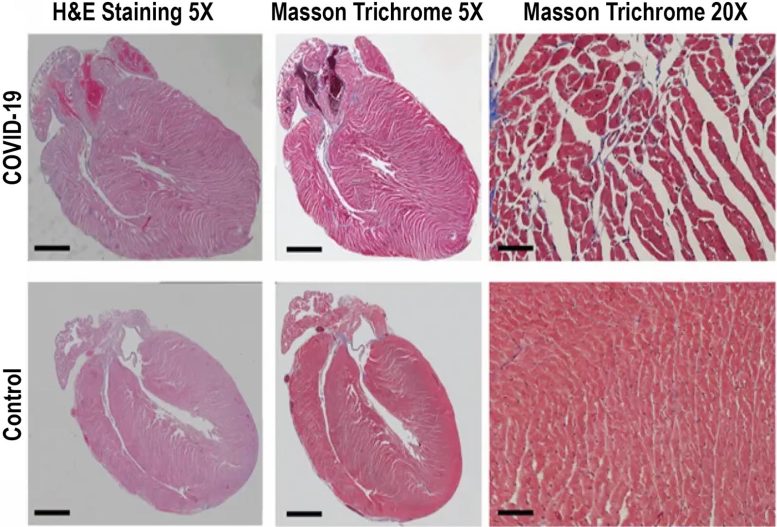
To study changes to the heart further, they used a mouse model infected with COVID-19. They observed changes to the heart tissue including immune cell infiltration, collagen deposition (indicative of injury), death of heart cells, and blood clots. They also measured changes to the heart proteome—the proteins that are expressed by the heart cells—and found patterns consistent with changes observed to human hearts that were infected with COVID-19, as well as markers of cardiomyopathy, which can make it harder for the heart to pump blood to the body and can lead to heart failure.
“The more awareness you build around particular aspects of a disease, the more likely you are to improve the care of patients. And doctors should be aware of heart changes related to COVID-19 infections and should be looking for them,” Marks said.
Ultimately, “we want to really figure out what’s causing the heart disease and how to fix it,” Marks said. Understanding changes at the molecular level may reveal drug targets that could improve cardiac symptoms related to COVID-19 and help healthcare professionals diagnose and treat these issues more effectively. Additionally, understanding the cardiac complications of COVID-19 can also help public health officials make more informed decisions about how to respond to the COVID-19 pandemic, especially in advising those at higher risk for heart problems.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
2 Comments
Oddly, I developed cardiac arrhythmias after the pfizer covid vaccine along with tinnitus, neuropathy and muscle fasciculations. Is anyone looking into this?
No. It’s probably due to climate change.
Search youtube for Dr. John Campbell and one of his COVID-19 videos. He’s had similar problems, and explains in a balanced scientific way.