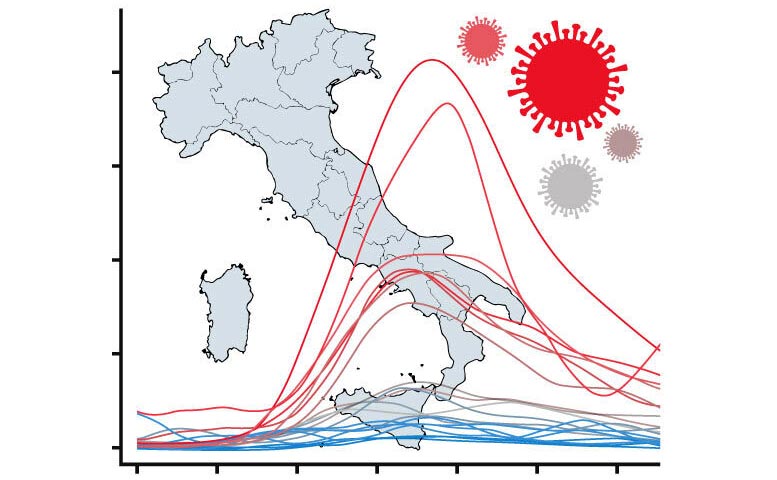
New study uses novel statistics to understand why some regions in Italy were hit harder than others during the first wave of the pandemic.
Staying home and limiting local travel, supporting access to primary care, and limiting contacts in contagion hubs — including hospitals, schools, and workplaces — are strategies that might help reduce COVID-19-related deaths, according to new research. The research team, by statisticians at Penn State, the Sant’Anna School of Advanced Studies in Pisa, Italy, and Université Laval in Quebec, Canada, used novel statistical approaches to compare the first wave of the epidemic across 20 regions in Italy and identify factors that contributed to mortality.
“The first wave of the COVID-19 epidemic took very different paths in different regions, with some areas being hit especially hard while others fared much better,” said Francesca Chiaromonte, leader of the research team, who is a professor of statistics and the holder of the Lloyd and Dorothy Foehr Huck Chair in Statistics for the Life Sciences at Penn State, and the scientific coordinator of the EMbeDS department of excellence at the Sant’Anna School. “We wanted to understand why some regions were hit so much harder than others, so we used both vetted and newly developed techniques in a field of statistics called functional data analysis to compare how the first wave progressed in different regions in Italy.”
Rather than focusing on models for predicting epidemic trajectories, the study used functional data analysis techniques to gather information from the shapes of mortality curves over time, providing a sensitive way to capture associations and patterns from data. The researchers compared mortality curves during the first wave of the epidemic across 20 regions in Italy. After clustering and aligning the curves, to characterize their shapes and account for outbreaks beginning on different dates, the researchers could evaluate factors that might contribute to their differences. Their results appear August 30 in the journal Scientific Reports.
Mobility as a Key Predictor of COVID-19 Deaths
The researchers found that local mobility — how much people moved around their local areas — was strongly associated with COVID mortality. Specifically, they used data from Google’s “grocery and pharmacy” category, which reflects mobility linked to acquiring necessities such as food and medicine. During a national lock-down which started in March 2020, these mobility levels dropped drastically in Italy, roughly by 30% just in the first week of lockdown and then further by as much as 60% during weekdays and almost 100% during weekends in March and April.
“Early on in the epidemic, there were a lot of questions about whether mobility restrictions would really work; our results add to the mounting evidence that they do,” said Chiaromonte. “We see the effect with a lag, but when people reduced their mobility, we saw fewer COVID-related deaths. And we aren’t the only ones to document this, so when we’re told to stay home as a mitigation measure, we should stay home!”
The rates of positive COVID tests and mortality were also associated with each other with a lag, according to the study, reaffirming that positivity is a useful measure to include in disease models.
The research team also investigated several demographic, socio-economic, infrastructural, and environmental factors one at a time to see if they could further explain patterns in mortality. These included factors such as the percent of the population over 65, prevalence of pre-existing conditions such as diabetes and allergies, accessibility of primary care and ICU beds, and factors that might increase contact rates, such as the number of beds in a hospital or nursing home and the number of students per classroom.
“Based on the associations captured by our statistical techniques, what reduces mortality may not be so much having big fancy hospitals with lots of ICU beds, but rather having good access to primary care doctors,” said Chiaromonte. “In fact, having big hospitals may have backfired because they acted as contagion hubs. The places where you have more beds per hospital, more beds per nursing home, more pupils per classroom, and more employees per firm are where epidemics were the strongest.”
Rethinking Contact Points and Health Systems
With additional research to confirm these trends, these results could inform decision making, for example encouraging short- and medium-term investments to boost distributed primary health care and to limit contacts in contagion hubs. Schools and workplaces could encourage pods, where students and employees see only a limited group of individuals, and hospitals could segment sections to reduce contacts.
“Importantly though, even controlling for these factors in our statistical analyses, mobility still remains a very strong lagged predictor of mortality,” said Chiaromonte. “And even accounting for mobility, positivity rates, and the other factors we considered, we still can’t fully explain why the epidemic was so much more intense in Lombardia, a northern industrialized region that includes Milan, compared to the rest of the country. They are still an outlier relative to what our models can explain. Increasing access to accurate, timely and high geographic resolution data might allow us and other researchers to validate results and improve our ability to explain the most extreme trajectories — such as those observed in Lombardia during the first wave of COVID-19.”
Limited data availability and accuracy posed several challenges for this study. For example, official death counts reflected serious underreporting early in the epidemic, so the research team also integrated information on differential mortality—differences in overall deaths in 2020 compared to the average death rate over the previous five years. However, more accurate information on deaths, as well as cases and hospitalizations, at a finer geographic scale, and possibly partitioned by sex, age, pre-existing conditions, and other characteristics would allow the team to improve their models. Additionally, demographic, socio-economic, infrastructural and environmental data are frequently reported at a coarse geographic scale and are often multiple years out of date.
“Some progress has been made since the beginning of the pandemic, but we hope that going forward governmental agencies, statistical offices, and other groups will really prioritize data collection, integration, and availability to qualified researchers,” said Chiaromonte. “All the ambiguity and questions we had early on, and still have in some cases, about where contagions occur, whether the virus is spreading in restaurants or gyms or on public transport, or if certain mitigation measures work—we could answer these questions much more effectively with good data. We are already trying to capitalize on the progress — for instance, Google has made their measures for mobility available at a finer geographic resolution, and we are using them to analyze the second wave of the COVID-19 epidemic in Italy. But we cannot stress enough how important it is to have access to accurate, fine-grained, and current information on the epidemic and on the many variables that may contribute to aggravating or mitigating it.”
Reference: “Functional data analysis characterizes the shapes of the first COVID-19 epidemic wave in Italy” by Tobia Boschi, Jacopo Di Iorio, Lorenzo Testa, Marzia A. Cremona and Francesca Chiaromonte, 30 August 2021, Scientific Reports.
DOI: 10.1038/s41598-021-95866-y
In addition to Chiaromonte, the research team includes Tobia Boschi, a graduate student in statistics at Penn State; Jacopo Di Iorio, who was a postdoc at the Sant’Anna School and will soon become an Eberly Postdoctoral Research Fellow at Penn State; Lorenzo Testa, a graduate student at the Sant’Anna School who is currently a Penn State visiting scholar; and Marzia Cremona, a former Bruce Lindsay Visiting Assistant Professor in the statistics department at Penn State, who is now an assistant professor in Data Science at the Université Laval in Quebec, Canada.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.