As a result of organ transplantation, patients need to take a lifelong regimen of immunosuppressors to fight off graft-versus-host disease (GvHD), which is common and often deadly. Now, researchers have been able to completely replace people’s bone-marrow-derived stem cells with those from unrelated donors without causing GvHD. This means that the recipients could also accept kidneys from the same donors without the need for immunosuppressors.
According to experts, the findings, which were published today in the journal Science Translational Medicine, are extremely important and will undoubtedly change the quality of life of transplant patients.
The latest study builds off research that Tatsuo Kawai, a transplant surgeon at Massachusetts General Hospital in Boston, began with his colleagues almost fourteen years ago. That’s when they launched a clinical trial that attempted to use bone marrow to induce immune tolerance for kidney recipients and avoid lifelong immunosuppressive therapy.
The researchers showed that the majority of people could achieve stable kidney function and successfully wean off their immunosuppressants with few side-effects, but the protocol didn’t work for everybody and the study subjects maintained foreign bone marrow only for a few weeks.
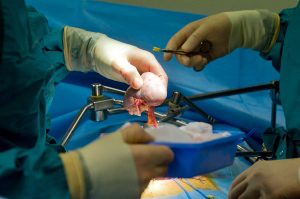 The new findings, by a team led by Suzanne Ilstad, director of the University of Louisville’s Institute for Cellular Therapeutics in Kentucky, make use of a regimen involving chemotherapy, radiation, and blood stem cells manipulated to eliminate those that cause GvHD as well as facilitating cells.
The new findings, by a team led by Suzanne Ilstad, director of the University of Louisville’s Institute for Cellular Therapeutics in Kentucky, make use of a regimen involving chemotherapy, radiation, and blood stem cells manipulated to eliminate those that cause GvHD as well as facilitating cells.
Five of the eight people who underwent the treatment were able to stop taking immunosuppressants within a year after their kidney and stem-cell transplants, four of which came from unrelated donors. Since then, Ilstad has treated seven more patients in this fashion.
This could open the door for any patient with a hematological condition, such as leukemia or sickle-cell anemia, to use bone marrow transplants to get much needed transplants from unmatched donors.
It remains unclear exactly how Ilstad’s recipe succeeds and whether the facilitating cells or the timing of a certain chemotherapy drug, called cyclophosphamide, prevents graft rejection and GvHD. The secrecy is due to the fact that Ilstad is seeking a way to commercialize the approach through a company she founded, Regenerex.
Reference: “Chimerism and Tolerance Without GVHD or Engraftment Syndrome in HLA-Mismatched Combined Kidney and Hematopoietic Stem Cell Transplantation” by Joseph Leventhal, Michael Abecassis, Joshua Miller, Lorenzo Gallon, Kadiyala Ravindra, David J. Tollerud, Bradley King, Mary Jane Elliott, Geoffrey Herzig, Roger Herzig and Suzanne T. Ildstad, 7 March 2012, Science Translational Medicine.
DOI: 10.1126/scitranslmed.3003509
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.