Obesity in young adults appears to trigger early biological changes linked to inflammation, liver stress, and neuronal damage.
Researchers found that low choline levels strongly correlate with these risks, hinting at a nutrient gap affecting long-term brain health.
How Physical Health Shapes Brain Health
Researchers have long recognized that problems affecting the body often influence the brain as well. Conditions such as obesity, high blood pressure, and insulin resistance place heavy demands on the body’s metabolic and vascular systems. Over many years, that constant strain can accelerate cognitive decline and raise the likelihood of developing Alzheimer’s disease.
A new study led by Arizona State University scientists suggests that these brain-related effects may begin far earlier in life than once believed. In young adults with obesity, the research team detected biological indicators of inflammation, liver strain, and early signs of injury to brain cells. Although subtle, these markers resemble patterns typically found in older adults experiencing cognitive impairment.
One unexpected finding stood out. Many of the young adults in the study had unusually low levels of choline in their blood. Choline is an essential nutrient that plays a central role in liver function, inflammation management, and long-term brain health.
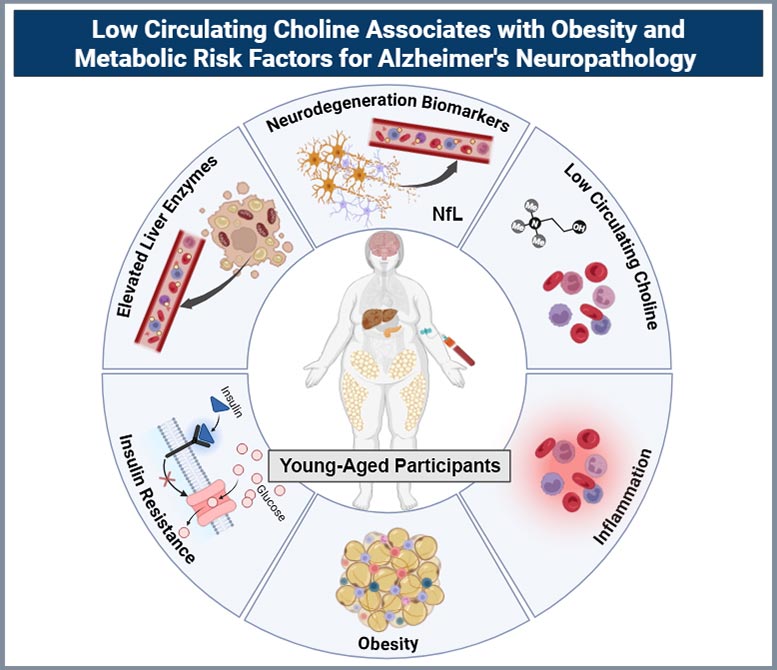
“This research adds to the growing evidence that choline is a valuable marker of metabolic and brain dysfunction—and reinforces the importance of sufficient daily intake, as it is essential for human health,” says Ramon Velazquez. “Several new reports published this month further link reduced blood choline levels to behavioral changes, including anxiety and memory impairment, as well as broader metabolic dysfunction.”
Velazquez, who led the investigation, is part of the ASU-Banner Neurodegenerative Disease Research Center and worked with collaborators from the ASU School of Life Sciences, Banner Sun Health Research Institute and Mayo Clinic, AZ. The work appears in the journal Aging and Disease.

Early Biological Signs That Connect Obesity and Brain Function
Although obesity is widely known to raise the risk of heart disease and type 2 diabetes, the new findings indicate that its effects may extend to the brain earlier than expected. The researchers reported elevated levels of proteins linked to persistent inflammation, along with enzymes signaling liver stress. They also observed increases in neurofilament light chain (NfL), a protein released into the bloodstream when neurons are damaged. Notably, higher NfL levels aligned with lower choline levels, even at ages when behavioral changes would not typically be apparent.
NfL is becoming increasingly recognized as an early indicator of neurodegenerative processes. Individuals with mild cognitive impairment or Alzheimer’s disease often have elevated NfL levels. Detecting similar signals in young adults is noteworthy and suggests that obesity may leave early measurable effects on the brain long before symptoms appear.
These results highlight how metabolic stress, inflammation, and neuronal health may be closely linked, potentially forming a biological pathway that begins much earlier than previously understood.

Choline’s Role in Metabolic and Brain Health
A key takeaway from the study involves the clear relationship between choline status and overall metabolic health. Choline is required for proper liver function, inflammation control, cell-membrane integrity, and the production of acetylcholine, a neurotransmitter important for memory and cognition.
Young adults with obesity showed significantly lower levels of circulating choline. These lower levels closely matched increases in inflammation, insulin resistance, liver-enzyme activity, and NfL.
Although the liver produces a small amount of choline, most of it must come from food. Good dietary sources include eggs, poultry, fish, beans and cruciferous vegetables such as broccoli, cauliflower and brussels sprouts. The study also noted that women had lower choline levels than men, which is particularly striking because women are disproportionately affected by cognitive aging and Alzheimer’s disease.
National nutrition surveys show that many Americans fail to meet the recommended choline intake, especially adolescents and young adults. Because choline supports both liver and brain health, consistently low intake may increase vulnerability to metabolic stress. This could create conditions in which obesity’s impact on the brain becomes even more pronounced.
“Most people don’t realize they aren’t getting enough choline,” said Wendy Winslow, first co-author of the new study. “Adding choline-rich foods to your routine can help reduce inflammation and support both your body and brain as you age.”
Nutrition Challenges Linked to Next-Generation Weight-Loss Drugs
The new wave of weight-loss medications has transformed obesity care due to their strong impact on body weight, metabolic markers, and cardiovascular health. However, GLP-1 drugs significantly reduce calorie intake and alter eating habits.
As a result, people using these medications may unintentionally consume too little choline and other essential nutrients. This raises questions about whether supplementation could help maintain metabolic stability and protect brain health in people taking GLP-1 therapies. Further research will be needed to explore this possibility.

How Researchers Conducted the Study
The study included 30 young adults in their 20s and 30s, divided evenly between those with obesity and those of healthy weight. Each volunteer provided a fasting blood sample so the researchers could measure circulating choline, inflammatory cytokines, insulin, glucose, liver-related enzymes, other metabolic markers and NfL.
Comparisons between the two groups revealed a consistent pattern: lower choline levels, increased inflammation, greater metabolic stress, and early signs of neuronal injury in participants with obesity. To understand how these findings relate to brain aging, the researchers compared the young participants’ choline and NfL profiles with data from older adults who had mild cognitive impairment or Alzheimer’s disease.
They found the same pairing of low choline and elevated NfL in both groups. This suggests that biological processes associated with Alzheimer’s may start many years before symptoms develop, particularly in individuals experiencing obesity or metabolic strain.
Taken together, the results show a strong connection between obesity, inflammation, choline levels, and early neuronal stress. This relationship may help explain why metabolic disorders are associated with a higher risk of cognitive decline later in life.
Although the study does not establish causation, it reveals a cluster of biomarkers that closely resemble those observed in older adults with cognitive impairment. It also aligns with earlier studies in rodents indicating that insufficient dietary choline can contribute to obesity, metabolic dysfunction, and increased Alzheimer’s disease pathogenesis.
“Our results suggest that, in young adults, good metabolic health and adequate choline contribute to neuronal health, laying the groundwork for healthy aging,” says Jessica Judd, co-author of the study.
Ongoing research will explore how early metabolic stress influences long-term neurodegenerative risk and may eventually point to strategies for protecting brain health decades before symptoms appear.
Reference: “Reduced Circulating Choline in Young Adults with Obesity Is Associated with Metabolic Dysfunction, Inflammation, and Elevated Neurofilament Light Chain—Factors Linked to Mild Cognitive Impairment and Alzheimer’s Disease” by Wendy Winslow, Jessica M. Judd, Savannah Tallino, Geidy E. Serrano, Thomas G. Beach, Lori R. Roust, Eleanna De Filippis, Brooke Brown, Christos Katsanos and Ramon Velazquez, 25 November 2025, Aging and Disease.
DOI: 10.14336/AD.2025.1207
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
What are nutrient supplements that may prevent Alzheimer’s an disease?