A simple positioning mistake during a blood pressure check could quietly alter the results.
That quick blood pressure check at the doctor’s office may not be as accurate as you think. According to research from Johns Hopkins Medicine, something as simple as where you rest your arm during the test can significantly raise the reading and potentially lead to a hypertension diagnosis that is not actually correct.
The study found that two common arm positions frequently used in clinics can artificially increase blood pressure measurements by enough to shift some patients into a higher risk category. Researchers say the findings are especially important because high blood pressure is one of the leading causes of heart disease, stroke, kidney failure, and preventable death worldwide.
Published in JAMA Internal Medicine, the study examined how different arm positions affect blood pressure readings in adults between 18 and 80 years old. Researchers compared the guideline-recommended position, with the arm supported on a desk at heart level, against two alternatives often seen in real-world settings: resting the arm in the lap and letting the arm hang unsupported at the side.
The differences were striking.
Small Changes, Significant Effects
When participants rested their arm on their lap, systolic blood pressure readings rose by an average of 3.9 mmHg, while diastolic pressure increased by 4.0 mmHg. When the arm hung unsupported at the side, systolic pressure climbed by 6.5 mmHg and diastolic pressure by 4.4 mmHg.
That may sound minor, but even small changes in blood pressure readings can have major consequences. A difference of just a few points can determine whether someone is considered healthy, at risk, or in need of medication.
“If you are consistently measuring blood pressure with an unsupported arm, and that gives you an overestimated BP of 6.5 mmHg, that’s a potential difference between a systolic BP of 123 and 130, or 133 and 140, which is considered stage 2 hypertension,” said Sherry Liu, M.H.S., a study author and epidemiology research coordinator at the Johns Hopkins Bloomberg School of Public Health.

Hypertension affects nearly half of U.S. adults, according to the American Heart Association. Yet many people do not realize they have it because symptoms are often absent until serious damage has already occurred. That makes accurate screening especially important.
Why Proper Positioning Matters
Doctors have long known that talking during a reading, crossing your legs, using the wrong cuff size, or drinking caffeine beforehand can distort results. This study adds more evidence that arm position is another overlooked factor that can quietly skew measurements.
The researchers designed the trial to closely mirror a typical doctor’s appointment. Participants first emptied their bladders, walked for two minutes, and then sat quietly with their backs supported and feet flat on the floor. Each person underwent repeated blood pressure measurements using all three arm positions. To reduce the impact of natural fluctuations in blood pressure, researchers also repeated the standard desk-supported measurement at the end of the session.
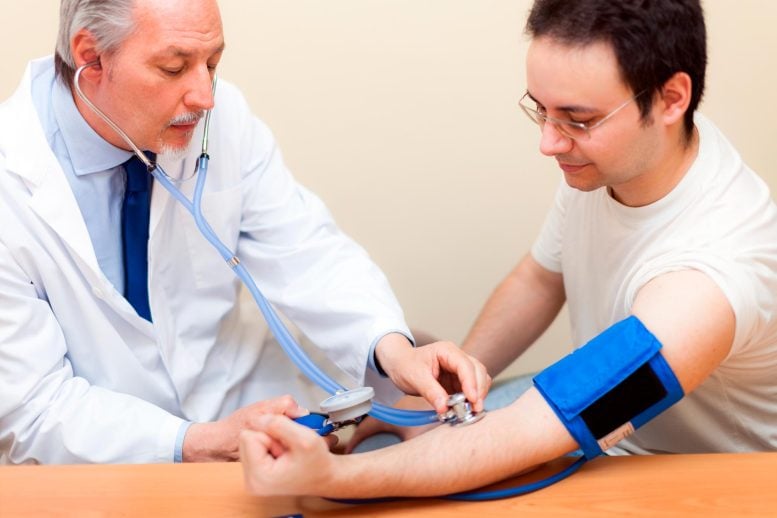
The study included 133 adults in Baltimore, Maryland, with a broad mix of ages and health backgrounds. About 36% had systolic blood pressure readings of 130 mmHg or higher, and 41% had obesity. The pattern of inflated readings remained consistent across groups, including older adults and people with obesity.
A Widespread Issue in Clinics and Homes
Researchers say the problem is widespread because many clinics do not strictly follow measurement guidelines. Patients are often seated on exam tables without proper arm support, or they may rest their own arm in their lap while a reading is taken. In some cases, a health care worker holds the patient’s arm during the test, which can also affect positioning.
The standard recommendation is simple: sit upright in a chair with feet flat on the floor, legs uncrossed, and the arm resting on a desk or table so the blood pressure cuff sits at heart level.
Tammy Brady, M.D., Ph.D., senior author of the study and a hypertension specialist at Johns Hopkins Medicine, said the findings reinforce the need for both clinicians and patients to pay closer attention during screenings.
The issue extends beyond doctor’s offices. Millions of people now use home blood pressure monitors, but many may unknowingly take readings while sitting on a couch, reclining, or holding their arm incorrectly. Experts say inaccurate home measurements can create unnecessary anxiety or lead people to believe their treatment is not working.
The researchers caution that the study focused on automated blood pressure devices, so the findings may not apply to every type of monitor. Still, they say the message is clear: proper positioning matters far more than many people realize.
Follow-up Research
The authors later followed up the work with a broader review exploring how blood pressure checks could be streamlined in busy clinics without sacrificing accuracy. The follow-up analysis found that some guideline steps, including long rest periods before measurements, may be shortened or simplified. However, the researchers stressed that proper cuff sizing, correct patient posture, and keeping the arm supported at heart level remain essential because mistakes in those areas can significantly distort readings.
They concluded that a faster, evidence-based approach to blood pressure screening could allow clinics to evaluate far more patients each day while still avoiding the kinds of measurement errors uncovered in the original arm-position study.
References:
“Evidence-Based, Streamlined Approach to Measure Blood Pressure in Primary Care Settings” by Kathryn Foti, Andrew E. Moran, Kunihiro Matsushita, Lawrence J. Appel, Stephen P. Juraschek, Anupam Khungar Pathni, Bolanle F. Banigbe, Girma A. Dessie, Bishal Belbase, Mahfuzur Rahman Bhuiyan, Shamim Jubayer, Sohel Reza Choudhury and Tammy M. Brady, 26 November 2025, Hypertension.
DOI: 10.1161/HYPERTENSIONAHA.125.24527
“Arm Position and Blood Pressure Readings: The ARMS Crossover Randomized Clinical Trial” by Hairong Liu, Di Zhao, Ahmed Sabit, Chathurangi H. Pathiravasan, Junichi Ishigami, Jeanne Charleston, Edgar R. Miller, Kunihiro Matsushita, Lawrence J. Appel and Tammy M. Brady, 7 October 2024, JAMA Internal Medicine.
DOI: 10.1001/jamainternmed.2024.5213
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
23 Comments
If I am taking a blood pressure measurement during a hot flush the blood pressure is significantly higher. If the measurement is taken just before a hot flush it can be lower. Coffey increases the blood pressure for a significant time.
I agree with the level of arm support for Blood pressure accuracy.
Relaxing before the measurements is helpful.
I find my pressure is higher when I’m anxious.
Very interesting article.
Worth sharing.
Thank you.
It’s wrong readings can misslead
Just on Tuesday this week I wondered how my BP is high 132/87. This could be because of wrong positioning of the arm
Totally agree with placing the arm resting on a table at heart level. My experience in different doctor visits is how you are hurried through triage. They rush you in, take your blood pressure, pulse, and temperature while asking questions like “What is the reason for your visit?” This is so medically wrong. Half the time, the equipment is in need of repair or replaced. Then you have a doctor ready to put you on blood pressure medicine. It just drives me nuts!!
Just anecdotal, it seems to me that if I take a number of deep breaths before the BP measurement it lowers the measurement.
Same experience with me. About 30 seconds of deep breathing prior to measuring my BP will lower the reading quite noticeably. Unfortunately, I find the effect to be only temporary.
I took BP with home machine,was 117 etc, when hrs later with stressful dr & wait in office was 140/ so readings can definitely NOT be accurate,I’m not overweight & have great #’s on blood panel work!!!
My BP is always higher when the nurse takes it. After I’ve been in the room a few minutes, my doc takes it and it’s much lower. I always recommend taking more than one reading.
Take your device with you to the doctors office and take your BP while you’re waiting. That way you’ll know if its your device or just stress.
Take 5 readings with your machine and see the 5 widely different numbers it returns. They are very much unreliable, especially wrist cuff ones.
people getting a different blood pressure reading at home than at the doctors office is a well known phenomenon. some people have a higher reading always at the doctors office. some will have a lower reading always. its a known psychological effect.
Scare tactics, can’t leave well enough alone,let’s feed the fear and keep em coming back. I’m done with the sell outs ,Dr have lost credibility.you fafo’d we’re done.
All the pictures in an article about how to use a blood pressure cuff correctly show the tube at the back of the arm.
You morons cant be helped.
Apart from everything else, I am surprised by the need for this study. As a medical student, one is always reminded that two positions could influence one’s blood pressure. If the arm is dropped by your side, the BP will be higher, and if the arm is raised above your head, the BP will be lower. The best is when the arm is at the level of the heart. However, at least in the UK, GPs are told to spend only 0 minutes with each patient, and this could influence the time for taking the BP. The best is self-BP measurement at home.
Right, but was what you were told in med school based on actual studies? Or suppositions? We still know very little about the human body, studies like this add to the knowledge so that we arrive at facts backed up by objective testing, not guesses and assumptions.
For me the question is “who polices the police”. How do they know the blood pressure they’re comparing the tests to is accurate and factual.
My cardiologist who retired last year, would always tuck my arm under his to keep it at heart level. None of nurses did so. Not surprisingly, my BP was always better when he took it.
Try taking a blood pressure from someone who has Alzheimer’s and can’t follow directions to sit still and proper alignment of body position. Or a little kid who can’t sit still. You have to have a lot of patience. Lol
Try taking a blood pressure from someone who has problems and can’t follow directions to sit still
How were arms positioned when b.p. standards were established?
It’s even worse if you’re short and they’re always in too much of a rush to lower the table for you, so they grab your arm and twist it. Or have you supported by a thin chair arm bar with most of your arm cantilevered.
I’ve also noticed a huge difference in my BP when the last patient had a very high level so the cuff squeezes me too hard because they’re programmed to not reset.
The American Heart Association said this over a decade ago. I implemented it back then but apparently no doctor’s offices have.
Best reading is the “zero level posture” (and should be the standard) is for the patient to lay down, arm extended at lying level and the reading taken!