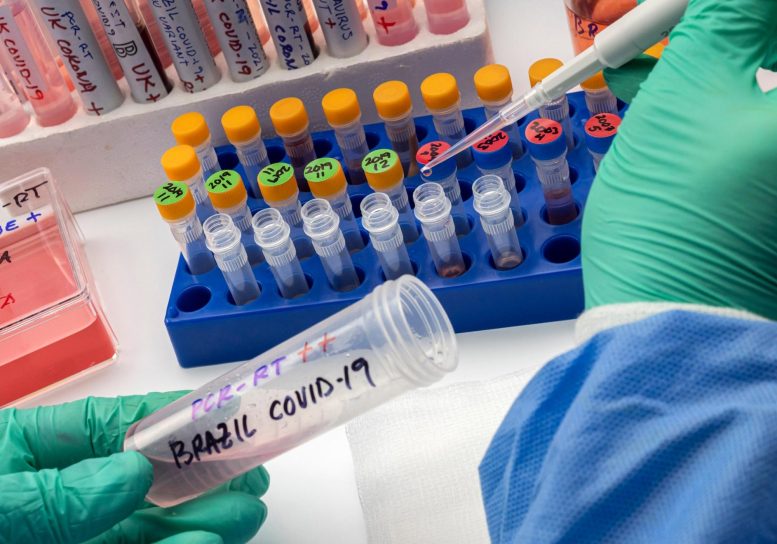
A new study presented at this year’s European Congress of Clinical Microbiology & Infectious Diseases (ECCMID) and published in The Lancet Microbe, shows that antibodies generated by CoronaVac, an inactivated COVID-19 vaccine, work less well against the P.1 Brazil (Gamma) variant.
It also suggests that the P.1 variant may be able to reinfect individuals who previously had COVID-19.
The SARS-CoV-2 virus spike protein is the primary target of neutralizing antibodies — antibodies that block the entry of the virus into cells — including those induced by vaccines. The emergence of variants with multiple mutations in this protein has raised concerns that neutralizing antibody responses, and so the effectiveness of vaccination programs, could be compromised.
The P.1 variant was discovered in Manaus, Brazil, in early January 2021 and has 15 unique mutations. Previous studies have found evidence that it can escape neutralization by antibodies. However, most of these studies used modified viruses and there is little information on the ability of the wild-type P.1 variant, with a complete set of mutations, to evade neutralizing antibodies in individuals previously infected with COVID-19 or vaccinated with an inactivated vaccine.
Dr. Jose Luiz Proença-Módena, Laboratory of Emerging Viruses, University of Campinas, Brazil, and colleagues, studied the sensitivity of the P.1 variant to neutralizing antibodies present in the serum of 53 individuals who had been vaccinated and 21 who had been previously infected with SARS-CoV-2.
The results were compared with those for a B lineage virus, one of the dominant strains in Brazil before the emergence of the P.1 variant.
The vaccinated group was made up of 18 individuals who had received a single dose and 20 who had received two doses of the CoronaVac inactivated vaccine during the Brazilian vaccination program, plus 15 participants who had received two doses during a trial.
CoronaVac is one of the main vaccines in Brazil’s national immunization program and has been approved for emergency use in Brazil, China, Columbia, Indonesia, Mexico, and Turkey. Previous research from Brazil has shown it to be 50.7% effective at preventing symptomatic infections.
All the blood samples from individuals with past infections had high concentrations of SARS-CoV-2-specific antibodies. Tests showed the P.1 variant to be less sensitive to these antibodies than the B lineage virus. Antibody concentrations needed to be around nine times higher to neutralize the P.1 variant than the B lineage virus.
Antibodies from vaccinated individuals were also less efficient at neutralizing the P.1 variant than the B lineage virus. The antibodies from almost all of the people who had one dose of the vaccine (20-23 days earlier) as part of the immunization program and all of those who had two doses in the trial (134-260 days earlier) had no detectable effect on the P.1 variant.
In contrast, the P.1 variant was still sensitive to the antibodies in the plasma of those who had two doses in the immunization program (second dose 17-38 days earlier) but to a lesser extent than the B lineage virus.
The authors say: “This study shows that antibodies present in the plasma of people with a history of COVID-19 or individuals vaccinated with CoronaVac were less efficient at neutralizing P.1 variant isolates than a B lineage isolate.
“Neutralising antibodies are an important component of the immune response against SARS-CoV-2. Therefore, the capacity of the P.1 variant to evade antibodies present in the plasma of CoronaVac-immunised individuals suggests that the virus can potentially circulate in vaccinated individuals — even in areas with high vaccination rates.”
They add: “Our results also suggest that the P.1 variant can escape from neutralizing antibody responses generated by previous SARS-CoV-2 infection and thus reinfection might be possible.
“Consequently, continued and enhanced genetic surveillance of SARS-CoV-2 variants worldwide, paired with plasma neutralizing antibody assays is required to guide updates of immunization programs.
“However, a phase 3 clinical trial showed that CoronaVac can protect against severe COVID-19 and death. Therefore, neutralizing antibodies might not be the only contributing factor — the T-cell response may also play an important role in reducing disease severity.”
Reference: “Neutralisation of SARS-CoV-2 lineage P.1 by antibodies elicited through natural SARS-CoV-2 infection or vaccination with an inactivated SARS-CoV-2 vaccine: an immunological study” by William M Souza, PhD; Mariene R Amorim, MSc; Renata Sesti-Costa, PhD; Lais D Coimbra, MSc; Natalia S Brunetti, BSc; Daniel A Toledo-Teixeira, MSc; Gabriela F de Souza, MSc; Stefanie P Muraro, MSc; Pierina L Parise, BSc; Priscilla P Barbosa, MSc; Karina Bispo-dos-Santos, BSc; Luciana S Mofatto, PhD; Camila L Simeoni, BSc; Ingra M Claro, BSc; Adriana S S Duarte, PhD; Thais M Coletti, BSc; Audrey B Zangirolami, MSc; Carolina Costa-Lima, MSc; Arilson B S P Gomes, BSc; Lucas I Buscaratti, BSc; Flavia C Sales, BSc; Vitor A Costa, BSc; Lucas A M Franco, PhD; Darlan S Candido, MSc; Oliver G Pybus, DPhil; Jaqueline G de Jesus, PhD; Camila A M Silva, BSc; Mariana S Ramundo, PhD; Giulia M Ferreira, BSc; Mariana C Pinho, BSc; Leandro M Souza, BSc; Esmenia C Rocha, BSc; Pamela S Andrade, BSc; Myuki A E Crispim, PhD; Grazielle C Maktura, PhD; Erika R Manuli, BSc; Magnun N N Santos, PhD; Cecilia C Camilo, BSc; Rodrigo N Angerami, PhD; Prof Maria L Moretti, PhD; Fernando R Spilki, PhD; Prof Clarice W Arns, PhD; Marcelo Addas-Carvalho, PhD; Bruno D Benites, PhD; Marco A R Vinolo, PhD; Marcelo A S Mori, PhD; Nelson Gaburo, PhD; Christopher Dye, DPhil; Henrique Marques-Souza, PhD; Rafael E Marques, PhD; Alessandro S Farias, PhD; Prof Michael S Diamond, PhD; Nuno R Faria, DPhil; Prof Ester C Sabino, PhD; Fabiana Granja, PhD and Jose Luiz Proença-Módena, PhD, 8 July 2021, Lancet Microbe.
DOI: 10.1016/S2666-5247(21)00129-4
Meeting: European Congress of Clinical Microbiology & Infectious Diseases (ECCMID)
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.