The COVID-19 pandemic has revealed critical knowledge gaps and assumptions concerning how respiratory viruses spread between hosts.
Traditionally thought to be spread mainly through large respiratory droplets produced by the coughs and sneezes of sick individuals, a growing body of evidence indicates that many respiratory pathogens – including SARS-CoV-2– spread through virus-laden microscopic respiratory aerosols. In this Review, Chia Wang and colleagues discuss the recent research regarding airborne transmission of respiratory viruses and how an improved understanding of aerosol transmission will allow for better-informed controls to reduce and mitigate airborne transmission.
Until recently, most respiratory pathogens were assumed to spread through large droplets expirated from an infectious person or transferred from contaminated surfaces. This understanding has largely guided public health recommendations in mitigating viral spread. However, several respiratory pathogens, including influenza and the common cold, are also known to spread through infectious respiratory aerosols, which can float and travel in air flows at far greater distances and for much longer, infecting those who inhale them.
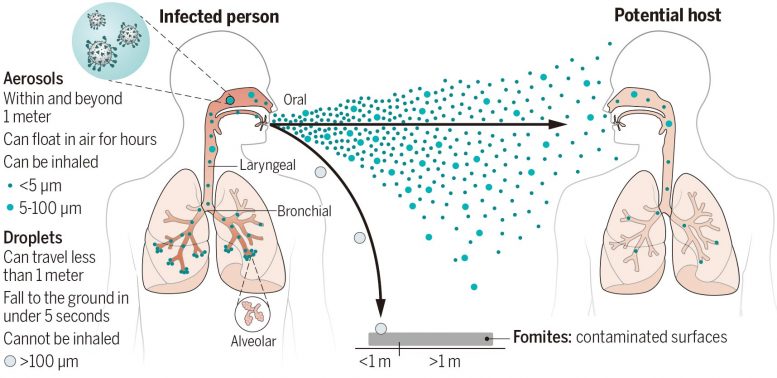
According to a growing body of evidence, much of which was gained from studying the spread of COVID-19, airborne transmission may be a more dominant mode of respiratory virus transmission than previously thought.
Here, Wang et al. highlight how infectious aerosols are generated, travel throughout an environment and deliver their viral payloads to hosts. The authors also outline ways to mitigate aerosol transmission at long and short ranges, including improvements to ventilation and airflows, air filtration, UV disinfection and personal face mask fit and design.
For more on this research, see It’s Not Just COVID-19: Most Respiratory Viruses Actually Spread by Aerosols.
Reference: “Airborne transmission of respiratory viruses” by Kimberly A. Prather, Josué Sznitman, Jose L. Jimenez, Seema S. Lakdawala, Zeynep Tufekci and Linsey C. Marr, 27 August 2021, Science.
DOI: 10.1126/science.abd9149
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
Whether spread by droplets or airborne, the vaccines we have are only handling half the problem. Some of the virus will evade them and enter cells, and we need to understand what happens then.
All the coronaviruses and all their variants have different protein spikes, with Delta having one that’s more efficient at getting around the vaccines. But the real problem is in the virus itself, not its protein shell, and why the most dangerous (MERS, SARS, and Covid-19) are so infectious. My independent research has found multiple one-in-a-million nucleotide sequence matches between all the coronaviruses and the human genome. Those sequences are the same as some of the loops of human tRNA. Using those loops and their amino acid code matches, viruses may be able to fool the nucleus membrane in cells to allow the virus to enter and associate with the human DNA, creating more opportunities for further infection. Our immune system may be compromised and may no longer be able to stop the virus and other diseases from attacking organs throughout the body. Vaccines that attack the virus protein shells while ignoring their contents are doomed to failure from the Darwin effect, but recognizing these loops suggests a possible approach to successful coronavirus vaccines. Only the infection process is considered in my work, not the innate virulence of the virus. For more info, check out this YouTube, Coronavirus – Using Your DNA Against You. https://www.youtube.com/watch?v=8dOIzD6ch8s