Abnormal blood-oxygen levels and breathing rates are strong predictors of poor patient outcomes in-hospital, study shows.
A study of 1,095 patients hospitalized with COVID-19 discovered that two easily measurable signs of health — respiration rate and blood-oxygen saturation — are distinctly predictive of higher mortality. Notably, the authors said, anyone who receives a positive COVID-19 screening test can easily monitor for these two signs at home.
This context is lacking in current guidance from the Centers for Disease Control and Prevention, which tells people with COVID-19 to seek medical attention when they experience overt symptoms such as “trouble breathing” and “persistent pain or pressure in the chest” — indications that may be absent even when respiration and blood oxygen have reached dangerous levels, the authors say.
“These findings apply to the lived experience of the majority of patients with COVID-19: being at home, feeling anxious, wondering how to know whether their illness will progress, and wondering when it makes sense to go to the hospital,” said Dr. Neal Chatterjee of the University of Washington School of Medicine.
Chatterjee and fellow cardiologist Dr. Nona Sotoodehnia were co-lead authors of the paper, which is to be published today (May 24, 2021) in the journal Influenza and Other Respiratory Viruses.
They said the findings suggest that, for some people with COVID-19, by the time they feel bad enough to come to the hospital, a window for early medical intervention might have passed.
Dangerous Symptoms May Be Asymptomatic
“Initially, most patients with COVID don’t have difficulty breathing. They can have quite low oxygen saturation and still be asymptomatic,” said Sotoodehnia. “If patients follow the current guidance, because they may not get short of breath until their blood oxygen is quite low, then we are missing a chance to intervene early with life-saving treatment.”
The researchers examined the cases of 1,095 patients age 18 and older who were admitted with COVID-19 to UW Medicine hospitals in Seattle or to Rush University Medical Center in Chicago. The study span was from March 1 to June 8, 2020. The lone exclusions were people who chose “comfort measures only” at the time of their admission.
While patients frequently had hypoxemia (low blood-oxygen saturation; 91% or below for this study) or tachypnea (fast, shallow breathing; 23 breaths per minute for this study), few reported feeling short of breath or coughing regardless of blood oxygen.
The study’s primary measure was all-cause in-hospital mortality. Overall, 197 patients died in the hospital. Compared to those admitted with normal blood oxygen, hypoxemic patients had a mortality risk 1.8 to 4.0 times greater, depending on the patient’s blood oxygen levels. Similarly, compared to patients admitted with normal respiratory rates, those with tachypnea had a mortality risk 1.9 to 3.2 times greater. By contrast, other clinical signs at admission, including temperature, heart rate, and blood pressure, were not associated with mortality.
Nearly all patients with hypoxemia and tachypnea required supplemental oxygen, which, when paired with inflammation-reducing glucocorticoids, can effectively treat acute cases of COVID-19.
“We give supplemental oxygen to patients to maintain blood oxygen saturation of 92% to 96%. It’s important to note that only patients on supplemental oxygen benefit from the life-saving effects of glucocorticoids,” Sotoodehnia said. “On average our hypoxemic patients had an oxygen saturation of 91% when they came into the hospital, so a huge number of them were already well below where we would’ve administered life-saving measures. For them, that care was delayed.”
Guidance for Physicians and Telehealth
The findings have relevance for family-medicine practitioners and virtual-care providers, who typically are first-line clinical contacts for people who have received a positive COVID-19 test result and want to monitor meaningful symptoms.
“We recommend that the CDC and [World Health Organization] consider recasting their guidelines to account for this population of asymptomatic people who actually merit hospital admission and care,” Chatterjee said. “But people don’t walk around knowing WHO and CDC guidelines; we get this guidance from our physicians and news stories.”
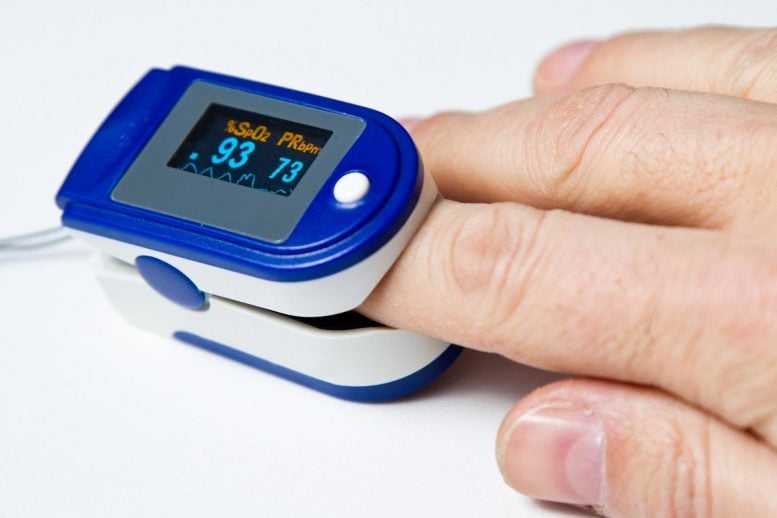
Sotoodehnia recommended that people with positive COVID-19 test results, particularly those at higher risk of adverse outcomes due to advanced age or obesity, buy or borrow a pulse oximeter and monitor for blood oxygen below 92%. The clip-like devices fit over a fingertip and can be purchased for under $20.
“An even simpler measure is respiratory rate — how many breaths you take in a minute. Ask a friend or family member to monitor you for a minute while you’re not paying attention to your breathing, and if you hit 23 breaths per minute, you should contact your physician,” she said.
Reference: “Admission respiratory status predicts mortality in COVID-19” by Neal A. Chatterjee, Paul N. Jensen, Andrew W. Harris, Daniel D. Nguyen, Henry D. Huang, Richard K. Cheng, Jainy J. Savla, Timothy R. Larsen, Joanne Michelle D. Gomez, Jeanne M. Du-Fay-de-Lavallaz, Rozenn N. Lemaitre, Barbara McKnight, Sina A. Gharib and Nona Sotoodehnia, 24 May 2021, Influenza and Other Respiratory Viruses.
DOI: 10.1111/irv.12869
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
When I got Covid, I first tested negative, but it wasn’t until I began gulping for air, became giddy from lack of oxygen, and strangely, lost all muscle control of my core muscles, where I couldn’t sit upright, and when I tried, I would just flop over from one side to the other, my husband said, “Enough! This is NOT RIGHT!” and called 911. I remember not even feeling concerned, and when the Paramedics arrived and came into our bedroom, where I was laying across our bed, I just looked at them and said, “Hey guys, did you come to get me?” Before the ambulance traveled half a block, I was was completely unconscious.
When I finally awoke, two days laterI was in the ICU, and was in and out of consciousness for I cannot even remember for how long. Eventually I did start feeling better enough to ask the physician what I had, and he told me I had Covid, Covid Pneumonia, AND Bacterial Pneumonia, ALL at the same time. They told me I had quite a bit of fluid in my lungs, and wanted to drain off as much as they could, both to help me breathe easier, and also so they could test the composition of the ugliest colored pus I have ever seen in my life, and to also help me breathe easier, so they had to prop me up, lean me forward, and stuck one of the longest needles I had ever seen and using ultrasound guidance to extract as much as of the pus they possibly could! 1000mil out of one lung, and 750mil out of the other.
All of the Doctor’s and Nurse’s there were some of the kindest, considerate, wonderful, people on this Earth, and I could not thank them enough, for literally saving my life!