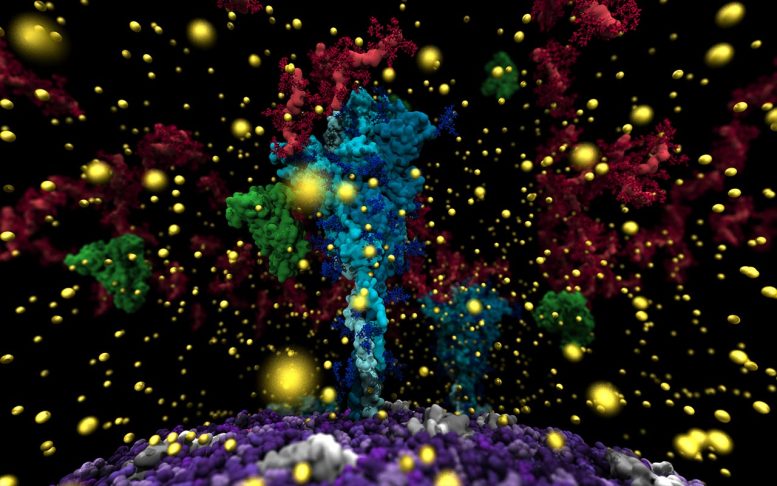
UC San Diego develops computer model to aid understanding of how viruses travel through the air.
Research using high-performance computing has modeled COVID-19’s delta variant in aerosols, enhancing understanding of its airborne transmission.
In May 2021, the Centers for Disease Control (CDC) officially recognized that SARS-CoV-2—the virus that causes COVID-19—is airborne, meaning it is highly transmissible through the air.
Now University of California San Diego Professor and Endowed Chair of Chemistry and Biochemistry Rommie Amaro, along with partners across the U.S. and around the world, has modeled the delta virus inside an aerosol for the first time.
This work was a finalist for the Gordon Bell Prize, given by the Association for Computing Machinery each year to recognize outstanding achievement in high-performance computing. Amaro led the team that won the prize last year for its work on modeling an all-atom SARS-CoV-2 virus and the virus’s spike protein to understand how it behaves and gains access to human cells.
“It’s wonderful to be a finalist for the Gordon Bell Prize a second year in a row,” stated Amaro. “But more than that, we’re really excited about the potential this work has to deepen our understanding of how viruses are transmitted through aerosols. The impacts could change the way we view airborne diseases.”
The Role of Aerosols in Virus Transmission
Aerosols are tiny. A human hair is approximately 100 microns in diameter. Droplets—think of the spray that comes out of your mouth and nose when you sneeze—are larger than 100 microns and fall to the ground in seconds. In contrast, aerosols—produced simply by breathing and speaking-are everything smaller than 100 microns and can float in the air for hours and travel long distances.
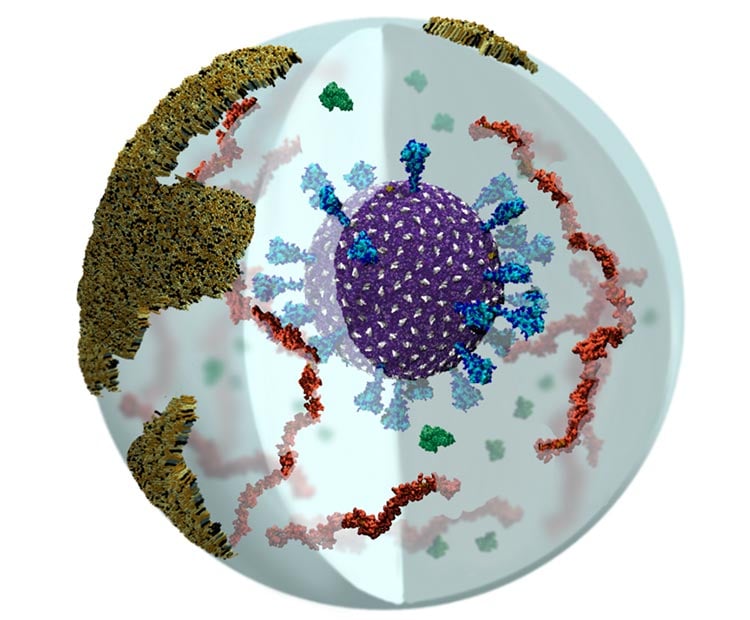
Advancements in Aerosol Research
Kim Prather, Distinguished Chair in atmospheric chemistry and director of the Center for Aerosol Impacts on Chemistry of the Environment (CAICE), has studied sea spray and ocean aerosols extensively. She contacted Amaro several years ago noting that these aerosols had much more than seawater in them.
“The common thinking used to be that ocean aerosols only contained salt water,” Prather stated. “But we discovered there was a ton of ocean-biology inside—living organisms including proteins and viruses. I not only thought Rommie would be interested in studying this, but also thought her work could be really beneficial in helping us gain a better understanding of aerosol composition and movement and airborne survival.”
Amaro’s lab began to develop computer models of what aerosols looked like using Prather’s work in sea spray. These simulations paved the way for Amaro and her group to understand the experimental methods and tools used to study aerosols, generally, as well as develop a useful framework to build, simulate and analyze complex aerosol models.
Innovations in Viral Aerosol Modeling
When SARS-CoV-2 came on the scene in early 2020, she began modeling the virus and was able to show how it infects host cells through a sugary coating called a glycan that covers the spike proteins.
Aerosol scientists always suspected SARS-CoV-2 was airborne, so studying the virus inside an aerosol provided an opportunity to back those suspicions with evidence. Taking the work her lab was already doing with aerosols and the work her lab was also doing with the virus, Amaro put two and two together.
“It’s these fine aerosols that can travel the farthest and move into the deep lung, which can be devasting,” Amaro stated. “There is no experimental tool, no microscope that allows people to see the particles in this much detail, but this new computational microscope allows us to see what happens to the virus—how it moves, how it stays infectious during flight. There is something very powerful about being able to see what something looks like, seeing how components come together—it fundamentally changes the kinds of questions people even think to ask.”
Future Directions and Implications
To better understand how the virus moves and lives inside aerosols, Amaro worked with a team of 52 from around the globe, including Oak Ridge National Laboratory, using their Summit supercomputer to simulate the models. Summit is one of the few supercomputers in the world capable of performing these large-scale simulations, which allowed researchers to see aerosols at an unprecedented one billion atoms.
These simulations included more intricate details of the virus’s membranes, as well as visualizations of aerosols. In addition to the SARS-CoV-2 virus, these sub-micron respiratory aerosols also contained mucins, lung surfactant, water, and ions.
Mucins are polymers that line most of the surfaces of the body that are wet, including the respiratory tract and they may work to protect the virus from harsh external elements like sunlight. One of the hypotheses that Amaro’s team is exploring is whether the delta variant of SARS-CoV-2 is more transmissible in part because it seems to interact so well with mucins.
Now that the models have been built, Amaro hopes to formally create an experiment that will test the predictions of aerosolized virus movements. She is also developing tools that will investigate how humidity, wind, and other external conditions affect the transmission and life of the virus in aerosols.
Beyond the immediate needs of learning as much as possible about how SARS-CoV-2 operates, computer models of aerosols can have wide-ranging impacts, including climate science and human health.
“What we learned during the pandemic is that aerosols were one of the main drivers in spreading the virus and that their importance in the transmission of many other respiratory pathogens has been systematically underappreciated,” said Dr. Robert “Chip” Schooley, a professor in the Department of Medicine at UC San Diego School of Medicine. “The more we learn about aerosols and how they host viruses and pollutants, such as soot, that have adverse health impacts, the better positioned we are to create effective treatment and mitigation measures. This benefits the public health and well-being of people around the world.”
This work was supported by the NSF Center for Aerosol Impacts on Chemistry of the Environment (CAICE), National Science Foundation Center for Chemical Innovation (NSF CHE-1801971), NIH GM132826, NSF RAPID MCB-2032054, Oak Ridge Computing Facility at Oak Ridge National Laboratory (DOE DE-AC05-00OR22725), Texas Advanced Computing Center Frontera (NSF OAC-1818253), Argonne Computing Facility (DOE DE-AC02-06CH11357), and Pittsburgh Supercomputer Center ( NSF TG-CHE060063). Additional funding provided by RCSA Research Corp. and a UC San Diego Moore’s Cancer Center 2020 SARS-CoV-2 seed grant. This work appears in The Proceedings of SC21, Virtual Event, November 14-19, 2021.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
3 Comments
I worked in a hospital. No mask if patient didn’t have cough. I tested positive for COVID and intubated on April 7, 2020. I would spend next 98 days in hospital or rehab AND Intubated again. I would have a radial artery repair. I have Long COVID. I have Neuro issues like brain fog (wrong words, wrong order, stopping in middle of sentence,forgetting names of family, friends). I have balance issues, left sided weakness, and nausea episodes every day. I have no memory of most of my journey. I went to my 1st Dr appointment to follow up. I was using a walker. He told me they didn’t expect me to make it. I am alive.
Amazing technology and presentation. I’m left with continued doubts I have about masking. I don’t see how a cloth mask can possibly prevent this type of transmission. Do you have a view on masking whether it be cloth, N95, K95, etc.? I’ve made up my own mind that cloth masks are useless but what does the science reveal? Thanks and really appreciate this information.
Any thing that reduces the number or size of (harmful) particulates that enter the respiratory systems is beneficial. This is not the same as saying it is a flawless filter.