J. Matthews/Panos
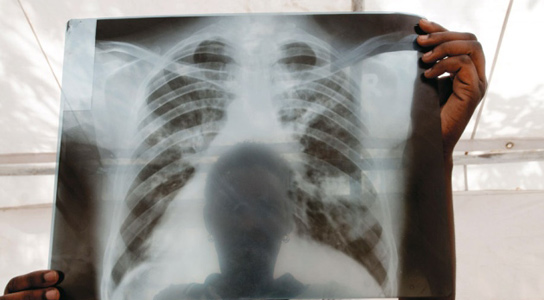
Back in 2005, doctors at a remote hospital in the village of Tugela Ferry, South Africa, were puzzled when patients with HIV, who were initially responding well to antiretroviral drugs, began rapidly dying from tuberculosis.
When patients contract ordinary TB, they start to feel better after a few weeks or months on a selection of four antibiotics. Of the 542 people with TB at the hospital in 2005 and early 2006, 221 (41%) had multi-drug-resistant (MDR) TB, against which these therapies are useless. 53 of them didn’t even respond to the few antibiotics that form a second line of defense. Eventually, all but one of the 53 died, half of them within 16 days of the diagnosis. This was the first major outbreak of extensively drug-resistant (XDR) TB.
The latest report on TB from the WHO, published last October, revealed that new infections of ordinary TB had dropped by 41% since 1990. Some 3.7% of new cases and 20% of previously treated cases were MDR-TB. In 2000, the highest incidence of MDR-TB was in Estonia at 14%. In 2010, it jumped to 35% in Russia’s Arkhangelsk province. An estimated 9% of MDR-TB cases are XDR-TB.
In some countries, particularly in Europe, Asia, and Africa, the weakening or collapse of healthcare systems over the past 20 years has meant that patients combating ordinary TB don’t always finish their drugs, or take the wrong ones, allowing for highly transmissible, drug-resistant strains of TB to emerge and spread amongst the population.
MDR-TB is harder and more expensive to treat, and the current vaccine is largely ineffective. The most common diagnostic technique can determine that Mycobacterium tuberculosis is present, but not whether it’s MDR.
Several drugs are currently being developed to treat MDR-TB. But currently TB is one of the world’s leading killers, killing 1.4 million people worldwide and caused 8.7 million new and relapse infections in 2011. One-third of the world’s population carries the bacterium, but most will never develop an active form of the disease.
Resistance starts to develop when patients don’t follow their drug regimens, which typically last six months for drug-sensitive TB and 20 months for MDR-TB. This allows naturally-occurring resistant mutants to grow and evolve, putting more people at risk. MDR-TB is resistant to isoniazid and rifampicin, but can be treated with second-line drugs, broad-spectrum antibiotics, like fluoroquinolones or injectable agents like amikacin, capreomycin, and kanamycin. These treatments are less effective, more toxic and take many more months to work. XDR-TB is resistant to fluoroquinolones and at least one of the injectable agents.
The decline in some countries’ healthcare infrastructure since the 1990s has meant that some patients aren’t diagnosed with TB and treated. In some countries, the over-the-counter availability of anti-TB drugs encouraged patients to take inappropriate second-line therapies, accelerating the growth of drug resistance.
The private sector has had little incentive to invest in research to create anti-MDR-TB vaccines, since if any eventual products emerge, they would be sold at low cost in poor countries. There are currently ten TB drugs in clinical trial. The aim is to create compounds that are effective against MDR-TB, work faster and have fewer side effects.
Accurate and fast diagnostic tests for MDR-TB strains are a part of keeping it under control. In December 2011, clinicians in Mumbai, India, reported the identification of 12 patients with totally drug-resistant TB (TDR-TB). There have been additional claims, but the WHO concluded that there wasn’t enough evidence to say that TDR-TB was substantially different from XDR-TB.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.