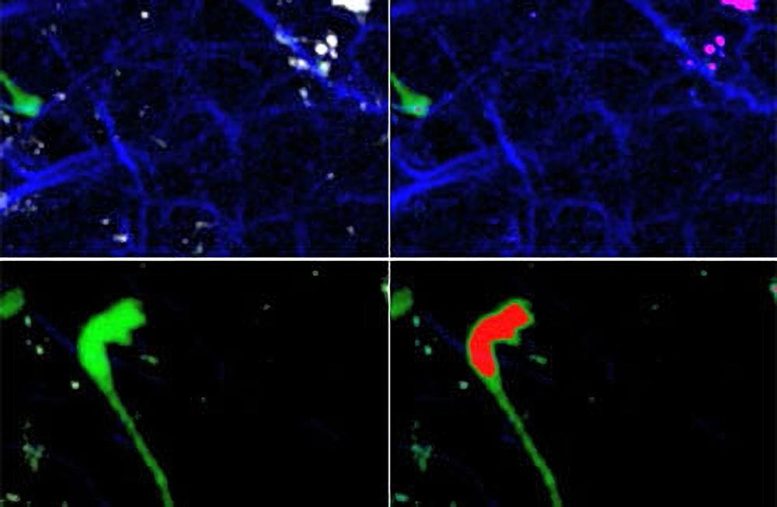
Visualizing HIV migration: These images from the lymph node of a live humanized mouse show several HIV-infected T cells (green) that have fused, forming one giant cell called a syncytium. Since T cells move a great deal in lymph nodes, the fused cells pull in different directions, but membrane bridges keep them together. The infected cells express a modified version of the green fluorescent protein that marks cell nuclei (highlighted in red in the right hand panel). Images courtesy of Thorsten Mempel.
Using the humanized BLT mouse model, a new study is the first to visualize the behavior of HIV-infected human T cells within a lymph node of a live animal, showing tethering interactions between infected and uninfected CD4-expressing cells.
Researchers have discovered one more way the human immunodeficiency virus (HIV) exploits the immune system. Not only does HIV infect and destroy a class of immune cells called CD4-positive helper T cells – which normally direct and support the infection-fighting activities of other immune cells – the virus also appears to use those cells to travel through the body and infect other CD4 T cells.
The study, which appeared online on August 1 in the journal Nature is the first to visualize the behavior of HIV-infected human T cells within a lymph node of a live animal, using a recently developed “humanized” mouse model of HIV infection.
“We have found that HIV disseminates in the body of an infected individual by ‘hitching a ride’ on the T cells it infects,” said study senior author Thorsten Mempel, HMS assistant professor of medicine at Massachusetts General Hospital. “Infected T cells continue doing what they usually do, migrating within and between tissues such as lymph nodes, and in doing so they carry HIV to remote locations that free viruses could not reach as easily. There are drugs that can manipulate the migration of T cells that potentially could be used to help control the spread of virus within a patient.”
When HIV enters blood or tissues, the virus binds to CD4 molecules on the surface of helper T cells, injecting its contents and initiating a process that leads to the assembly and release of new virus particles. It has long been assumed that the virus travels by diffusion through tissue fluids where it seeks out new cells to infect.
But recent studies have suggested that HIV can also pass directly from cell to cell when structures called virological synapses form during long-lasting interactions between T cells. Since CD4 T cells usually migrate quickly and form only transient contacts with other cells, the current study was designed to examine whether HIV alters the migration of infected T cells, allowing the kind of persistent contact that facilitates the spread of infection.
Researchers used the humanized BLT mouse model, the only non-primate that can be infected with HIV. After first confirming that human T cells enter and normally migrate within the animals’ lymph nodes – known to be important sites of HIV replication – the researchers injected the animals with HIV engineered to express green fluorescent protein (GFP), allowing them to track cell movement using a method called intravital microscopy. They first observed that, within two days, infected T cells continued to migrate and were uniformly distributed within lymph nodes but remained in nodes closest to the site of injection.
While the HIV-infected cells actively moved within lymph nodes, they did not move as quickly as the uninfected T cells, with some forming abnormally long and thin extensions that appeared to trail behind moving cells. The researchers hypothesized that the HIV envelope protein might cause infected cells to form tethering contacts with uninfected cells, producing these extensions. A series of experiments verified that the elongated shape of some infected cells requires the presence of the envelope protein. What’s more, many of these cells contained multiple nuclei, suggesting they had been formed by the fusion of several cells.
To test the role of T cell migration in HIV infection, the researchers injected another group of BLT mice with HIV and at the same time treated them with an agent that prevents T cells from leaving lymph nodes. Two months later, levels of HIV in the bloodstream and in lymph nodes distant from the site of injection were much lower than in untreated HIV-infected animals, further evidence that T cells carry the virus throughout the body. The migration-suppressing agent, however, did not reduce viral levels in animals with already-established HIV infection.
“While our observation of tethering interactions between infected and uninfected CD4-expressing cells suggest that HIV may be transmitted between T cells by direct contact, we will have to clearly show this in future studies and explore how important it is relative to the transmission by free virus,” said Mempel. He added that the availability of the BLT mouse was instrumental in their ability to carry out this study. “This approach provides a new vantage point to investigate previously unexplored aspects of HIV pathogenesis.”
Reference: “HIV-infected T cells are migratory vehicles for viral dissemination” by Thomas T. Murooka, Maud Deruaz, Francesco Marangoni, Vladimir D. Vrbanac, Edward Seung, Ulrich H. von Andrian, Andrew M. Tager, Andrew D. Luster and Thorsten R. Mempel, 1 August 2012, Nature.
DOI: 10.1038/nature11398
The study was supported by grants from the National Institutes of Health and the Ragon Institute of MGH, MIT, and Harvard.








Be the first to comment on "First Visualization of the Behavior of HIV Infected Human T Cells"