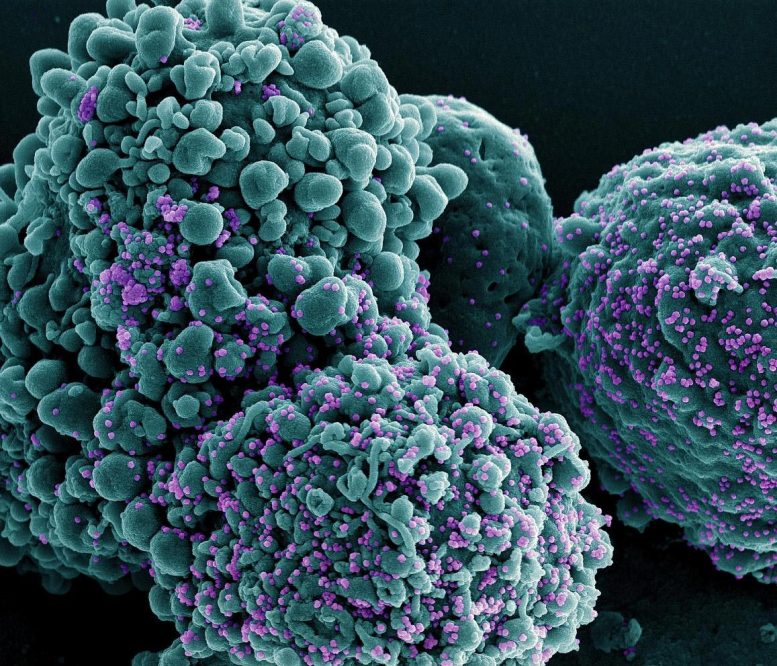
COVID-19 rebound after Paxlovid appears linked to a strong immune response rather than impaired immunity or resistance. Robust T-cell responses were detected, suggesting the need for further studies on treatment duration.
Findings from a small study of eight patients suggest that COVID-19 rebound is likely not caused by impaired immune responses. The study, led by scientists at the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health (NIH), was published on October 6 in Clinical Infectious Diseases. It aimed to define the clinical course and the immunologic and virologic characteristics of COVID-19 rebound in patients who have taken nirmatrelvir/ritonavir (Paxlovid), an antiviral therapeutic developed by Pfizer, Inc.
According to the Centers for Disease Control and Prevention (CDC), COVID-19 rebound is characterized by a recurrence of COVID-19 symptoms and/or a new positive viral test after having tested negative. The findings, according to the study’s authors, do not corroborate the idea that a five-day Paxlovid course is too brief for the body to mount a potent defense against SARS-CoV-2, the virus that causes COVID-19.
The goal of the research was to better understand how SARS-CoV-2 affects white blood cells. Participants were selected from adults enrolled in an ongoing COVID-19 study at the NIH Clinical Center in Bethesda, Maryland, and other local hospitals. As part of the study, participants provided blood and other samples as well as access to their COVID-19 medical records.
Six participants (three men and three women with a median age of 42 years) who took Paxlovid within four days of initial symptom onset and then experienced recurrent symptoms were included in the study to evaluate COVID-19 rebound. Two participants (a 54-year-old man and a 35-year-old woman) experienced recurrent symptoms and did not take Paxlovid. Finally, a control group included six people who had COVID-19 but did not experience symptom rebound. All participants were previously vaccinated and boosted against COVID-19, and none developed severe disease requiring hospitalization during acute infection or rebound. Investigators collected data on each participant’s clinical course and performed laboratory tests on blood and nasal swab samples.
Key Findings on Immune Response and Viral Characteristics
Researchers found no evidence of genetic mutations that would indicate participants who experienced COVID-19 rebound were infected with a strain of SARS-CoV-2 that was resistant to Paxlovid. Additionally, they found no evidence of delayed development of antibodies in participants experiencing rebound after taking Paxlovid. In fact, investigators detected robust SARS-CoV-2 T-cell responses in rebound patients. Overall, the level of T-cell responses was greater in rebound patients than in patients with early acute COVID-19 who did not experience rebound. Infectious SARS-CoV-2 was detected by viral culture in one out of eight rebound participants.
According to the authors, the findings indicate that rebound symptoms could be partially driven by the robust cellular immune response to residual viral RNA throughout the respiratory tract, rather than an impaired immune response allowing viral replication. Larger, more detailed epidemiologic studies are needed to further understand the clinical importance and epidemiologic consequences of COVID-19 rebound, the authors write. The authors note that the current data support the need for isolation in symptomatic rebound persons and the need to evaluate, in a clinical trial, longer courses of Paxlovid in immunocompromised individuals where the immune response may be ineffective.
Reference: “Clinical, Virologic, and Immunologic Evaluation of Symptomatic Coronavirus Disease 2019 Rebound Following Nirmatrelvir/Ritonavir Treatment” by Brian P Epling, Joseph M Rocco, Kristin L Boswell, Elizabeth Laidlaw, Frances Galindo, Anela Kellogg, Sanchita Das, Allison Roder, Elodie Ghedin, Allie Kreitman, Robin L Dewar, Sophie E M Kelly, Heather Kalish, Tauseef Rehman, Jeroen Highbarger, Adam Rupert, Gregory Kocher, Michael R Holbrook, Andrea Lisco, Maura Manion, Richard A Koup and Irini Sereti, 6 October 2022, Clinical Infectious Diseases.
DOI: 10.1093/cid/ciac663
Irini Sereti, M.D., chief of the HIV Pathogenesis Section in the Laboratory of Immunoregulation, part of NIAID’s Division of Intramural Research, is available for comment.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
Made chronically mildly (potentially disabling and deadly) ill with US FDA approved non-IgE-mediated mild food allergy aggravating added ‘cultured-free’ monosodium glutamate (MSG) since 1980, aggravated with modified soy protein mostly processed with toxic hexane with some residue since the early 1970s, hospitalized with a heart attack ‘scare’ in late 2015 following two tiny doses of the FDA approved cooking oil preservative TBHQ in one day, suffering a self-discovered serious calcium deficiency in 2010 resultant of avoiding good nutritional quality animal food products for allergy reasons since 1980, briefly urinating red after five days of hospital stay FDA approved prescription blood pressure meds in 2017 until quitting the meds, suffering a few days up to three months of crippling, painful gout or pseudogout from FDA approved propylene glycol in combination with cocoa or chocolate by 2021 and still addressing a very serious phosphorus deficiency self-discovered in mid-March of 2021 during a phony for-profit $6 Trillion Covid-19 pandemic still in progress while about 4,000 unsuspecting Americans still die prematurely daily from undiagnosed allergies and FDA approved food poisoning; first writing the FDA (with replies) in October of 2005 about allergies, added MSG, chronic disease and the then still recently announced “obesity epidemic” (obviously, now, in-vain), I estimate about 20 million premature American deaths (including most of my immediate family) could have been cheaply and easily prevented by now. Still struggling to stay healthy, at age 78, I’m supposed to believe anything the US Government says about diet, nutrition and/or health; not happening! And, so-called “modern medicine” is still so “dark-ages.”