
Researchers Are Exploring Possible Effects on the Brain
Neurodegenerative diseases like Alzheimer’s are among the most puzzling in medical research. The underlying causes of these conditions might be anything from dietary influences and lifestyle decisions to genetic factors and general cardiovascular health.

Various environmental pollutants have also been linked to the development or progression of neurological illness. Among them is glyphosate, a broad-spectrum herbicide. Glyphosate is a widely used herbicide that is used on agricultural crops all over the globe.
Joanna Winstone, Ramon Velazquez, and their colleagues at the Translational Genomics Research Institute (TGen) investigate the consequences of glyphosate exposure on the brains of mice in a new study. For the first time, the study shows that glyphosate can successfully cross the blood-brain barrier and enter the brain. Once there, it raises levels of a key factor known as TNF-α (for tumor necrosis factor alpha).
TNF-α is a molecule with two faces. This pro-inflammatory cytokine is essential in the neuroimmune system, functioning to boost immune response and protect the brain. (Cytokines are a broad category of small proteins that are essential for proper cell signaling.)
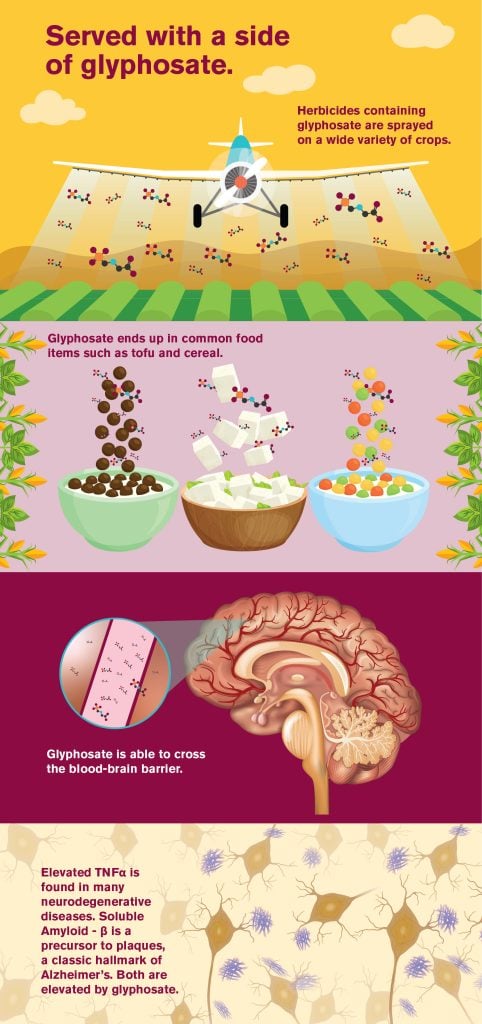
When levels of TNF-α are dysregulated, however, a host of diseases linked with neuroinflammation can result. Among these is Alzheimer’s disease.

The study further demonstrates in cell culture studies that glyphosate exposure appears to increase the production of soluble beta-amyloid (Aβ) and reduce the viability of neurons. The accumulation of Aβ, the sticky protein responsible for the formation of Aβ plaques, is one of the central diagnostic hallmarks of Alzheimer’s disease.
Further evidence suggestive of potential hazards to neurological health was observed when the researchers examined changes in gene expression via RNA sequencing in the brains of mice following glyphosate exposure.
These RNA transcripts hinted at disruptions in the expression of genes related to neurodegenerative disease, including dysregulation of a class of brain cells responsible for producing the myelin sheath critical for proper neuronal communication. These cells, known as oligodendrocytes, are affected by elevated levels of TNF-α.
“We find increases in TNF-α in the brain, following glyphosate exposure,” Velazquez says. “While we examined AD pathology, this might have implications for many neurodegenerative diseases, given that neuroinflammation is seen in a variety of brain disorders.”
An Enigmatic Disease. A Path of Destruction.
A hundred years have passed since the first diagnosis of Alzheimer’s disease. Despite vast investments in research and drug development, the affliction remains without effective treatment. A suite of therapies, developed over many decades at extravagant cost, have one by one failed to alleviate the symptoms of the disease.
Alzheimer’s disease is the most common form of dementia. The progression of the disease usually begins with mild memory loss. As the disease develops, increasing confusion and a breakdown in communication abilities often result, as the affliction attacks brain pathways involved in memory, language, and thought.
Some 5.8 million Americans are living with Alzheimer’s disease, as of 2020, according to the Centers for Disease Research. Unlike heart disease or cancer, the death toll for Alzheimer’s disease is on a frightening upward trajectory. By 2040, the costs of the disease are projected to rise dramatically to between $379 and more than $500 billion annually. The staggering toll of the illness is currently projected to nearly triple to 14 million people by 2050.
The onset of symptoms typically occurs after age 60 and the risk to individuals doubles every 5 years after age 65. Although genetics are believed to play a role in some cases of Alzheimer’s disease, and a family history of the disorder is considered a significant risk factor, environmental factors are believed to play a significant role in the disease.
Researchers are trying to learn how genetic correlates may subtly interact with environmental and other factors to decrease or enhance the likelihood of developing the affliction. Some recent research suggests that lifestyle changes, including proper physical activity, nutritious food, limited alcohol consumption, and not smoking may help prevent or slow cognitive decline, noting that brain and cardiovascular health are closely linked.
Toxic Effects: the Jury Is Out
The new study examines the neurological effects of glyphosate, the most ubiquitous herbicide in global use. Each year, around 250 million pounds of glyphosate are applied to agricultural crops in the U.S. alone. Although the chemical is regarded as generally safe for humans by the Environmental Protection Agency and the European Food Safety Authority, researchers are taking a second look.
Studies of acute herbicide use suggest they are non-harmful, but little is known about possible long-term effects from prolonged exposure. One issue of considerable concern is that glyphosate can cross the blood-brain barrier, a layer of endothelial cells preventing dissolved substances in the circulating bloodstream from readily passing into the extracellular fluid of the central nervous system, where the brain’s neurons reside.
Potential risks to brain health posed by glyphosate should be critically evaluated, particularly for those consistently exposed to the herbicide. “The Alzheimer’s connection is that there’s a much higher prevalence of Alzheimer’s disease in agricultural communities that are using this chemical,” Winstone says. “We’re trying to establish a more molecular-science-based link between the two.”
The study exposed mice to high doses of glyphosate, then detected elevated levels of TNF-α in their brains. The researchers then exposed extracted mouse neurons in Petri dishes to the same levels of glyphosate detected in the brains of mice, observing elevated amyloid beta and cell death in cortical neurons. Dysregulated oligodendrocyte RNA transcripts, which could indicate disruption of myelination, were detected in brain tissue.
Taken together, the results demonstrate a correlation between glyphosate exposure and classic symptoms of AD, though the authors stress that much more work will be required before a causative link can be established.
Nevertheless, the widespread use of the chemical and the disturbing correlates highlighted in the current study underscore the need for intensified investigation. Among the pressing questions to be answered: how does prolonged, low-dose exposure to glyphosate affect the brain; does glyphosate act synergistically with other chemicals present in common herbicides; and can glyphosate be detected post-mortem in patients who died of Alzheimer’s disease?
On the horizon, new drugs designed to reduce TNF-α in the brain are being explored, offering renewed hope for those with Alzheimer’s disease as well as other neurodegenerative ailments.
Reference: “Glyphosate infiltrates the brain and increases pro-inflammatory cytokine TNFα: implications for neurodegenerative disorders” by Joanna K. Winstone, Khyatiben V. Pathak, Wendy Winslow, Ignazio S. Piras, Jennifer White, Ritin Sharma, Matthew J. Huentelman, Patrick Pirrotte and Ramon Velazquez, 28 July 2022, Journal of Inflammation.
DOI: 10.1186/s12974-022-02544-5
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
3 Comments
Ridiculous fear mongering. Petri dish tests are not real life situations. The whole thing is not relevant unless one can first proven that the molecule can get to the barrier in large enough quantities to be of any biological significance. The authors of this article need to be fired.
Similar in time frame (e.g. glyphosate herbicide, patented in 1974 and added ‘cultured-free’ monosodium glutamate; MSG; FDA approved for expanded use in 1980), with a family and personal history of food allergies and dementia and my personal occasional use of Roundup week killer experience and statistics inform me it is toxic FDA approved added MSG that is most closely related to the Alzheimer’s Disease epidemic/pandemic and that which should be researched, first and foremost. Also, my kind of food allergies being a major factor, how does one determine if a mouse or mouse brain neuron in a petri dish has/had a kind of food allergies which mainstream medicine is still unable to diagnose in humans?
… Oh my God!
This is such a surprise to me that I can’t tell a word for a while… Common people, we all know that most of that chemistry is bad for humans and other things…