
The sensor technology could also be used to create clothing that detects a variety of pathogens and other threats.
Engineers at MIT and Harvard University have designed a novel face mask that can diagnose the wearer with COVID-19 within about 90 minutes. The masks are embedded with tiny, disposable sensors that can be fitted into other face masks and could also be adapted to detect other viruses.
The sensors are based on freeze-dried cellular machinery that the research team has previously developed for use in paper diagnostics for viruses such as Ebola and Zika. In a new study, the researchers showed that the sensors could be incorporated into not only face masks but also clothing such as lab coats, potentially offering a new way to monitor health care workers’ exposure to a variety of pathogens or other threats.
“We’ve demonstrated that we can freeze-dry a broad range of synthetic biology sensors to detect viral or bacterial nucleic acids, as well as toxic chemicals, including nerve toxins. We envision that this platform could enable next-generation wearable biosensors for first responders, health care personnel, and military personnel,” says James Collins, the Termeer Professor of Medical Engineering and Science in MIT’s Institute for Medical Engineering and Science (IMES) and Department of Biological Engineering and the senior author of the study.
The face mask sensors are designed so that they can be activated by the wearer when they’re ready to perform the test, and the results are only displayed on the inside of the mask, for user privacy.
Peter Nguyen, a research scientist at Harvard University’s Wyss Institute for Biologically Inspired Engineering, and Luis Soenksen, a Venture Builder at MIT’s Abdul Latif Jameel Clinic for Machine Learning in Health and a former postdoc at the Wyss Institute, are the lead authors of the paper, which appears today in Nature Biotechnology.
Wearable Sensors
The new wearable sensors and diagnostic face mask are based on technology that Collins began developing several years ago. In 2014, he showed that proteins and nucleic acids needed to create synthetic gene networks that react to specific target molecules could be embedded into paper, and he used this approach to create paper diagnostics for the Ebola and Zika viruses. In work with Feng Zhang’s lab in 2017, Collins developed another cell-free sensor system, known as SHERLOCK, which is based on CRISPR enzymes and allows highly sensitive detection of nucleic acids.
These cell-free circuit components are freeze-dried and remain stable for many months, until they are rehydrated. When activated by water, they can interact with their target molecule, which can be any RNA or DNA sequence, as well as other types of molecules, and produce a signal such as a change in color.
More recently, Collins and his colleagues began working on incorporating these sensors into textiles, with the goal of creating a lab coat for health care workers or others with potential exposure to pathogens.
First, Soenksen performed a screen of hundreds of different types of fabric, from cotton and polyester to wool and silk, to find out which might be compatible with this kind of sensor. “We ended up identifying a couple that are very widely used in the fashion industry for making garments,” he says. “The one that was the best was a combination of polyester and other synthetic fibers.”
To make wearable sensors, the researchers embedded their freeze-dried components into a small section of this synthetic fabric, where they are surrounded by a ring of silicone elastomer. This compartmentalization prevents the sample from evaporating or diffusing away from the sensor. To demonstrate the technology, the researchers created a jacket embedded with about 30 of these sensors.
They showed that a small splash of liquid containing viral particles, mimicking exposure to an infected patient, can hydrate the freeze-dried cell components and activate the sensor. The sensors can be designed to produce different types of signals, including a color change that can be seen with the naked eye, or a fluorescent or luminescent signal, which can be read with a handheld spectrometer. The researchers also designed a wearable spectrometer that could be integrated into the fabric, where it can read the results and wirelessly transmit them to a mobile device.
“This gives you an information feedback cycle that can monitor your environmental exposure and alert you and others about the exposure and where it happened,” Nguyen says.
A Diagnostic Face Mask
As the researchers were finishing up their work on the wearable sensors early in 2020, COVID-19 began spreading around the globe, so they quickly decided to try using their technology to create a diagnostic for the SARS-CoV-2 virus.
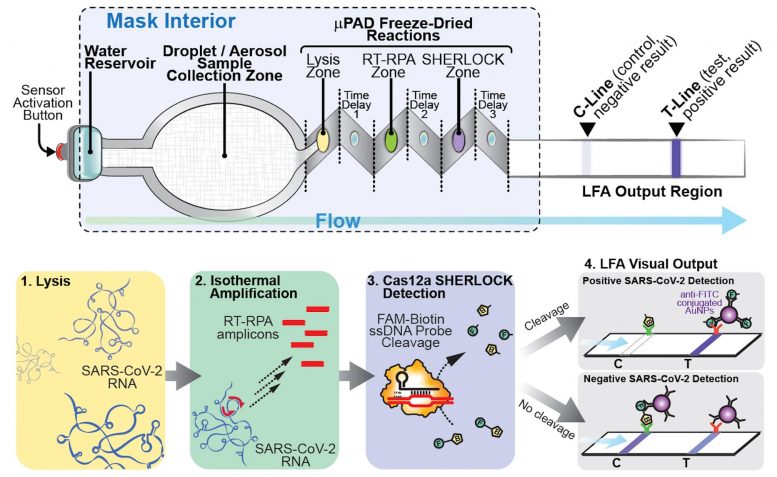
To produce their diagnostic face mask, the researchers embedded freeze-dried SHERLOCK sensors into a paper mask. As with the wearable sensors, the freeze-dried components are surrounded by silicone elastomer. In this case, the sensors are placed on the inside of the mask, so they can detect viral particles in the breath of the person wearing the mask.
The mask also includes a small reservoir of water that is released at the push of a button when the wearer is ready to perform the test. This hydrates the freeze-dried components of the SARS-CoV-2 sensor, which analyzes accumulated breath droplets on the inside of the mask and produces a result within 90 minutes.
“This test is as sensitive as the gold standard, highly sensitive PCR tests, but it’s as fast as the antigen tests that are used for quick analysis of COVID-19,” Nguyen says.
The prototypes developed in this study have sensors on the inside of the mask to detect a user’s status, as well as sensors placed on the outside of garments, to detect exposure from the environment. The researchers can also swap in sensors for other pathogens, including influenza, Ebola, and Zika, or sensors they have developed to detect organophosphate nerve agents.
“Through these demonstrations we have essentially shrunk down the functionality of state-of-the-art molecular testing facilities into a format compatible with wearable scenarios across a variety of applications,” Soenksen says.
The researchers have filed for a patent on the technology and they are now hoping to work with a company to further develop the sensors. The face mask is most likely the first application that could be made available, Collins says.
“I think the face mask is probably the most advanced and the closest to a product. We have already had a lot of interest from outside groups that would like to take the prototype efforts we have and advance them to an approved, marketed product,” he says.
Reference: “Wearable materials with embedded synthetic biology sensors for biomolecule detection” by Peter Q. Nguyen, Luis R. Soenksen, Nina M. Donghia, Nicolaas M. Angenent-Mari, Helena de Puig, Ally Huang, Rose Lee, Shimyn Slomovic, Tommaso Galbersanini, Geoffrey Lansberry, Hani M. Sallum, Evan M. Zhao, James B. Niemi and James J. Collins, 28 June 2021, Nature Biotechnology.
DOI: 10.1038/s41587-021-00950-3
The research was funded by the Defense Threat Reduction Agency; the Paul G. Allen Frontiers Group; the Wyss Institute; Johnson and Johnson Innovation JLABS; the Ragon Institute of MGH, MIT and Harvard; and the Patrick J. McGovern Foundation.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
2 Comments
How does this distinguish between SARS-COV2 and other coronaviruses that are also circulating around us?
What is the sensitivity and specificity of the prototype?