
In an effort to increase global awareness and to better detect signs of infectious diseases around the world, engineers at UCLA have developed a compact and cost-effective RDT-reading device that works in tandem with standard cell phones.
In the fight against emerging public health threats, early diagnosis of infectious diseases is crucial. And in poor and remote areas of the globe where conventional medical tools like microscopes and cytometers are unavailable, rapid diagnostic tests, or RDTs, are helping to make disease screening quicker and simpler.
RDTs are generally small strips on which blood or fluid samples are placed. Specific changes in the color of the strip, which usually occur within minutes, indicate the presence of infection. Different tests can be used to detect various diseases, including HIV, malaria, tuberculosis and syphilis.
While the advantages of RDTs are significant — better disease management, more efficient surveillance of outbreaks in high-risk areas, and the ability of minimally trained technicians to test large numbers of individuals — they can also present problems.
“Conventional RDTs are currently read manually, by eye, which is prone to error, especially if various different types of tests are being used by the health care worker,” said Aydogan Ozcan, a University of California, Los Angeles (UCLA) professor of electrical engineering and bioengineering.
To address such challenges, Ozcan and his colleagues from the UCLA Henry Samueli School of Engineering and Applied Science and the California NanoSystems Institute at UCLA have developed a compact and cost-effective RDT-reading device that works in tandem with standard cell phones.
“What we have created is a digital ‘universal’ reader for all RDTs, without any manual decision-making,” he said.
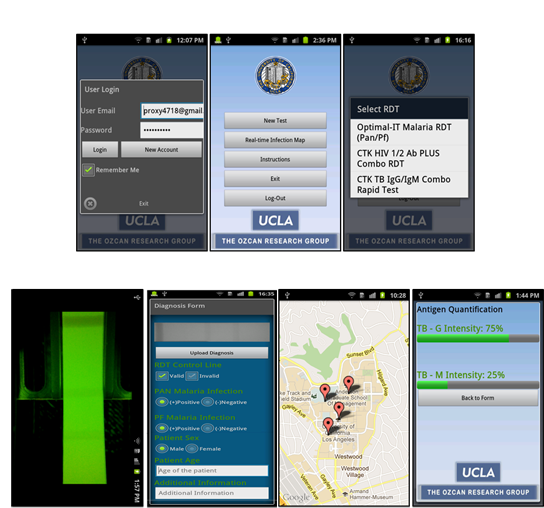
The RDT-reader attachment, which clips onto a cell phone, weighs approximately 65 grams and includes an inexpensive lens, three LED arrays and two AAA batteries. The platform has the ability to read nearly every type of RDT. An RDT strip is inserted into the attachment, and with the help of cell phone’s existing camera unit and a special smart-phone application, the strip is converted into a digital image.
The platform then rapidly reads the digitized RTD image to determine, first, whether the test is valid and, second, whether the results are positive or negative, thus eliminating the potential errors that can occur with a human reader, especially one administering multiple tests of various test types. And because the color changes in RDTs don’t last more than a few hours in the field, the ability to store the digitized image indefinitely provides an added benefit.
After this step, the RDT-reader platform wirelessly transmits the results of the tests to a global server, which processes them, stores them and, using Google Maps, creates maps charting the spread of various diseases and conditions — both geographically and over time — throughout the world.
Together, the universal RDT reader and the mapping feature, which have been implemented on both iPhones and Android-based smart-phones, could significantly increase our ability to track emerging epidemics worldwide and aid in epidemic preparedness, the researchers say.
“This platform would be quite useful for global health professionals, as well as for policymakers, to understand cause–effect relationships at a much larger scale for combating infectious diseases,” Ozcan said.
The research is published in the journal Lab on a Chip.
Reference: “Integrated rapid-diagnostic-test reader platform on a cellphone” by Onur Mudanyali, Stoyan Dimitrov, Uzair Sikora, Swati Padmanabhan, Isa Navruz and Aydogan Ozcan, 16 April 2012, Lab on a Chip.
DOI: 10.1039/C2LC40235A
Additional authors of the study include Onur Mudanyali (first author), Stoyan Dimitrov, Uzair Sikora, Swati Padmanabhan, and Isa Navruz, all of the department of electrical engineering at the UCLA Henry Samueli School of Engineering and Applied Science.
Ozcan and his UCLA research team have been developing a variety of cell-phone attachments that utilize the digital components already embedded in standard cell phones to aid in the fight against global disease. With more than 5 billion cell-phone subscribers around the world today, cell phones can play a central role in telemedicine applications, and existing wireless telecommunications infrastructure presents new opportunities for innovative cloud-based health-monitoring and management platforms, the researchers say.
Funding for the Ozcan Research Group is provided by the Presidential Early Career Award for Scientists and Engineers (PECASE), the ARO Young Investigator Award, the National Science Foundation CAREER Award (BISH program), the ONR Young Investigator Award, and the National Institutes of Health Director’s New Innovator Award.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
Bravo on RDT readers! As an ER doc, I congratulate all involved and all supporting this project. A global application that we can act local with. This is a fledgling science. I can see a time where the triage nurse has a patient suck on a viral and bacterial coded test strip in triage and by the time the patient reaches the doctor, the nurse/doctor reads his/her cell phone positive test result and definitively diagnose COVID-19, influenza H5N1, or RSV!!!! Bravo! Same can be run on saliva, stool, spit or blood!!! Amazing!!!