Groundbreaking Discovery in Migraine Brain Changes
For the first time, a new study has identified enlarged perivascular spaces in the brains of migraine sufferers. Results of the study were presented recently at the annual meeting of the Radiological Society of North America (RSNA).
“In people with chronic migraine and episodic migraine without aura, there are significant changes in the perivascular spaces of a brain region called the centrum semiovale,” said study co-author Wilson Xu, an M.D. candidate at Keck School of Medicine of the University of Southern California in Los Angeles. “These changes have never been reported before.”
Migraine is a common, often debilitating condition, involving a severe recurring headache. Migraines may also cause nausea, weakness, and light sensitivity. According to the American Migraine Foundation, over 37 million people in the U.S. are affected by migraine, and up to 148 million people worldwide suffer from chronic migraine.
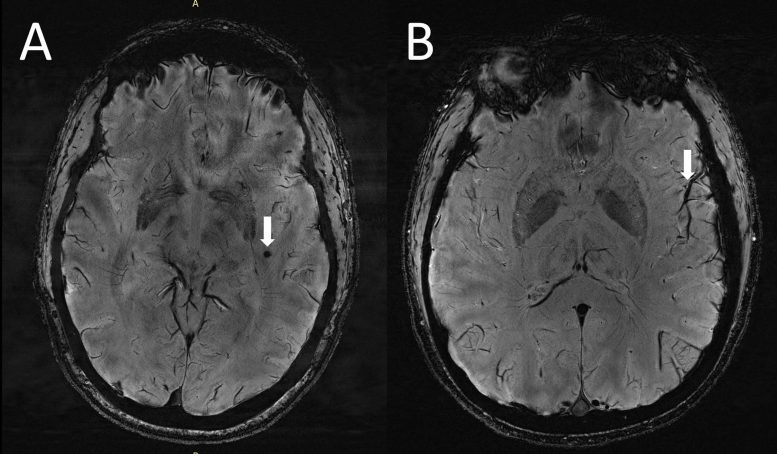
Perivascular spaces are fluid-filled spaces surrounding blood vessels in the brain. They are most commonly located in the basal ganglia and white matter of the cerebrum, and along the optic tract. Perivascular spaces are affected by several factors, including abnormalities at the blood-brain barrier and inflammation. Enlarged perivascular spaces can be a signal of underlying small vessel disease.
“Perivascular spaces are part of a fluid clearance system in the brain,” Xu said. “Studying how they contribute to migraine could help us better understand the complexities of how migraines occur.”
Using Ultra-High-Field MRI for Migraine Research
Xu and colleagues set out to determine the association between migraine and enlarged perivascular spaces. The researchers used ultra-high-field 7T MRI to compare structural microvascular changes in different types of migraine.
“To our knowledge, this is first study using ultra-high-resolution MRI to study microvascular changes in the brain due to migraine, particularly in perivascular spaces,” Xu said. “Because 7T MRI is able to create images of the brain with much higher resolution and better quality than other MRI types, it can be used to demonstrate much smaller changes that happen in brain tissue after a migraine.”
Study participants included 10 with chronic migraine, 10 with episodic migraine without aura, and five age-matched healthy controls. All patients were between 25 and 60 years old. Patients with overt cognitive impairment, brain tumor, prior intracranial surgery, MRI contraindications and claustrophobia were excluded from the study.
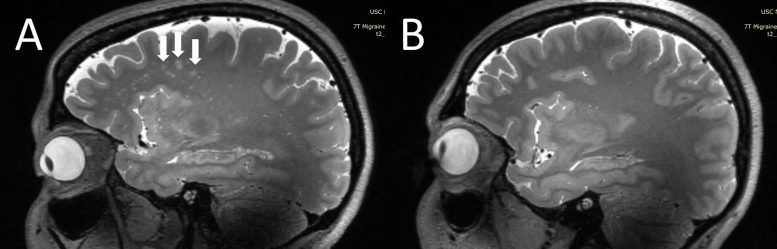
The researchers calculated enlarged perivascular spaces in the centrum semiovale (central area of white matter) and basal ganglia areas of the brain. White matter hyperintensities—lesions that “light up” on MRI—were measured using the Fazekas scale. Cerebral microbleeds were rated with the microbleed anatomical rating scale. The researchers also collected clinical data such as disease duration and severity, symptoms at time of scan, presence of aura and side of headache.
Enlarged Perivascular Spaces
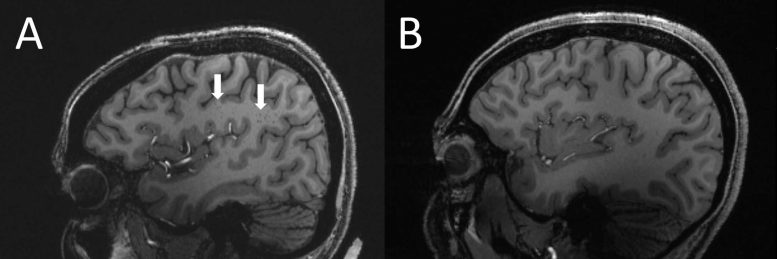
Statistical analysis revealed that the number of enlarged perivascular spaces in the centrum semiovale was significantly higher in patients with migraine compared to healthy controls. In addition, enlarged perivascular space quantity in the centrum semiovale correlated with deep white matter hyperintensity severity in migraine patients.
“We studied chronic migraine and episodic migraine without aura and found that, for both types of migraine, perivascular spaces were bigger in the centrum semiovale,” Xu said. “Although we didn’t find any significant changes in the severity of white matter lesions in patients with and without migraine, these white matter lesions were significantly linked to the presence of enlarged perivascular spaces. This suggests that changes in perivascular spaces could lead to future development of more white matter lesions.”
The researchers hypothesize that significant differences in the perivascular spaces in patients with migraine compared to the healthy controls might be suggestive of glymphatic disruption within the brain. The glymphatic system is a waste-clearance system that utilizes perivascular channels to help eliminate soluble proteins and metabolites from the central nervous system.
However, whether such changes affect migraine development or result from migraine is unknown. Continued study with larger case populations and longitudinal follow-up will better establish the relationship between structural changes and migraine development and type.
“The results of our study could help inspire future, larger-scale studies to continue investigating how changes in the brain’s microscopic vessels and blood supply contribute to different migraine types,” Xu said. “Eventually, this could help us develop new, personalized ways to diagnose and treat migraine.”
Co-authors are Brendon Chou, Giuseppe Barisano, Raymond Huang, Soniya Pinto, M.D., Daniel Chang Phung, M.D., Soma Sahai-Srivastava, Alexander Lerner, M.D., and Nasim Sheikh Bahaei, M.D., FRCR.
Meeting: 108th Scientific Assembly and Annual Meeting of the Radiological Society of North America
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
13 Comments
I was a migraine sufferer due to my menstrual cycle, with and without aura.
Since going through menopause I have not had any migraine attacks.
I had an MRI done many, many years ago which shows that I have scaring on my white matter. This just proves to me that migraines do damage parts of the brain. Not sure if the scaring heals itself.
Have had migraines my entire life. Ones that affect vision And sound and thought processes. 45 years… These scientists need to get with the scientist working on psuedotumor aka IIH maybe then they can see the bigger picture. And stop telling me Barometric pressure changes do not affect migraine sufferers!
I have helped some people with hemiplegic migraines become pain free by correcting abnormalities in the nose. Barometric pressure as a trigger is a key indicator the nose is the problem. A sinus ct scan shows the abnormal structures. You are welcome to call my office for more information,713-795-0600.
Finally! I was diagnosed with seizures as a child, they started just about the time of puberty. My vision would get fuzzy, my body – one side, my face and tongue would go numb and I couldn’t speak sometimes I couldn’t think right either. Eventually I “grew out” of them around the age of 13-14. At 26 I had a hysterectomy and shortly thereafter started menopause. Between the hormones or lack thereof, and weather changes I started getting the same symptoms of what I had as a child, but now diagnosed as migraines. I am not sure if I was misdiagnosed as a child, I had so many tests done and they recorded seizure activity in my brain while I slept. My father has debilitating migraines also. It would be great for scientists to figure out a way to help them without meds that cause more headaches or severe side effects.
I am an ent surgeon who has cured thousands by correcting abnormalities in the nose that cause the pain. Much like a Covid test swab hurts, these abnormalities do the same until removed.
I use a sinus ct scan to identify the abnormalities. It would be good to see if the MRI’s in this study shows the abnormalities I know cause the pain.
If you are interested in seeing if you are a candidate for my Smith Migraine Procedure, call the office for more information, 713-795-0600.
I was a severe migraine suffer for over 20 years. Once or twice a month. I researched, did what I could to at least be in a functionable state. Almost 20 yrs ago I had 3 colonics a month apart and I haven’t had a migraine since. I might feel symptoms which I treat but it might not be for everyone.
@ashley some of your symptoms sound similar to mine. Maybe look into hemiplegic migraines. They can cause the numbness and partial paralysis as well as the migraine symptoms. Getting the correct diagnosis helped me bc there are so many types of migraine. But I’m always excited when there is new information about migraine disease so I can try to understand what is happening to my brain.
Lea D. Amen!! I have been diagnosed with both IIH and chronic migraines. I take pills daily and get Botox and still suffer!
I correct abnormal structures in the nose and eliminate migraine pain. You are welcome to get a sinus ct scan and send it to me to review. For more information call my office and visit my Smith Center Facebook page for video testimonials, 713-795-0600
I’ve been having Migraine with aura for 55 years now since I was 12. I am lucky that they are not too frequent although frequency has varied over the years. When I was pregnant I had an event which doctors thought may have been a stroke or may have been hemiplegic migraine. I hope that these latest studies into brain changes in migraine sufferers eventually lead to effective preventative safe medication in future. At the moment I manage my migraines by taking pink migralieve to prevent vomiting and lying down with an ice pack on my temple. If I can manage to sleep for 2 hours I can usually resume normal activities but can feel delicate and a bit spaced out for the rest of the day. To people who have worse symptoms than I, you have my sympathy.
Let’s start the new year off with a proper diagnosis. I eliminate migraines in people by correcting abnormal structures in the nose. The nose is largely ignored as a source of pain however, Covid tests demonstrate just how sensitive it is when swabs are placed to collect a sample. You are welcome to get a sinus scan and send it to me to see what abnormal structures you have. My office is available for more information and my Smith Center Facebook page has lots of videos, 713-795-0600.
Was this published? Anyone know the name of the article?
Yes, Virchow Robinson Spaces ( prominent perivascular spaces) and multiple lucunar infarcts. I suffer from migraines with aura, epilepsy and I’m trying to find out what encalophmalcia in the bilateral caudal aspect of Basel ganglia means. I wished a doctor would just talk to me, I would like to understand