Stanford cancer team uses the custom molecule sBCMA-Fc V3 to inhibit the development of diffuse large B cell lymphoma and multiple myeloma in mice.
Researchers at Stanford University have created “decoy receptor” molecules that prevent the development of diffuse large B cell lymphoma (DLBCL) and multiple myeloma (MM) in mice.
The molecules, which were recently described in a study published in the Journal of Experimental Medicine (JEM), were also found to be nontoxic in monkeys, indicating they could be used to treat people with either of these deadly conditions, which are two of the most prevalent blood cancers in the world.
Both MM and DLBCL are cancers that arise from the body’s B cells, which make antibodies. Less than 60% of patients who have one of these conditions will survive five years.
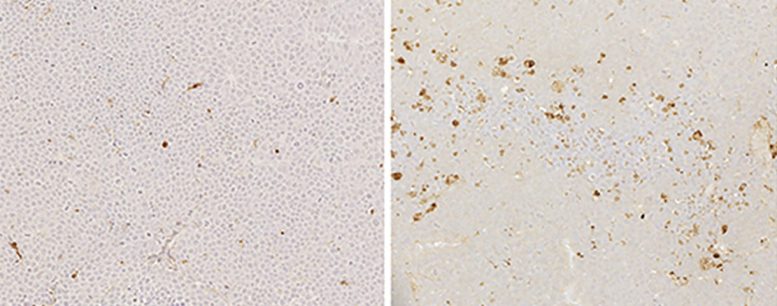
In recent years, several patients have seen success using genetically modified CAR T cells to target and destroy cancerous B cells. However, this immunotherapeutic strategy often has serious side effects and is unsuitable for older individuals, one of the most common types of people who have MM and DLBCL.
“Safe and effective targeted therapies are therefore still needed for patients who exhaust currently available treatment options,” says Dr. Yu Rebecca Miao, an instructor in the Department of Radiation Oncology at Stanford University.
Miao co-led the new research with Stanford University’s Dr. Kaushik Thakkar and Professor Amato J. Giaccia, who currently works at the University of Oxford’s Oxford Institute for Radiation Oncology. The Medical Research Council UK provided partial funding for the research.
APRIL and BAFF: Potential Therapeutic Targets
Two cell signaling proteins called APRIL and BAFF were hypothesized to be potential therapeutic targets for MM and DLBCL by Miao and colleagues. APRIL and BAFF regulate the growth of healthy B cells by binding to several different cell surface receptor proteins.
However, increased levels of APRIL and BAFF encourage the development and survival of malignant B cells, promoting the spread of blood cancer and the development of treatment resistance. Particularly, APRIL is connected to the development of MM, while BAFF is connected to DLBCL.
BCMA is a B cell surface receptor that binds to both APRIL and BAFF. Miao and colleagues investigated whether a soluble version of BCMA, unattached to the B cell surface, would act as a “decoy receptor” to mop up excess APRIL and BAFF and prevent these proteins from driving the growth of cancerous B cells.
The researchers found that soluble BCMA was able to bind to APRIL and inhibit the growth of MM in mice. However, the decoy receptor only bound weakly to BAFF and was therefore unable to reduce the growth of DLBCL.
More Effective Decoy: sBCMA-Fc V3
Miao and colleagues, therefore, engineered a mutant version of soluble BCMA that binds strongly to both APRIL and BAFF. This molecule, dubbed sBCMA-Fc V3, was able to impede the growth of both MM and DLBCL in rodents.
Notably, sBCMA-Fc V3 also reduced the activity of APRIL and BAFF in cynomolgus monkeys without causing any significant side effects. This suggests that treatment with sBCMA-Fc V3 or similar decoy receptors could be safe and effective in humans.
“Collectively, our data support sBCMA-Fc V3 as a clinically viable candidate for the treatment of MM and DLBCL,” Miao says. “The biological functions of BAFF and APRIL are not limited to B cell malignancies but extend to autoimmune disorders and other diseases triggered by pathological B cells, suggesting an even broader clinical indication for sBCMA-Fc V3.”
Reference: “Developing high-affinity decoy receptors to treat multiple myeloma and diffuse large B cell lymphoma” by Yu Rebecca Miao, Kaushik Thakkar, Can Cenik, Dadi Jiang, Kazue Mizuno, Chenjun Jia, Caiyun Grace Li, Hongjuan Zhao, Anh Diep, Yu Xu, Xin Eric Zhang, Teddy Tat Chi Yang, Michaela Liedtke, Parveen Abidi, Wing-sze Leung, Albert C. Koong and Amato J. Giaccia, 26 July 2022, Journal of Experimental Medicine.
DOI: 10.1084/jem.20220214
The study was funded by the Silicon Valley Community Foundation, the Sydney Frank Foundation, the Kimmelman Fund, the Medical Research Council, the Cancer Prevention and Research Institute of Texas, and the Welch Foundation.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.