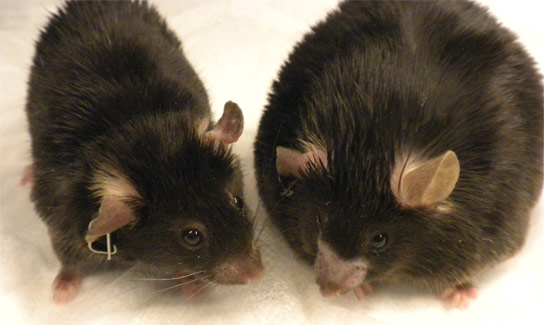
A newly published study from the University of Michigan found that a currently available asthma drug reverses obesity, diabetes and fatty liver in mice.
Researchers at the University of Michigan’s Life Sciences Institute have found that amlexanox, an off-patent drug currently prescribed for the treatment of asthma and other uses, also reverses obesity, diabetes, and fatty liver in mice.
The findings from the lab of Alan Saltiel, the Mary Sue Coleman director of the Life Sciences Institute, are published online in the journal Nature Medicine.
“One of the reasons that diets are so ineffective in producing weight loss for some people is that their bodies adjust to the reduced calories by also reducing their metabolism, so that they are ‘defending’ their body weight,” Saltiel said. “Amlexanox seems to tweak the metabolic response to excessive calorie storage in mice.”
Different formulations of amlexanox are currently prescribed to treat asthma in Japan and canker sores in the United States. Saltiel is teaming up with clinical-trial specialists at U-M to test whether amlexanox will be useful for treating obesity and diabetes in humans. He is also working with medicinal chemists at U-M to develop a new compound based on the drug that optimizes its formula.
The study appears to confirm and extend the notion that the genes IKKE and TBK1 play a crucial role for maintaining metabolic balance, a discovery published by the Saltiel lab in 2009 in the journal Cell.
“Amlexanox appears to work in mice by inhibiting two genes—IKKE and TBK1—that we think together act as a sort of brake on metabolism,” Saltiel said. “By releasing the brake, amlexanox seems to free the metabolic system to burn more, and possibly store less, energy.”
Using high-throughput chemical screening at LSI’s Center for Chemical Genomics to search for compounds that inhibit IKKE and TBK1, the researchers hit upon an approved off-patent drug: amlexanox. They then demonstrated that amlexanox had profound beneficial effects in both genetic and dietary-induced obese mice. The chemical lowered the weight of obese mice and reversed related metabolic problems such as diabetes and fatty liver.
“These studies tell us that, at least in mice, the IKKE/TBK1 pathway plays an important role in defending body weight by increasing storage and decreasing burning of calories, and that by inhibiting that pathway with a compound, we can increase metabolism and induce weight loss, reverse diabetes and reduce fatty liver,” Saltiel said.
The drug has been on the market in Japan for more than 25 years.
However, the researchers don’t yet know if humans respond with the same pathway, or if the discovery of amlexanox’s effectiveness in mice can lead to a compound that is safe and effective for treating obesity and diabetes in humans.
“We will be working hard on that,” Saltiel said.
Saltiel’s search for a drug targeting the IKKE/TBK1 pathway was supported by the Life Science Institute’s Innovation Partnership, which provides philanthropic funding and business mentorship to help move promising research toward commercialization.
Reference: “An inhibitor of the protein kinases TBK1 and IKK-ɛ improves obesity-related metabolic dysfunctions in mice” by Shannon M Reilly, Shian-Huey Chiang, Stuart J Decker, Louise Chang, Maeran Uhm, Martha J Larsen, John R Rubin, Jonathan Mowers, Nicole M White, Irit Hochberg, Michael Downes, Ruth T Yu, Christopher Liddle, Ronald M Evans, Dayoung Oh, Pingping Li, Jerrold M Olefsky and Alan R Saltiel, 10 February 2013, Nature Medicine.
DOI: 10.1038/nm.3082
Additional authors were Shannon M. Reilly, Shian-Huey Chiang, Stuart J. Decker, Louise Chang, Martha J. Larsen, John R. Rubin, Nicole M. White and Irit Hochberg from the Life Sciences Institute; Maeran Uhm and Jonathan Mowers from the Life Sciences Institute and Departments of Internal Medicine and Molecular and Integrative Physiology at the University of Michigan; Michael Downes, Ruth Yu and Ronald M. Evans from the Salk Institute for Biological Sciences; Christopher Liddle from the Storr Liver Unit, Westmead Millennium Institute and University of Sydney, Australia; and Dayoung Oh, Pingping Li, and Jerrold M. Olefsky from the Department of Medicine, University of California, San Diego.
Saltiel is the Mary Sue Coleman director of the Life Sciences Institute, where his laboratory is located and all his research is conducted. He is also the John Jacob Abel Collegiate Professor in the Life Sciences and a professor of internal medicine and molecular and integrative physiology at University of Michigan Medical School.
The research was also supported by the National Institutes of Health, the Michigan Diabetes Research and Training Center, the Michigan Institute for Clinical and Health Research, and the Nathan Shock Center in the Basic Biology of Aging.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
I kept waiting for the ” Of course it will be many years before we know if it works in humans or will be able to be taken by them.” So, maybe something will come of it, unless the drug and health care people stop it because curing diabetes and obesity would be very bad for their business and add to the unemployment problem.