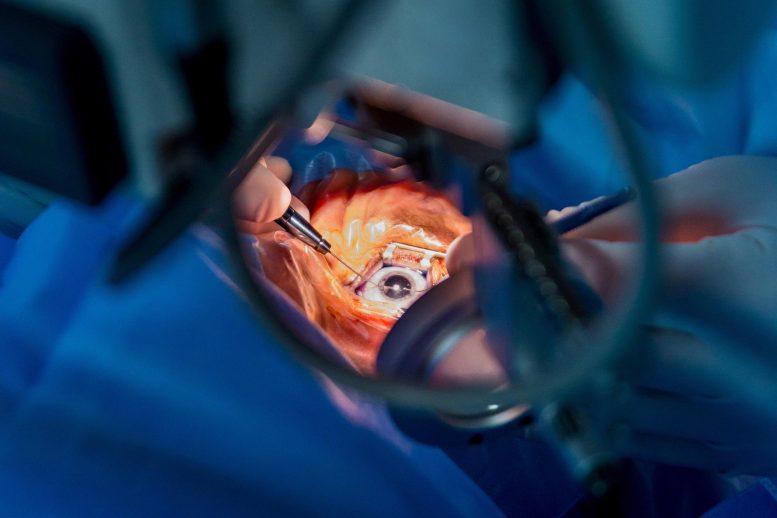
Co-developed by Harvard Medical School researchers and colleagues, a new computer-based simulation tool, the Cataract Master, aims to minimize clinical risk while providing residents and practicing ophthalmologists with the most authentic cataract surgical experience possible outside of the operating room.
Phacoemulsification cataract surgery is one of the most frequently performed eye surgeries in the United States, with 1.5 million procedures undertaken each year. It is also one of the most complex procedures to learn. A new, highly innovative, computer-based simulation tool, the Massachusetts Eye and Ear Infirmary (Mass. Eye and Ear) Cataract Master, bridges the learning gap that residents and ophthalmologists new to phaco must navigate prior to performing actual surgery.
Nearly a decade in the making, the Cataract Master was co-developed by Harvard Medical School’s (HMS) Bonnie An Henderson, assistant clinical professor of ophthalmology; John I. Loewenstein, ophthalmology residency training program director and an associate professor of ophthalmology; Adam Neaman; and several colleagues. Massachusetts Eye and Ear is a Harvard affiliate.

Ophthalmology residents typically train in wet labs and on phacoemulsification simulators that supplement motor skills training before moving on to live patients. The leap from lab to patient is challenging for surgeons-in-training, even with the most careful oversight by attending physicians.
“The Cataract Master aims to minimize clinical risk while providing residents and practicing ophthalmologists with the most authentic cataract surgical experience possible outside the OR,” Loewenstein said. “The goal is to boost skills and confidence, to better prepare residents for the surgical experience, and to raise the quality of patient care everywhere.”
Computer-based simulation technology has been used in medical training since the early 2000s, but these tools often did not take into account the hundreds of decision-making requirements that arise during surgery. The Cataract Master is different in that it offers a self-guided, self-correcting curriculum that requires trainees to make decisions based on realistic surgical situations. The simulator, which can be accessed from any personal computer, contains true-to-life animations along with videos of actual surgeries — complete with expert discussions of each phase of the procedure. The interactive program includes frequent pop-up questions relating to the various surgical steps, with user answers then animated on-screen. If the user makes a serious error, videos provide immediate feedback explaining how the problem occurred, what to do to fix it, and how to avoid making the same mistake again.
“This essentially allows new phaco surgeons to learn from their mistakes and to master lifelike surgery without risking injury to a patient,” said Henderson. “This type of immersion learning is simply not possible any other way, and [it] provides an excellent transition to the operating room.”
The Cataract Master, which is owned by Mass. Eye and Ear, is licensed to the not-for-profit American Society of Cataract and Refractive Surgery.
Funding for the development of this teaching tool was provided by the Massachusetts Lions Eye Research Fund, Norman Knight, the U.S. Army, and the Harvard Medical School Department of Ophthalmology.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.