A new gene therapy that inhibits targeted nerve cell signaling effectively reduced neuropathic pain in mice with spinal cord or peripheral nerve injuries with no detectable side effects.
In mouse studies, pain-blocking neurotransmitters produced long-lasting benefits without detectable side effects.
An international team of researchers led by scientists at the University of California San Diego School of Medicine reported that a gene therapy that inhibits targeted nerve cell signaling effectively reduced neuropathic pain in mice with spinal cord or peripheral nerve injuries with no detectable side effects.
The results, which were published in the online edition of Molecular Therapy on May 5, 2022, suggest a possible new treatment option for a condition that may affect more than half of individuals with spinal cord injuries. Neuropathy involves damage or dysfunction in nerves elsewhere in the body, typically resulting in chronic or debilitating numbness, tingling, muscle weakness, and pain.
There are no singularly effective remedies for neuropathy. Pharmaceutical therapy, for example, may need sophisticated, continuous medication administration and is linked with adverse side effects such as drowsiness and motor weakness. Opioids may be effective, but they can also develop tolerance and raise the risk of overuse or addiction.
Because physicians and researchers are able to pinpoint the precise location of a spinal cord injury and the origin of neuropathic pain, there has been much effort to develop treatments that selectively target impaired or damaged neurons in the affected spinal segments.
In recent years, gene therapy has proven an increasingly attractive possibility. In the latest study, researchers injected a harmless adeno-associated virus carrying a pair of transgenes that encode for gamma-aminobutyric acid or GABA into mice with sciatic nerve injuries and consequential neuropathic pain. GABA is a neurotransmitter that blocks impulses between nerve cells; in this case, pain signals.
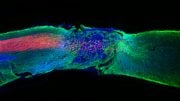
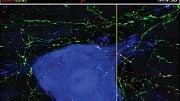
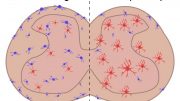
The delivery and expression of the transgenes — GAD65 and VGAT — were restricted to the area of sciatic nerve injury in the mice and, as a result, there were no detectable side effects, such as motor weakness or loss of normal sensation. The production of GABA by the transgenes resulted in measurable inhibition of pain-signaling neurons in the mice, which persisted for at least 2.5 months after treatment.

Senior study author Martin Marsala, MD, is a professor in the Department of Anesthesiology at UC San Diego School of Medicine. Credit: UC San Diego Health Sciences
“One of the prerequisites of a clinically acceptable antinociceptive (pain-blocking) therapy is minimal or no side effects like muscle weakness, general sedation or development of tolerance for the treatment,” said senior author Martin Marsala, MD, professor in the Department of Anesthesiology in the UC San Diego School of Medicine.
“A single treatment invention that provides long-lasting therapeutic effect is also highly desirable. These findings suggest a path forward on both.”
Reference: “Precision spinal gene delivery-induced functional switch in nociceptive neurons reverses neuropathic pain” by Takahiro Tadokoro, Mariana Bravo-Hernandez, Kirill Agashkov, Yoshiomi Kobayashi, Oleksandr Platoshyn, Michael Navarro, Silvia Marsala, Atsushi Miyanohara, Tetsuya Yoshizumi, Michiko Shigyo, Volodymyr Krotov, Stefan Juhas, Jana Juhasova, Duong Nguyen, Helena Kupcova Skalnikova, Jan Motlik, Hana Studenovska, Vladimir Proks, Rajiv Reddy, Shawn P. Driscoll, Thomas D. Glenn, Taratorn Kemthong, Suchinda Malaivijitnond, Zoltan Tomori, Ivo Vanicky, Manabu Kakinohana, Samuel L. Pfaff, Joseph Ciacci, Pavel Belan and Martin Marsala, 5 May 2022, Molecular Therapy.
DOI: 10.1016/j.ymthe.2022.04.023




“Opioids may be effective, but they can also develop tolerance and raise the risk of overuse or addiction.”
Don’t all pain meds share these qualities? Yes, but they do not share is opiods’ terrible reputation for destroying lives. Perhaps the pharmaceutical companies prefer this state of affairs.
In the 19th century, before the opium-based drugs morphine and heroin became the betes noires they are today, people learned about addiction the hard way. For example, William Stewart Halsted. the pioneering Johns Hopkins surgeon, used morphine most of his adult life — his maintenance dose was said to be about 200 mg daily. Yet he was creative and productive (known as the “father of American surgery”) over a very long career, because morphine was not illegal then. Note that these substances are well-tolerated by the body, too: It is opiods’ legal status and the black market this has created which makes these drugs so dangerous today.
That’s awesome! I’m sure mice everywhere are rejoicing at the prospect of finally finding relief from chronic pain of spinal injuries! Mouse traps be damned!
I wholeheartedly agree 👍 with you Richie. I noted the article states opiates are addictive yet fails to admit they are like these methods they are promoting & what they are given to these mice. Mind you with relief lasting a whole 2.5 months.I wonder do they cause massive pain for the week after getting the shot like the current steroid shots do? IMO The current & new methods then only kind of work for a few weeks. 😒 🤔 What was the upside to the new method again
There is always someone in a comments section trying to promote addictive and recreational drugs, pretending the only negative is that they are illegal. They either have no objectivity, or they were not alive in the 1980s when people were dying in enormous numbers. Take any graduating class back then, and 2, 3 or more are now missing because of drugs. Either they committed suicide because they lost control over their lives, destroyed their lives and saw no hope of ever repairing it, or simply made a mistake and overdosed.
Fentanyl people who got prescriptions, still were dying by the thousands just a few years ago. Legalized? The carnage would be 100,000+ a year in the US just from one drug. The current level of overdoses is 100,306 drug overdose deaths in the United States during 12-month period ending in April 2021. Could be a million a year if they removed all the protective laws. There are plenty of medications that are dangerous at the wrong dose, or in combination with others. People will be guessing at what they need and how much, accidentally killing themselves, their children their elderly parents… Just an utter disaster.
I’m interested in this news as I cannot tolerate any opioids at all & suffer chronic pain past 13yrs just taking osteopana plus Lyrica. Ive just seen a new pain specialist who put me on LDN, its working ! Im so happy & can almost walk without a cane now. He may do PFRN which is not painful but I may not need it.
This sounds promising, SCI patients neuralgia is well documented. Their already hampered life due to the injury can be doubly frustrating due to this nerve pain . When do the human trials start ? Are they expanding it to actual repairing the SCI , using gene therapy ?
I had a cervical spine issue for 14 years. Herniated disks at c4/5 and 5/6 that impinge on a nerve. I’ve had 18 epidural steriod shots(with no weeks of pain after) and 144 trigger point shots. My pain management Dr is happy to prescribe oxycodone (3 per day for 21 days) along with my shots which I can get every 3 months. First off opiods ARE highly addictive. I take half a pill twice a day if necessary. They prescribed 3 per day! 3 a day would send me to oblivion. The opiod problem in America is the worse drug problem this country has ever seen. I’m extremely hopeful to possibly be pain free for 2.5 months. That would be amazing. The epidurals do releive some pain(with some soft tissue deteriation). My next options is stem cell injections in Panama at Tony Robbins place. My options after that is spinal fusion. NO THANKS. Fingers crossed on any future devopements as far as pain relief for nerve pain. 😊
I have been waiting over 20 years for something like this research to happen and to work. I can only hope your research continues to work.
I have been on extended release morphine and other prescriptions for many many years since being diagnosed with Spinal Adhesive Arachnoiditis caused by my back surgeon during a laminectomy in the 90’s. Of course the surgeon never admitted this and I have been paying for his mistakes with chronic pain and other problems since, diagnosed by many other physicians. So I applaud all the work you are doing in gene therapy to help patients like me. To give us some relief from chronic pain so we don’t have to be shamed for NEEDING and taking narcotics for pain. Maybe one day we won’t have to search from town to town and state to state for doctors and pharmacies who will prescribe and fill our needed prescription narcotics for chronic pain. It is not fun to have to jump through all the hoops of the DEA, FDA, CDC, etc. just to have the right to be pain free. Thank you for all the work you do.