
Researchers at WEHI have solved a century-old question in diabetes research by discovering that a molecule other than insulin can have the same effect. This provides valuable information for the future creation of an oral insulin pill.
Researchers at the Walter and Eliza Hall Institute (WEHI) in Melbourne have finally answered a question that has puzzled diabetes researchers for a century: can a molecule other than insulin have the same effect? The team’s findings provide crucial insight into the development of an oral insulin pill.
They have successfully demonstrated how a non-insulin molecule can imitate insulin, which is essential for maintaining blood sugar levels.
The WEHI-led study opens new avenues for the development of drugs that could replace daily insulin injections for people with type 1 diabetes.

At a Glance
- Researchers have visualized precisely how an insulin-mimicking molecule reproduces the activity of insulin to regulate blood glucose levels
- The study answers a century-old question of whether it is possible to replace insulin
- Findings illuminate new opportunities for the development of oral insulin mimetics that may replace daily injections by type 1 diabetics
- People with type 1 diabetes cannot produce insulin and require multiple daily insulin injections to keep their blood glucose levels in check.
The new research confirms that alternative molecules can be used to turn on blood glucose uptake, bypassing the need for insulin altogether.
The study, published in Nature Communications, was led by WEHI’s Dr. Nicholas Kirk and Professor Mike Lawrence, in collaboration with researchers from Lilly, an American-based pharmaceutical company.
Why Is There No Insulin Pill?
Dr. Kirk said scientists have struggled to make insulin as a pill because insulin is unstable and readily degraded by the body upon digestion.
“Since the discovery of insulin 100 years ago, the development of an insulin pill has been a dream for diabetes researchers but, after decades of trying, there has been little success,” he said.
The research has now accelerated dramatically with the development of cryo-electron microscopy (cryo-EM), a new technology that can visualize complicated molecules in atomic detail, allowing researchers to generate 3D images (“blueprints”) of the insulin receptor rapidly.
“With cryo-EM, we can now directly compare how different molecules, including insulin, change the shape of the insulin receptor,” said Dr. Kirk.
“Insulin’s interaction turns out to be far more complex than anyone predicted, with both insulin and its receptor changing shape dramatically as they partner up.”
Mimicking Insulin With Simple Molecules
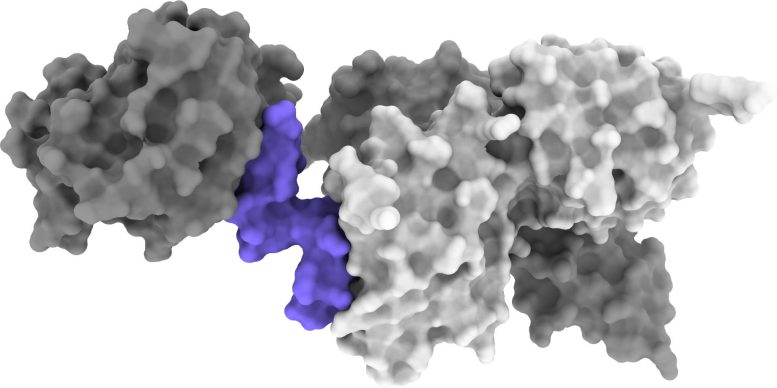
The new research shows how an insulin-mimicking molecule acts on the insulin receptor and turns it on, the first step in a pathway that directs cells to soak up glucose when the body’s sugar levels are too high.
The team performed intricate cryo-EM reconstructions to obtain blueprints of several molecules called “peptides” that are known to interact with the insulin receptor and hold it in the “active” position.
The cryo-EM experiments identified that one peptide that can bind to and activate the receptor in a manner similar to insulin.
“Insulin has evolved to hold the receptor carefully, like a hand bringing a pair of tongs together,” Dr. Kirk said.
“The peptides we used work in pairs to activate the insulin receptor – like two hands grabbing the pair of tongs around the outside.”
While therapeutic outcomes are distant, the team’s discovery could lead to a drug to replace insulin, reducing the need for injections by diabetics.
“Scientists have had success replacing these kinds of mimetic molecules with drugs that can be taken as pills,” Dr. Kirk said.
“It’s still a long road that will require further research, but it’s exciting to know that our discovery opens the door for oral treatments for type 1 diabetes.”
Reference: “Activation of the human insulin receptor by non-insulin-related peptides” by Nicholas S. Kirk, Qi Chen, Yingzhe Ginger Wu, Anastasia L. Asante, Haitao Hu, Juan F. Espinosa, Francisco Martínez-Olid, Mai B. Margetts, Faiz A. Mohammed, Vladislav V. Kiselyov, David G. Barrett and Michael C. Lawrence, 28 September 2022, Nature Communications.
DOI: 10.1038/s41467-022-33315-8
The research was funded by Lilly.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.