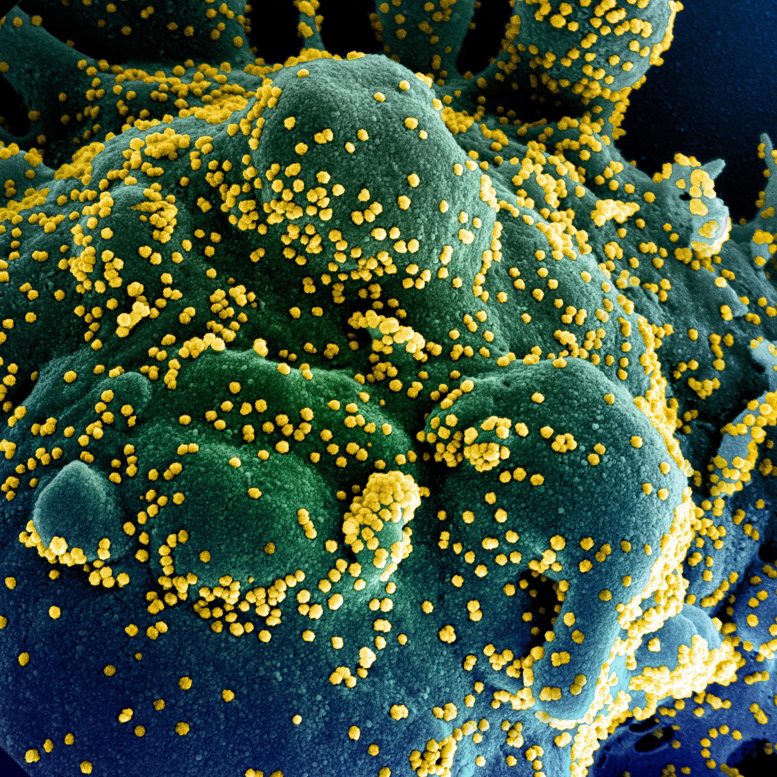
When the novel coronavirus (SARS-CoV-2) infects a human cell, it hijacks cellular machinery to produce millions of new copies of itself. Credit: NIAID
The National Institutes of Health has launched an adaptive Phase 3 clinical trial to evaluate the safety and efficacy of three immune modulator drugs in hospitalized adults with COVID-19. Some COVID-19 patients experience an immune response in which the immune system unleashes excessive amounts of proteins that trigger inflammation — called a “cytokine storm” — that can lead to acute respiratory distress syndrome, multiple organ failure and other life-threatening complications. The clinical trial aims to determine if modulating that immune response can reduce the need for ventilators and shorten hospital stays. The trial, known as ACTIV-1 Immune Modulators (IM), will determine if the therapeutics are able to restore balance to an overactive immune system.
Part of the Accelerating COVID-19 Therapeutic Interventions and Vaccines (ACTIV) initiative, the trial expects to enroll approximately 2,160 hospitalized adults with moderate to severe COVID-19 at medical facilities in the United States and Latin America. The National Center for Advancing Translational Sciences (NCATS), part of NIH, will coordinate and oversee the trial with funding support from the Biomedical Advanced Research and Development Authority (BARDA) of the U.S. Department of Health and Human Services Office of the Assistant Secretary for Preparedness and Response, in support of the Trump administration’s Operation Warp Speed goals. BARDA’s Clinical Studies Network will be responsible for operationalizing the trial through a task order awarded to contract research organization Technical Resources International, Inc.
“This is the fifth master protocol to be launched under the ACTIV partnership in an unprecedented timeframe, and focuses efforts on therapies that hold the greatest promise for treating COVID-19,” said NIH Director Francis S. Collins, M.D., Ph.D. “Immune modulators provide another treatment modality in the ACTIV therapeutic toolkit to help manage the complex, multi-system conditions that can be caused by this very serious disease.”
ACTIV-1 IM is a randomized, placebo-controlled trial that uses an adaptive master protocol. One of the hallmarks of master protocols is that they allow coordinated and efficient evaluation of multiple investigational agents as they become available. This enables maximum flexibility to swiftly weed out drugs that do not demonstrate effectiveness, identify those that do in a short time frame, and rapidly incorporate additional experimental agents into the trial.
The ACTIV public-private partnership selected three agents for the study from a pool of over 130 immune modulators initially reviewed based on several factors, including their relevance to COVID-19, strong evidence for use against inflammatory reaction and cytokine storm, and availability for large-scale clinical studies. The initial agents are infliximab (REMICADE), developed by Janssen Research & Development, LLC., one of the Janssen Pharmaceutical Companies of Johnson & Johnson; abatacept (ORENCIA), developed by Bristol Myers Squibb; and Cenicriviroc (CVC), an investigational late-stage agent developed by AbbVie.
All participants in the trial will receive remdesivir, which is the current standard of care treatment of hospitalized patients with COVID-19. Convalescent plasma and dexamethasone will be allowed at the discretion of the site investigator and in accordance with national guidelines. They will be randomly assigned to receive a placebo or one of the immune modulators as an add-on treatment. The trial will study the different combination treatment regimens with respect to illness severity, recovery speed, mortality and hospital resource utilization.
Enrollment is now open, and the trial is expected to last approximately six months. Results will be available shortly after the trial is completed, or possibly sooner if analysis conducted during the trial indicates that one or more of the drugs is beneficial. To ensure that the trial is being conducted in a safe and effective manner, an independent data and safety monitoring board will oversee the trial and conduct periodic reviews of the accumulating data.
The protocol team chair is William G. Powderly, M.D., director of the Institute for Clinical and Translational Sciences and co-director of the Division of Infectious Diseases at Washington University School of Medicine in St. Louis. NCATS’ Clinical and Translational Science Awards (CTSA) Program and the Trial Innovation Network will play a key role in adding U.S. study sites and enrolling patients, including those from communities disproportionately affected by COVID-19.
“The CTSA Program’s nimbleness and innovation in conducting clinical trials–along with the network’s extensive capacity and broad geographical reach–have positioned it to rapidly implement this important trial,” said NCATS Director Christopher P. Austin, M.D. “The innovative trial design will allow efficient evaluation of three different potential COVID-19 treatments concurrently, delivering new possible treatments for patients more quickly and valuable insights into the science of clinical translation.”





Be the first to comment on "National Institutes of Health Launches Large Clinical Trial to Test Immune Modulators for Treatment of COVID-19"