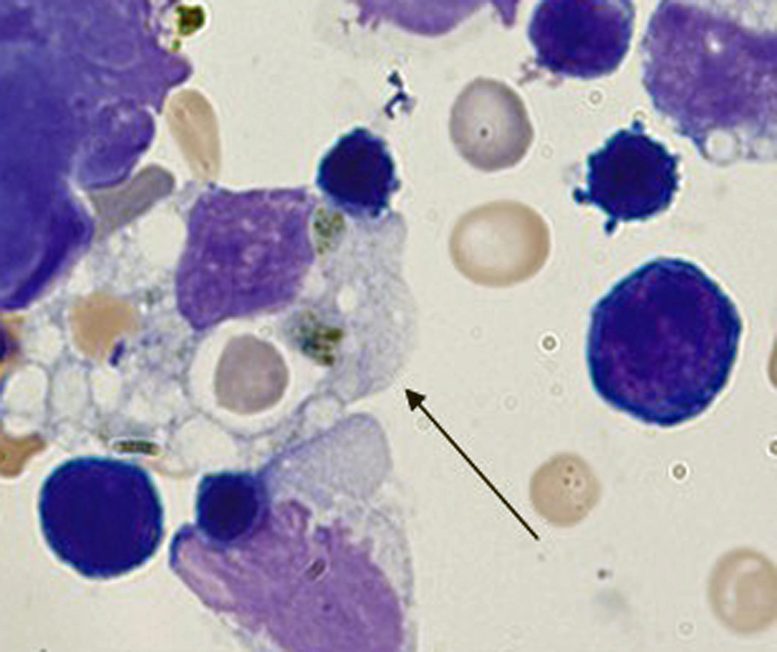
How mice that model immune disease’s cytokine storms may point to solution for global pandemic.
A transgenic mouse developed at Cincinnati Children’s to model the deadly childhood immune disease HLH (hemophagocytic lymphohistiocytosis) may play a key role in saving lives during the COVID-19 virus pandemic.
One of the genetically engineered mouse strain’s inventors–Cincinnati Children’s cancer pathologist Gang Huang, Ph.D.– is co-investigator on a small clinical trial that successfully tested a drug used to treat HLH (ruxolitinib) to dramatically reverse respiratory and multi-system inflammation in severely ill COVID-19 patients. Data from the Phase II clinical study is published in the Journal of Allergy and Clinical Immunology.
The study involved 43 hospitalized patients diagnosed with severe COVID-19 between February 9 and February 28 in Wuhan, China, believed to be ground zero for the pandemic. The multi-center study was led by Jianfeng Zhou, MD, Ph.D., Department of Hematology at Tongji Hospital, Tongji Medical College, and Huazhong University of Science in Wuhan.
Zhou is a longtime collaborator of Huang and colleagues at the Cincinnati Children’s HLH Center of Excellence, part of the Cancer and Blood Diseases Institute.
Ruxolitinib Shows Signs of Benefit
Patients taking ruxolitinib were randomly selected to receive two daily 5mg oral doses of the anti-inflammatory drug, plus the standard of care treatment for COVID-19. A randomly selected control group of 21 patients received a placebo along with the standard of care treatment.
“Ruxolitinib recipients had a numerically faster clinical improvement,” study authors write in their report. “Significant chest CT improvement, a faster recovery from lymphopenia and favorable side-effect profile in ruxolitinib group were encouraging and informative to future trials to test the efficacy of ruxolitinib in a larger population.”
Patients treated with ruxolitinib saw a shorter median time to clinical improvement compared to the control group. Patients treated with ruxolitinib saw a shorter median time to clinical improvement compared to the control group. Researchers reported that 90 percent of ruxolitinib patients showed CT scan improvement within 14 days, compared with 61. 9 percent of patients from the control group. Three patients in the control group eventually died of respiratory failure. All the severely ill patients who received ruxolitinib survived.
More clinical testing of the drug is needed. A larger Phase III clinical trial RUXCOVID by Incyte and Novartis is now testing up to 400 severely ill COVID-19 patients with the drug, according to Huang. Preliminary clinical data from the study is expected during the summer, he added.
“This is the first therapy we know of that appears to work effectively to quiet the cytokine storm and inflammation in severe COVID-19 disease, and there are no significant toxicities to patients who take the drug by two pills a day,” Huang said. “This is critical until we can develop and distribute enough effective vaccines to help prevent people from becoming infected.”
Calming the ‘Cytokine Storm’
The so-called cytokine storm that inundates the bodies of severely ill COVID-19 patients with inflammatory cells produced by the immune system is a common feature of children battling secondary HLH, which happens in patients where initial HLH treatment has not worked. Huang, who along with a large portion of the world’s scientific community was busy trying to study and find solutions to COVID-19, noticed this common clinical feature of both illnesses.
He also noticed that severe COVID-19 disease clinical manifestations are very similar to those seen in transgenic laboratory mice created to faithfully mimic human secondary HLH in the lab. That preclinical laboratory research, some of it in collaboration with the researchers in Wuhan, China, helped identify the drug ruxolitinib for treating secondary HLH. The anti-inflammatory drug is also used to treat other blood diseases including leukemia.
“I approached our research colleagues in Wuhan and explained our observations and recommended this drug be tested to quiet the cytokine storm in the multi-system inflammation in patients with severe COVID-19 disease,” Huang said. “The disease was spreading very rapidly and many people were dying. We believed the existing clinical drug would help save lives. So, we worked to push it forward before there is an effective vaccine for everyone.”
Huang said the work with colleagues in China was completed on a compressed timeframe as scientists around the world went on high alert to battle the pandemic in January. During their work, Huang and researchers in China found other clinical studies involving other diseases where ruxolitinib also had worked well at quieting inflammation, and testing on COVID-19 patients proceeded.
Reference: “Ruxolitinib in treatment of severe coronavirus disease 2019 (COVID-19): A multicenter, single-blind, randomized controlled trial” by Yang Cao, M.D., Ph.D., Jia Wei, M.D., Ph.D., Liang Zou, M.D, Tiebin Jiang, M.D, Gaoxiang Wang, M.D, Ph.D., Liting Chen, Ph.D., Liang Huang, M.D, Ph.D., FankaiMeng, M.D., Ph.D., Lifang Huang, M.D., Ph.D., Na Wang, M.D., Ph.D., Xiaoxi Zhou, M.D., Ph.D., Hui Luo, M.D., Ph.D., Zekai Mao, M.D., Ph.D., Xing Chen, M.D., Ph.D., Jungang Xie, M.D., Ph.D., Jing Liu, M.D., Ph.D., Hui Cheng, M.D, Jianping Zhao, M.D., Ph.D., Gang Huang, Ph.D., Wei Wang, M.D., Ph.D., Jianfeng Zhou, M.D., Ph.D., 19 May 2020 (accepted), Journal of Allergy and Clinical Immunology.
DOI: 10.1016/j.jaci.2020.05.019
Funding support for the JACI study came as part of an Emergency Research Project of Tongji Hospital, Huazhong University of Science and Technology (2020kfyXGYJ045), an Emergency Research Project of Hubei province (2020FCA006).
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
4 Comments
Seems to me we’re attacking this problem from the wrong end. A probiotic diet with plenty of plant fiber and supplements to get plenty of fat-soluble vitamins A, D3, E, and K2; minerals calcium, magnesium, zinc, and selenium, combined with intermittent fasting involving an eating period of at most 8 hours per day should strengthen the immune system, minimizing the probability that the cytokine storm is triggered in the first place.
What Triggers A Cytokine Storm . . . Predisposed VULNERABILITY
TBI – Traumatic Brain Injury
Immune System Compromise/ Deficiency.
ASIA – Autoimmune Inflammatory Syndrome Induced By Adjuvants.
Adjuvants Used Extensively In The Manufacturing Process Of Multiple Childhood Vaccines.
Live Virus Vaccines Are Contraindicated For Use In The Immunocompromised/ Immunodeficient Recipient.
“SCREENINGB4VACCINES” For
“CONTRAINDICATION” Needs To Become A Global Health Priority.
AUTISM – Acumulative Viral Toxic Effects Of Multiple Live Virus Vaccine Plus Adjuvants In Early Infancy Of An Innately Immunocompromised Infant Child.
AUTISM / FRAGILE X / CANCER DEVELOPMENT.
Parent Of A Birth Injured And Subsequently Severely Vaccine Injured Son Who Developed Devestating Regressive Autism / Cancer Following Multiple Live Virus Vaccine Plus Adjuvants In Early Infancy . Who Went On To Develop ASIA.
MIBE.
SSPE POST MMR LIVE VIRUS VACCINE.
AUTISM / CANCER
A Viral Infection Preceeds Cancer Development.
add water-soluble vitamins C and B-complex.
Leronlimab
https://www.thepharmaletter.com/article/researchers-begin-testing-cytodyn-s-leronlimab-antibody-in-covid-19