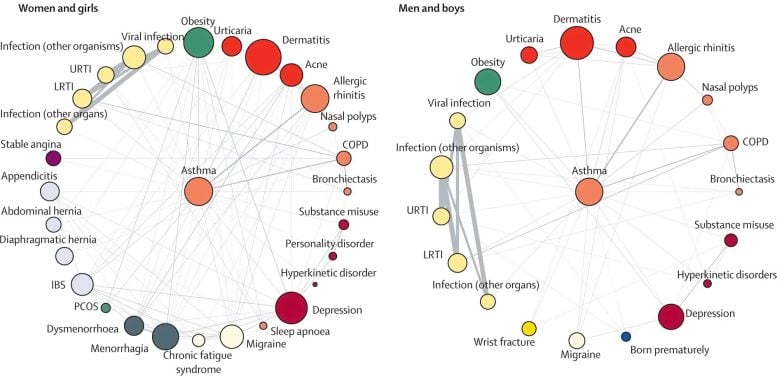
A new study led by University College London (UCL) researchers has identified patterns in how common health conditions occur together in the same individuals, using data from four million patients in England.
With advancing age, millions of people live with multiple conditions — sometimes referred to as multimorbidity. Furthermore, the proportion of people affected in this way is expected to rise over the next decades. However, medical education and training, clinical guidelines, healthcare delivery, and research have evolved to focus on one disease at a time.
This problem is recognized by the Academy of Medical Sciences and the UK Chief Medical Officer (CMO), which have set out a challenge of investigating which diseases co-occur in the same individuals and why.
In the new study, which was recently published in the journal Lancet Digital Health, the team used routine health records data to systematically identify patterns of clustering of 308 common mental and physical health conditions of men and women of different ages and with different ethnicities.
Patterns of Disease Co-Occurrence
Some patterns found include: heart failure often co-occurred with hypertension, atrial fibrillation, osteoarthritis, stable angina, myocardial infarction, chronic kidney disease, type 2 diabetes, and chronic obstructive pulmonary disease.
Hypertension was most strongly associated with kidney disorders in those aged 20–29 years, but with dyslipidaemia, obesity, and type 2 diabetes in individuals aged 40 years and older.
Breast cancer was associated with different comorbidities in individuals from different ethnicities, asthma with different comorbidities between the sexes, and bipolar disorder with different comorbidities in younger ages compared with older ages.
The findings, the researchers say, provide the data and resources to help improve health and care planning for patients in England living with more than one condition.
Inclusive Insights from Diverse Health Records
Co-author Professor Aroon Hingorani (UCL Institute of Cardiovascular Science) said: “Information from minority ethnic groups and younger people has often been missing from studies of multimorbidity, but by using diverse electronic health records, we present a more inclusive and representative perspective of multimorbidity. This is one area where the NHS electronic health records and data science can generate important insights.”
Professor Spiros Denaxas (UCL Institute of Health Informatics) said: “Millions of people live with multiple diseases, yet our understanding of how and when these transpire is limited. This research project is the first step towards understanding how these diseases co-occur and identifying how to best treat them.”
The study includes accessible tools to help users visualize patterns of disease co-occurrence, including for diseases that cluster more commonly than expected by chance, providing an entry point to investigate common risk factors and treatments.
The findings should help patients better understand their illness, doctors better plan the management of patients with multimorbidity, healthcare providers optimize service delivery, policymakers plan resource allocation, and researchers to develop new or use existing medicines to treat several diseases together.
The data analyzed were from the Clinical Practice Research Datalink under license and managed securely via the UCL Data Safe Haven. All algorithms for defining the diseases are open source (and can be found here).
Reference: “Identifying and visualising multimorbidity and comorbidity patterns in patients in the English National Health Service: a population-based study” by Valerie Kuan, PhD; Prof Spiros Denaxas, PhD; Prof Praveetha Patalay, PhD; Prof Dorothea Nitsch, MD; Prof Rohini Mathur, PhD; Arturo Gonzalez-Izquierdo, PhD; Prof Reecha Sofat, PhD; Prof Linda Partridge, PhD; Amanda Roberts, BSc; Prof Ian C K Wong, PhD; Melanie Hingorani, FRCOphth; Prof Nishi Chaturvedi, MD; Prof Harry Hemingway, FMedSci and Prof Aroon D Hingorani, PhD on behalf of the Multimorbidity Mechanism and Therapeutic Research Collaborative (MMTRC), 29 November 2022, Lancet Digital Health.
DOI: 10.1016/S2589-7500(22)00187-X
The research was enabled by UK Research and Innovation’s Strategic Priority Fund, NIHR UCLH Biomedical Research Centre, Health Data Research (HDR) UK, Medical Research Council, the Department of Health and Social Care, Wellcome Trust, the British Heart Foundation, and The Alan Turing Institute, in collaboration with the Engineering and Physical Sciences Research Council.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
Asthma is not the centre of spectrum