Researchers at Nagoya University and their colleagues in Japan have discovered that obesity in middle age is due to age-related alterations in the form of neurons in the hypothalamus, the brain region responsible for regulating metabolism and appetite.
A protein called melanocortin-4 receptor (MC4R) detects overnutrition and regulates metabolism and appetite to prevent obesity. According to their study in rats, MC4Rs were concentrated in primary cilia (antenna-like structures) that extend from a couple of groups of hypothalamic neurons. The study also showed that the primary cilia became shorter with age, which decreased MC4Rs accordingly, resulting in weight gain.
“We believe that a similar mechanism exists in humans as well,” said Professor Kazuhiro Nakamura of the Nagoya University Graduate School of Medicine, the lead author of the study. “We hope our finding will lead to a fundamental treatment for obesity.” The researchers published the results of the study in the journal Cell Metabolism.
The Mechanism Behind Weight Gain
As we get older, we become more prone to being overweight and obesity. Obese people are more susceptible to diabetes, hyperlipidemia, and other chronic diseases. Previous studies have suggested that middle-aged weight gain is caused by a decline in overall metabolism due to aging, but the mechanism was unclear.
A research team of the Nagoya University Graduate School of Medicine, in collaboration with researchers from Osaka University, the University of Tokyo, and the Nagoya University Research Institute of Environmental Medicine, conducted a study focusing on MC4Rs.
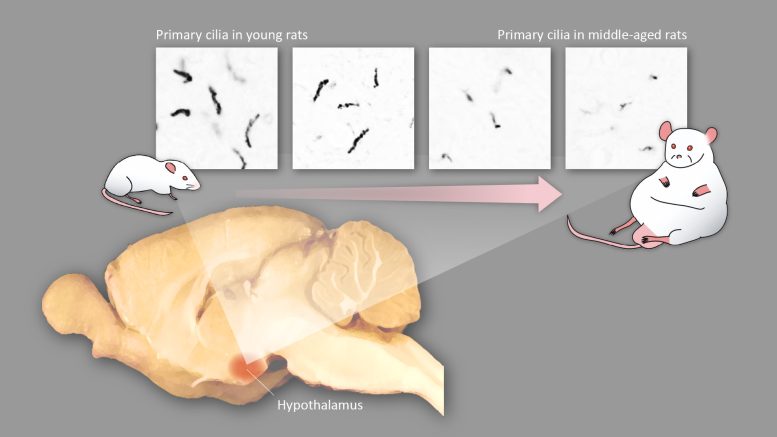
MC4Rs stimulate metabolism and suppress food intake in response to an overeating signal from melanocortin. Initially, the research team examined the distribution of MC4Rs in the rat brain by utilizing an antibody they had developed specifically to make MC4Rs visible. They found that MC4Rs are present exclusively in primary cilia of specific groups of hypothalamic neurons.
The team next investigated the length of the primary cilia that had MC4Rs (MC4R+ cilia) in the brains of 9-week-old (young) rats and 6-month-old (middle-aged) rats. The team found that MC4R+ cilia in middle-aged rats were significantly shorter than those in young rats. Accordingly, the metabolism and the fat-burning capacity of middle-aged rats were much lower than those of young rats.
Dietary Impact and Leptin Resistance
The team next analyzed MC4R+ cilia in rats under different dietary conditions. The results showed that MC4R+ cilia in rats on a normal diet gradually shortened with age. On the other hand, MC4R+ cilia in rats on a high-fat diet shortened at a faster pace, while those in rats on a restricted diet shortened at a slower pace.
Interestingly, the team also found that MC4R+ cilia that once disappeared with age were regenerated in rats raised under two months of dietary restriction.
In the study, the team also used genetic technologies to make MC4R+ cilia shorter in young rats. These rats showed increased food intake and decreased metabolism, leading to weight gain.
The team also administered a hormone called leptin to the brains of rats with artificially shortened MC4R+ cilia. Leptin is thought to help reduce food intake. Surprisingly, however, their appetite was not reduced, indicating that leptin could not exert anti-obesity effects.
“This phenomenon, called leptin resistance, is often observed in obese human patients as well. This is an obstacle to the treatment of obesity, but the cause has long been unknown,” explained Dr. Manami Oya, the first author of the study.
“In obese patients, adipose tissue secretes excessive leptin, which triggers the chronic action of melanocortin. Our study suggests that this may promote the age-related shortening of MC4R+ cilia and put animals into a downward spiral where melanocortin becomes ineffective, increasing the risk of obesity.”
The study concluded that the age-related shortening of MC4R+ cilia causes middle-age obesity and leptin resistance in rats. The researchers demonstrated that dietary restriction is one method to prevent and treat overweight and obesity. Prof. Nakamura said, “Moderate eating habits could maintain MC4R+ cilia long enough to keep the brain’s anti-obesity system in good shape even as we age.”
Reference: “Age-related ciliopathy: Obesogenic shortening of melanocortin-4 receptor-bearing neuronal primary cilia” by Manami Oya, Yoshiki Miyasaka, Yoshiko Nakamura, Miyako Tanaka, Takayoshi Suganami, Tomoji Mashimo and Kazuhiro Nakamura, 6 March 2024, Cell Metabolism.
DOI: 10.1016/j.cmet.2024.02.010
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
3 Comments
I think their research is phenomenal! I’m eager to see what else they discover within obesity.
Nothing is surprising in this article. We already know WHY obesity occurs, what this article explains is the body’s mechanism of how it happens. Obesity is a result of higher fat and food intake, and less physical activity. The article even states that. To prevent obesity, Prof. Nakamura said, “Moderate eating habits could maintain MC4R+ cilia long enough to keep the brain’s anti-obesity system in good shape even as we age.”
As we age, especially if our physical activity slows for one reason or another, it’s foolish to think we can continue to eat the same as we did as a growing teenager or as a physically active young adult. Couple that with how many children and young people are already overweight or even obese, the onus falls on the parents or the person thmself to change their eating habits.
Obesity can be due to a screwed up metabolism. If that isn’t corrected, it doesn’t matter if you eat consistently under the level of starvation. I know this because I live with this. Luckily, my internist and I have found a medication that will help solve this problem and I am finally losing weight. Telling people that all they need to do is “eat less and you will lose weight” could lead to death. If I am not eating above starvation level for my body my blood pressure sky rockets and cannot be controlled by any medication.