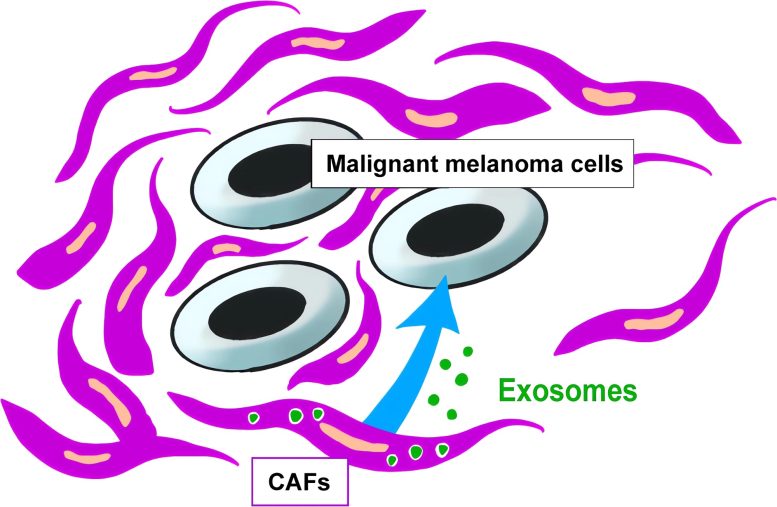
Researchers found that CD9-positive exosomes from CAFs may inhibit melanoma growth, offering a new marker for prognosis.
Malignant melanoma is a relatively aggressive type of skin cancer. When detected early, it is usually treatable by surgical resection only, but metastases develop often spreading to distant areas. Currently, tumor thickness and the presence of ulceration are some of the known prognostic factors used as indicators of malignant melanoma. Therefore, the discovery of valuable markers to assess the malignant potential of melanoma more accurately may be necessary to develop appropriate treatments.
Cross-talk between cancer cells and surrounding stromal cells is believed to orchestrate cancer progression through a variety of mechanisms. Cancer-associated fibroblasts (CAFs)—key factors in the tumor microenvironment—in particular have been implicated in cancer cell progression. It has also been reported that the exosomes, a type of small vesicles, produced by CAFs play an important role in cancer progression.
CD9-Positive Exosomes and Melanoma Growth
A research group led by Naho Fujii, M.D., and Professor Hisashi Motomura from Osaka Metropolitan University Graduate School of Medicine investigated the effect of CAF-derived exosomes on the growth of malignant melanoma cells. The group found that the transmembrane proteins CD9 and CD63 were mainly present on CAF-derived exosomes, and that among the exosomes, the CD9-positive ones inhibited the growth of malignant melanoma cells.
“As a plastic surgeon, usually I provide surgical treatment for skin cancer, but I have wanted to study other treatment methods for a long time,” explained Fujii, M.D. “This study suggests that CD9-positive exosomes inhibit the growth of malignant melanoma, so CD9-positive exosomes may be a useful marker to evaluate the malignant grade of melanoma. We expect further research will lead to the development of new treatments in that line.”
Reference: “CD9-positive Exosomes Derived from Cancer-associated Fibroblasts Might Inhibit the Proliferation of Malignant Melanoma Cells” by Naho Fujii, Masakazu Yashiro, Takaharu Hatano, Heishiro Fujikawa and Hisashi Motomura, 30 December 2022, Anticancer Research.
DOI: 10.21873/anticanres.16130
Basics of Malignant Melanoma and Risk Factors
Malignant melanoma is a type of skin cancer that develops from melanocytes, the pigment-producing cells in the skin. Melanocytes produce melanin, which is responsible for the color of our skin, hair, and eyes. When melanocytes become cancerous, they can form a malignant melanoma.
Malignant melanoma is the most aggressive and dangerous form of skin cancer, as it can spread rapidly to other parts of the body if not detected and treated early. While it accounts for a smaller percentage of skin cancer cases compared to other types, such as basal cell carcinoma and squamous cell carcinoma, it causes the majority of skin cancer-related deaths.
Risk factors for malignant melanoma include:
- Excessive sun exposure and ultraviolet (UV) radiation, including from tanning beds.
- A history of sunburns, especially during childhood or adolescence.
- Fair skin, light hair, and light eye color, as these individuals have less melanin to protect their skin from UV radiation.
- A family history of melanoma or a personal history of other skin cancers.
- A large number of moles or atypical moles (dysplastic nevi), which can be more likely to transform into melanoma.
Early detection is crucial for successful treatment of malignant melanoma. The American Academy of Dermatology recommends the “ABCDE” method to help identify potentially cancerous moles:
- Asymmetry: One half of the mole does not match the other half.
- Border: The edges are irregular, notched, or blurred.
- Color: The mole has varying colors or shades, such as black, brown, tan, white, or blue.
- Diameter: The mole is larger than 6 millimeters (about the size of a pencil eraser).
- Evolving: The mole is changing in size, shape, or color.
If you notice any of these signs, it’s important to consult a healthcare professional for evaluation and possible biopsy. Treatment options for malignant melanoma may include surgery, immunotherapy, targeted therapy, radiation therapy, or chemotherapy, depending on the stage and specific characteristics of the cancer.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.