You might have heard that COVID-19 vaccine trials are underway in Seattle. What exactly is being tested? How much longer will these tests take? And when can we expect a vaccine against the novel coronavirus? We chat with Benjamin Neuman, Ph.D., one of the world’s experts on coronavirus, and Daniel Wrapp, one of the scientists who mapped the structure of the protein that the coronavirus uses to infect your cells, to help us answer these questions:
Hi everyone.
So I am in week three of self quarantining. I’m here at home hanging out with this cute little potato, try and get some work done and going a little crazy.
So I read in the news that a vaccine targeting SARS-CoV-2 was already in phase one clinical trials, which sounded really good. So I did a bit of research.
I found out that on average it takes about 10 years to develop a vaccine to the point where it’s ready for the general public. So I would think we’re moving a heck of a lot faster than normal.
A big reason for this super fast pace is that we have a history of being infected by coronaviruses. Scientists came into this already knowing a lot about the structure and function of coronaviruses like SARS-CoV-2 in order to develop a vaccine.
It’s important for scientists to understand how a virus infects us.
To understand it myself, I reached out to Dr. Benjamin Neuman, who has been studying coronaviruses for decades.
And you were, just to clarify, you are part of the team that actually named the SARS-CoV-2 virus, right?
Not in charge of the team, but on the team.
Yeah, I joined back before it was cool. Yeah. I want my hipster creds.
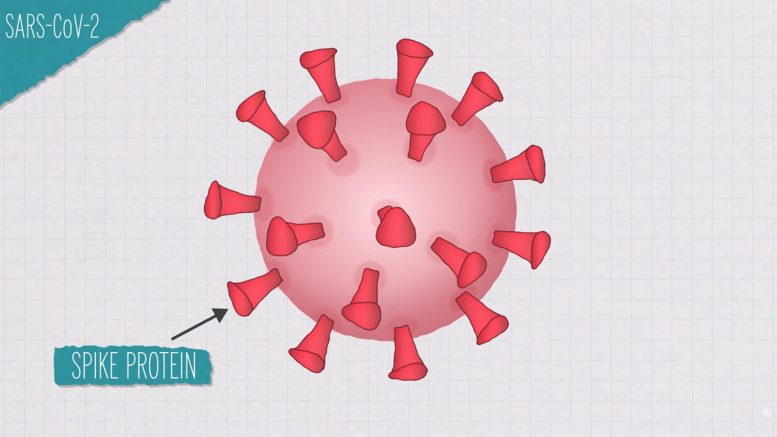
Uh, all right, so the SARS coronavirus has a protein on the outside called the spike protein.
The spike proteins stick off of the virus and search for cells to attach to.
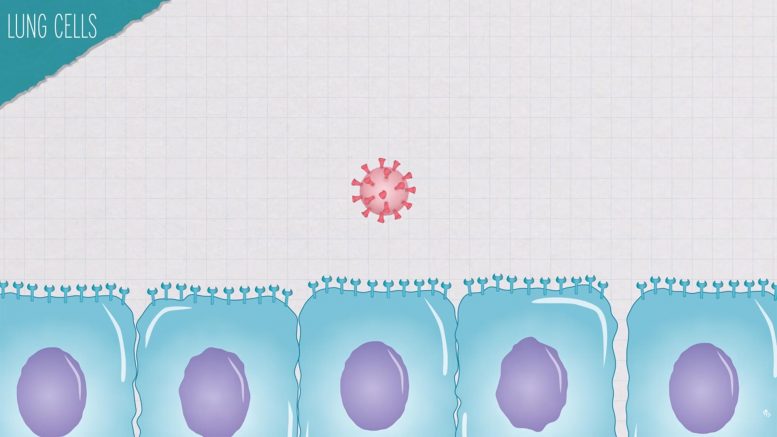
And that is going to bump into the ACE2 on the outside of a lung cell.
ACE2 is a receptor on some of your lung cells and that spike protein will bind to it in order for the virus to gain entry into your cells.
And then it’s basically going to make the cell think it’s time to eat. So the cell is going to pull in the receptor and the virus, I tell my students that basically it looks like fishing.
It throws out a little piece that looks like a hook that’s called a fusion peptide and the attaches to the cell and it’s already hooked into the virus and then it reels that in and just smacks the two together until the virus actually, yeah, has entered and deposited the genome and the cell. At that point, you’re infected.
Once the RNA is in your cells, you’re considered infected. Even if you don’t show any symptoms.
From there, what happens is the virus will replicate itself by hijacking things that your cell normally uses, like enzymes and organelles, and so it just makes more and more copies that will fill your cell until your cell explodes, releases those viruses and they go on to infect more cells.
Now that you have an idea of what being infected by SARS-CoV-2 actually means, let’s talk about a vaccine because that would actually stop the infection from ever happening. To develop a vaccine, you need to teach your immune system to recognize something unique about the virus so that then it can destroy it.
The spike protein might be that thing.
I actually spoke with Daniel Wrapp. He was the first author on the publication that came out in Science in mid February.
Yeah, the spike structure.
Yes.
Yes, I remember that name and that’s a heck of a paper and that was pretty amazing. Fast work. Yeah.
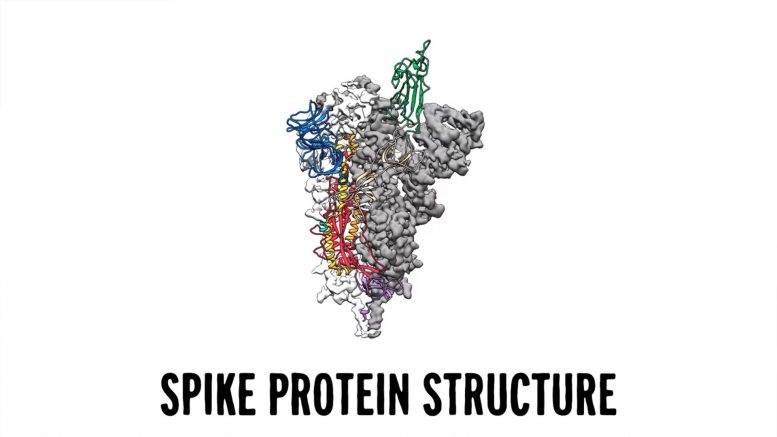
We used a technique called cryogenic electron microscopy or cryoEM. To look at individual spike proteins. So that we could determine the three dimensional structure.
Based on that 3D structure. Daniel and his team worked with a biotech company to create a vaccine.
The vaccine causes your body to make a bunch of that spike, so not the whole virus, just the spike. The idea is that if you’re ever exposed to SARS-CoV-2 your body will recognize the spike that’s on it and then go ahead and destroy the entire virus.
Okay, so do you want to know something else that is super interesting? The correct answer is yes. You definitely do.
Daniel and his team discovered something else about the spike.
SARS-CoV-2, which is the virus causing the COVID-19 pandemic right now is really similar in structure to the original SARS-CoV, the one that caused the SARS epidemic in 2002, 2003.
But there are already over 100 times more cases of COVID-19 than there were SARS cases back in the day. Why is that?
Daniel and his team have an idea of what could be going on here.
What we did was we used a technique called surface plasmon resonance or SPR to measure the binding affinity between ACE2 and spike. Um, and based on our calculations, we’re estimating it’s about 10 fold higher binding affinity between the receptor and this spike compared to SARS.
So this new version of the virus has a tenfold higher binding affinity, so you are more likely to be infected by it, but you’re also more likely to pass it on to other people.
So thanks to the knowledge that researchers already had about coronaviruses going into this pandemic and the collaborative efforts of scientists like Daniel, things are moving at a faster pace than normal.
And that means yes, we do have a vaccine that’s already in phase one clinical trials, but before we get ahead of ourselves, Daniel still predicts it’ll take about 14 months for a vaccine to be available to the public. That’s still really fast.
But remember, this is still phase one of the three phases of a clinical trial. And this vaccine could fail at any of those phases.
So while these trials are going on, Daniel has collaborators and other scientists around the world are still doing research to better understand that spike protein and to develop vaccines that might be even better.
In other words, they are not putting all their eggs in that one clinical trial basket.
So in the meantime, protect those who can’t self isolate and maybe just chill on your couch. Good girl Yuca, doing your part.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.