
A groundbreaking study suggests that IBS might be more of a brain issue than a gut disorder.
Researchers found that stress-induced IBS symptoms could be alleviated by drugs that regulate neurotransmitters in the brain. This could lead to treatments that not only ease IBS but also reduce stress and emotional distress.
Understanding IBS: A Widespread Yet Mysterious Condition
Irritable bowel syndrome (IBS) is a common digestive disorder that affects the intestines, causing symptoms like abdominal pain, bloating, gas, and irregular bowel movements, including diarrhea, constipation, or both. Despite affecting around 10% of the global population, the exact causes of IBS remain unclear. As a result, current treatments focus on managing symptoms rather than addressing the root cause.
Researchers at Tokyo University of Science (TUS) in Japan, led by Professor Akiyoshi Saitoh, have been investigating this issue for the past decade. Their latest study, published recently in the British Journal of Pharmacology, found that a class of drugs known as opioid delta-receptor (DOP) agonists may help relieve IBS symptoms. Unlike traditional treatments that act directly on the gut, these drugs work by targeting the central nervous system. The study was co-authored by Toshinori Yoshioka, a third-year PhD student at TUS.
The Link Between Stress and IBS
One of the main motivations for this study was the growing evidence linking IBS closely to psychological stress. Saitoh’s group aimed to address this potential root cause by focusing on finding a novel animal model for this condition.
In a study published in 2022, they developed a mice model repeatedly exposed to psychological stress—using a method called chronic vicarious social defeat stress (cVSDS)—which developed symptoms similar to a type of IBS called IBS-D.
These symptoms included overly active intestines and heightened sensitivity to abdominal pain, even though their organs showed no physical damage. The cVSDS animal model involved having the subject mouse repeatedly witness a territorial, aggressive mouse defeating a cage mate, inducing indirect chronic stress.
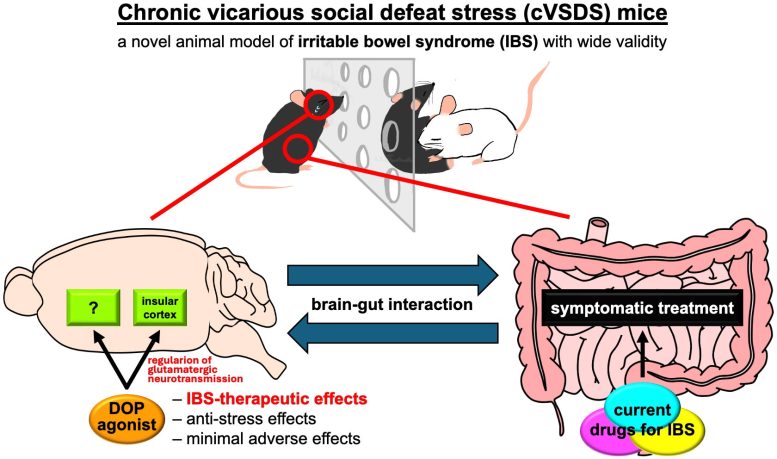
Exploring a Novel Stress-Based IBS Model
Using the cVSDS model, the researchers sought to determine whether DOP in the brain, which is closely linked to pain and mood regulation, could serve as promising drug targets for treating stress-induced IBS. To achieve this, they performed a series of detailed experiments to observe the effects of DOP agonists on IBS symptoms and chemical signaling in the brain.
Some experiments involved measuring the speed of a charcoal meal through the intestine to assess gastrointestinal motility and evaluate the impact of stress or treatments on bowel movement speed, along with directly measuring neurotransmitter concentrations using in vivo brain microdialysis. This revealed that re-exposure to VSDS increased glutamate levels in the insular cortex, but these elevated levels were normalized with DOP agonists.
DOP Agonists: A New Hope for IBS Treatment
According to the results, the administration of DOP agonists helped relieve abdominal pain and regulated bowel movements in cVSDS mice. Interestingly, applying the DOP agonists directly to a specific brain region called the insular cortex had similar effects on IBS symptoms as systemic treatment.
“Our findings demonstrated that DOP agonists acted directly on the central nervous system to improve diarrhea-predominant IBS symptoms in mice, and suggest that the mechanism of action involves the regulation of glutamate neurotransmission in the insular cortex,” highlights Saitoh.
Future Implications and Next Steps
Taken together, the continued research by Saitoh’s group on this topic could pave the way for effective treatments for IBS. “DOP agonists could represent a groundbreaking new IBS treatment that not only improves IBS-like symptoms but also provides anti-stress and emotional regulation effects. In the future, we would like to conduct clinical developments with the goal of expanding the indication of DOP agonists for IBS, in addition to depression,” remarks Saitoh.
Compared to currently available IBS treatments, such as laxatives, antidiarrheals, analgesics, and antispasmodics, targeting the underlying stress with DOP agonists may offer a more definitive solution with minimal adverse effects. Further clarification of the roles of stress and brain chemistry in the development of IBS will be essential in achieving this much-needed medical breakthrough. With promising prospects, future studies will translate Saitoh’s group’s findings to humans, bringing great relief to those affected by IBS.
Reference: “Agonists of the opioid δ-receptor improve irritable bowel syndrome-like symptoms via the central nervous system” by Toshinori Yoshioka, Sayaka Kimiki, Mayuna Yamazaki, Takumi Hamano, Mizuki Ou, Yumi Ode, Rui Ehara, Keita Kajino, Satoka Kasai, Kazumi Yoshizawa, Tsuyoshi Saitoh, Daisuke Yamada, Hiroshi Nagase and Akiyoshi Saitoh, 25 December 2024, British Journal of Pharmacology.
DOI: 10.1111/bph.17428
Professor Akiyoshi Saitoh, a distinguished researcher and professor at Tokyo University of Science’s Faculty of Pharmaceutical Sciences, is renowned for his expertise in medical and behavioral pharmacology, neuroscience, and anti-anxiety drug development. Holding a Ph.D. from Hoshi University, he has authored over 130 impactful publications in areas such as pharmacology, psychopharmacology, and neuropharmacology. With multiple patents to his name, Prof. Saitoh’s innovative contributions have left a lasting mark. His influential work, reflected in numerous citations, has established him as a key figure in advancing the pharmaceutical and neuroscience disciplines.
This work was supported by the Core Research for Evolutional Science and Technology as part of the Japan Agency for Medical Research and Development (AMED, grant number JP24gm1510008).
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
5 Comments
I wanted to respond to the IBS and brain connection. I believe many people that are diagnosed with IBS actually have(SIBO) small intestines bacterial overgrowth. I was diagnosed with it about a year ago. I have also been diagnosed with additional medical issues. However with that being said one of the most devastating things of having the sibo is that your brain isn’t getting any vitamins and nutrition that we need to function properly. I would love to be able to talk to someone that has more information on sibo. I have done three rounds of antibiotic treatments which has not worked for me. I just happened to notice this article. It says I can respond I don’t know even how many words I can put. I would love if somebody could respond back to me was possibly more information. Thank you.
Karen, you could search your question. “I’ve been diagnosed with sibo, now what?”, or how to recover from sibo. Or, physician near me to treat sibo or a nutritionist near you. If your doctor doesn’t know where to go from here, you could search for more help on your own. Hopefully someone with experience will answer here but, why wait? Best of luck to you!! Liz
Talk to your doctor about Anti parasite medication for your gut
Please try Manuka honey 1000 mgo
Whenever studies assume that only the neurons in the brain are important, and ignore the neuronal networks found in other parts of the body (like the abdomen and the heart) it makes me wonder who they are and why they’re not getting challenged more. Because they didn’t definitely find a brain connection – they saw a response in the intestinal system of mice to chemicals which affect the central nervous system, then say their findings “suggest that” it’s a brain cause in humans. Do mice also have an abdominal neuronal system? If not – why not suggest more research on the effects of the human abdominal neuronal system, instead of leaping to “it’s all in your brain” assumptions?
And – what about the definite connection which has been demonstrated between the gut microbiome and IBS? If it is a brain disorder, how does a poop transplant fix it?
At best, this is a very preliminary study which raises some interesting questions and points in several directions for more study. It doesn’t warrant the headline “Your IBS May Be a Brain Problem – And Researchers Have the Answer”. This study has no answers at all, just more questions.