Antibiotics cure many bacterial infections. However, some patients suffer a relapse. A research group at the University of Basel has now discovered why some bacteria can survive antibiotic therapy. The team uncovered where the bacteria hide in the body and how the body’s own immune system also plays an important role.
Infections such as tuberculosis or typhoid fever are caused by bacteria and can usually be treated well with antibiotics, at least as long as the bacteria are not resistant. However, full eradication of the bacteria cannot always be achieved. In some patients, a few bacteria survive the antibiotic therapy and can cause relapsing disease. For a long time, scientists have been trying to find out why antibiotics fail to kill all the bacteria.
Professor Dirk Bumann’s group at the Biozentrum, University of Basel, has now shown, that it is not – as may be expected – due to dormant and therefore insensitive pathogens. Rather, there are certain areas in the tissue in which typhoid fever-causing Salmonella can survive more or less unaffected by the body’s immune defenses. The researchers published their results in PNAS.
Examining Tissue Slice by Slice
“After antibiotic therapy, only about every 100th bacterium survives,” says Dirk Bumann, the study leader. “Tracking down and studying these few Salmonella in tissues is like looking for the needle in the haystack.”
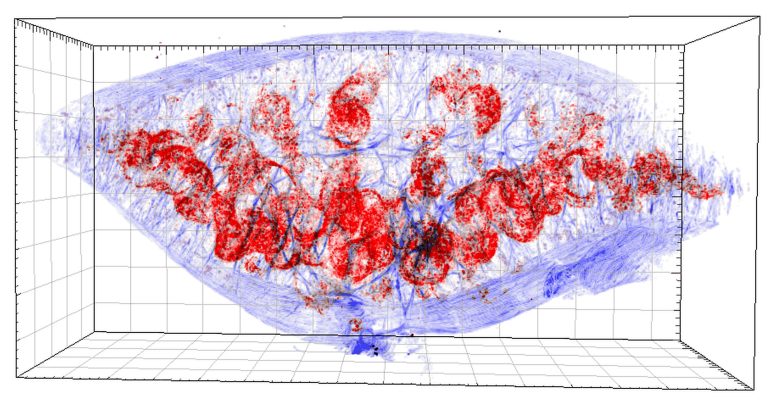
In order to manage this Sisyphean task, the researchers employed so-called serial two-photon tomography, a method used previously in neurobiology to detect the finest nerve fibers in the brain. The scanner device images the tissue surface and then cuts away the uppermost layer. The new surface is scanned again followed by the next cut. In this way the instrument works its way, slice by slice, through the whole tissue. This provides the scientists with a detailed three-dimensional view of the tissue and reveals where the few surviving bacteria are located.
Hidden in the Police Headquarters
In their study, the researchers imaged spleens of infected mice. Most Salmonella live in the so-called red pulp of the spleen, the recycling station for red blood cells. “Here, Salmonella is almost totally eliminated during antibiotic treatment,” explains Jiagui Li, one of the three first authors of the study. Some Salmonella live also in another spleen region, the white pulp, where immune responses are normally initiated. In this region, however, antibiotic therapy is rather ineffective. The white pulp thus becomes the major home of surviving Salmonella. “It’s ironic, that pathogens hide in the body exactly where they should be caught as the culprit and an effective defense against them should be activated,” says Bumann.
Antibiotics Alone Are Not Enough
How do the bacteria survive in this surprising location? The scientists found that antibiotics alone cannot eradicate Salmonella from the tissue but needs the help of the immune system to clear all bacteria. In particular neutrophils, white blood cells that effectively fight bacteria, are critical. For successful eradication of Salmonella, neutrophils have to work together with the antibiotic for several days. In the white pulp, however, there are only few neutrophils and their number collapses during treatment. With fading support from host neutrophils, the antibiotic alone cannot eradicate the local Salmonella.
To overcome this problem, the research team has tried boosting the body’s defenses with the help of a simultaneously applied immune therapy. “This approach can help to stimulate the immune system and to maintain a high density of neutrophils over a longer time,” explains Bumann. Indeed, such adjunct therapy may lead to more effective clearance of the bacteria opening new avenues to prevent relapses.
Reference: “Tissue compartmentalization enables Salmonella persistence during chemotherapy” by Jiagui Li, Beatrice Claudi, Joseph Fanous, Natalia Chicherova, Francesca Romana Cianfanelli, Robert A. A. Campbell, and Dirk Bumann, 15 December 2021, Proceedings of the National Academy of Sciences.
DOI: 10.1073/pnas.2113951118
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.