
Researchers from Osaka University discover an unexpected alteration in the brain during the autopsy of a patient with clinically typical Parkinson’s disease: an accumulation of TDP-43 proteins rather than alpha-synuclein.
Parkinson’s disease (PD) currently has no known cure, and one of the major challenges in creating effective treatments is that we are unsure of how or why the disease develops. Most experts agree that a buildup of Lewy bodies, which are cellular inclusions mostly made up of the brain-specific protein alpha-synuclein, causes cell death in important brain regions and results in the typical PD symptoms. But according to a new study by Osaka University researchers that was published in the journal Movement Disorders, this may not be the only way that PD-related cell death can take place.
A patient described in the paper exhibited what seemed to be standard PD and had neither a family history of the condition nor any gene alterations that may have contributed to it. He had classic PD motor symptoms such as stiffness, sluggishness, and balance issues. He also exhibited low dopamine (which helps cells communicate with one another) in the striatum of the brain and reacted well to treatment with the drug levodopa, both of which are frequent in patients with Parkinson’s disease.
The patient’s brain was carefully investigated after he passed away from pneumonia. The substantia nigra, a crucial PD-related brain area, showed increased inflammation and lost brain cells, among other common PD abnormalities, but some other typical PD-related changes were not seen. The researchers were unable to locate Lewy bodies harboring alpha-synuclein in any of the normally PD-affected areas.
Discovery of TDP-43 Protein Inclusions
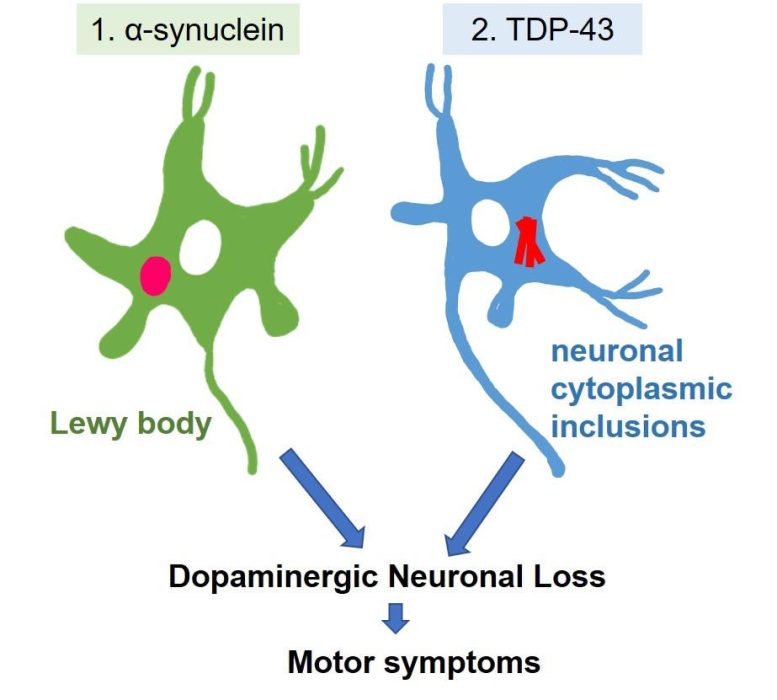
“This was unusual,” says the lead author of the study Rika Yamashita. “When we looked further, we realized that the patient had inclusions containing another type of protein: transactive response DNA-binding protein of 43 kDa, or TDP-43.”
Accumulation of TDP-43 protein occurs in other neurodegenerative diseases like amyotrophic lateral sclerosis and frontotemporal lobar degeneration, but it is not usually associated with PD. However, this new report suggests that its accumulation may cause cell loss in the substantia nigra as well as the typical motor symptoms of PD.
“This report has implications for how we think about the development of PD,” explains Goichi Beck, senior author of the report. “Much of the current research looking for PD treatments is very focused on alpha-synuclein—but it may not be the only protein that causes the disease. Our findings indicate that TDP-43 accumulation may be a cause of PD separate from alpha-synuclein accumulation.”
Future studies need to take TDP-43 into consideration when investigating the mechanisms causing PD in the brain. The findings from this research suggest a new pathway for developing PD and may lead to the discovery of new treatments that slow or cure the disease, which is currently lacking.
Reference: “TDP-43 Proteinopathy Presenting with Typical Symptoms of Parkinson’s Disease” by Rika Yamashita MD; Goichi Beck MD, Ph.D.; Yuki Yonenobu MD; Kimiko Inoue MD; Akihiko Mitsutake MD, Ph.D.; Hiroyuki Ishiura MD, Ph.D.; Masato Hasegawa Ph.D.; Shigeo Murayama MD, Ph.D. and Hideki Mochizuki MD, Ph.D., 9 May 2022, Movement Disorders.
DOI: 10.1002/mds.29048
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
But if they found thos phenomenon, the drug used in the treatment might caused this perhaps.