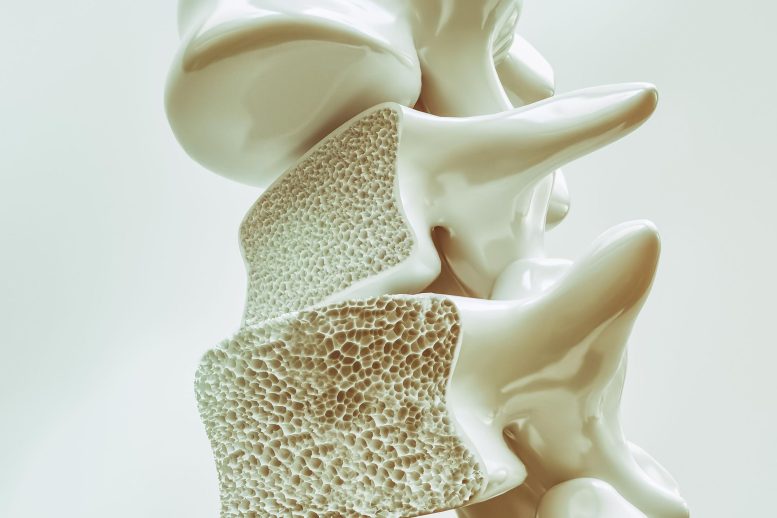
Osteopenia causes reduced bone density without symptoms, driven by aging, hormones, and lifestyle factors. Early detection and healthy habits can prevent worsening and reduce fracture risk.
About 40% of adults worldwide have osteopenia, a condition marked by reduced bone mineral density. It is especially common among postmenopausal women and older adults. In the UK alone, low bone density contributes to more than 500,000 fractures each year.
Osteopenia usually develops without noticeable symptoms and can progress for years without detection. Many people only discover they have it after a fracture or during a bone density scan, often recommended due to factors like aging or menopause. As a result, it remains a widespread yet frequently overlooked public health concern.
Bone is a living tissue that is constantly renewed through a process known as bone remodeling. In this cycle, old bone is broken down (resorption) while new bone is formed (formation).
Bone Remodeling and Peak Bone Mass
In early adulthood, bone breakdown and bone formation are in balance. Bone mass typically reaches its highest level between the mid-20s and early 30s. After this point, bone loss slowly begins to outpace new bone formation, leading to a gradual decline in bone density over time.
Aging is the primary driver of this process, although other factors can speed it up.
Hormonal changes play a major role. The drop in estrogen after menopause can sharply increase bone loss, since this hormone helps limit the natural breakdown of bone. As a result, about half of women over age 50 will experience a fragility fracture.
Lifestyle and Medical Risk Factors
Lifestyle also plays an important role. Smoking, excessive alcohol consumption, and physical inactivity can contribute to reduced bone strength over time. Diet is equally important. Insufficient calcium intake and low vitamin D can limit the body’s ability to build and maintain strong bones.
Certain medications, particularly long-term steroid use, as well as health conditions that affect hormone levels or nutrient absorption (such as Crohn’s or celiac disease), can further increase the risk.
Detecting osteopenia early is crucial. This allows you and clinicians to take steps that can reduce the risk of fractures and prevent osteopenia from progressing to osteoporosis, where bone loss is more advanced, and the risk of fractures is significantly higher.
Diagnosis and Bone Density Testing
Bone mineral density is commonly measured using a dual-energy X-ray absorptiometry (DXA) scan. This is a type of low-dose X-ray scan used to assess bone strength. Results are usually given as a T-score, which compares a patient’s bone density to that of a healthy young adult. A T-score between –1.0 and –2.5 indicates osteopenia, while a T-score below –2.5 meets the diagnostic threshold for osteoporosis.
Management of osteopenia typically focuses on slowing down or preventing further bone loss and reducing the risk of fractures. This involves making lifestyle changes (such as avoiding smoking, limiting alcohol intake, or maintaining a healthy body weight), nutritional support, and, in some cases, prescription treatment.
Weight-bearing exercises, such as walking, dancing, or jogging, stimulate bone formation by placing strain on the skeleton. Resistance training can further strengthen bones and muscles.
Exercise Benefits for Bone Strength
Research shows that regular physical activity is associated with improved bone mineral density and may reduce the risk of osteoporosis. Exercise, such as Tai Chi, also improves balance and muscle strength, reducing the risk of falls that could lead to fractures.
Sufficient calcium intake supports bone structure too, while vitamin D helps the body absorb calcium efficiently. Foods such as dairy products, leafy green vegetables, and fortified products are common dietary sources. Supplements may also be recommended where dietary intake is insufficient. In the UK, vitamin D deficiency is relatively common, so supplementation is often advised.
Not everyone with osteopenia requires drug treatment. Instead, clinicians often use a fracture risk assessment tool to evaluate the ten-year probability of a fracture based on age, bone mineral density, steroid use, and other risk factors.
Treatment Options and Risk Assessment
If fracture risk is high or if a person has already experienced a fragility fracture, medications may be recommended. These can include antiresorptive drugs, which slow bone breakdown and help maintain bone density. Such treatments are more commonly used in osteoporosis but may also benefit high-risk patients with osteopenia.
Osteopenia should not be viewed merely as a mild or early form of osteoporosis but rather as a warning sign and point of intervention. Progression from osteopenia to osteoporosis is not inevitable.
Evidence suggests that early detection and targeted lifestyle changes can maintain bone health, significantly slow bone loss, and reduce the risk of developing osteoporosis later in life. In some cases, bone density may even improve with appropriate treatment and lifestyle adjustments.
But prevention requires a long-term perspective. Bone health reflects the cumulative influences of our health and lifestyle across the lifespan, including our diets, physical activity levels, and hormonal changes we have gone through. Maintaining healthy habits over time remains the most effective strategy for protecting bone strength.
Adapted from an article originally published in The Conversation.![]()
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
2 Comments
thanks for this
You are more than welcome!