Identifying the brain circuits affected in these “lesional” cases of mania, in addition to contributing to understanding the underlying mechanisms, could help find more effective treatments for bipolar disorder. A team of scientists from Portugal and the USA have now announced significant progress in the matter.
People suffering from bipolar disorder experience periods of depression alternating with bouts of mania, during which patients, among other symptoms, may become euphoric, irritable, need less sleep, and talk in an excited and accelerated manner, haphazardly rushing from one idea to the next. But what is less known is that mania is not only associated with bipolar disorder, but can also be the result of brain injury caused, for instance, by head trauma or stroke. The biological explanation for the emergence of this so-called “secondary mania” following brain injury, as opposed to the “primary” mania characteristic of bipolar disorder, has remained elusive. Indeed, previous studies have concluded that many different lesions, in different and seemingly unrelated areas of the brain, can cause mania.
Nonetheless, these lesions seem to have one thing in common: they are usually located in the right hemisphere of the brain, sometimes called the “emotional” brain, the dysfunction of which has been associated with several emotional disorders. While right-sided predominance of lesions was confirmed earlier this year in a systematic study by researchers at the Champalimaud Center for the Unknown (CCU) Neuropsychiatry Unit, led by Albino Oliveira-Maia, that study also confirmed that lesions were distributed across multiple brain areas in that hemisphere. This supported the possibility that lesions leading to mania may have a specific common denominator, other than occurring in a given brain side or brain area, namely at the level of the brain circuits that are affected.
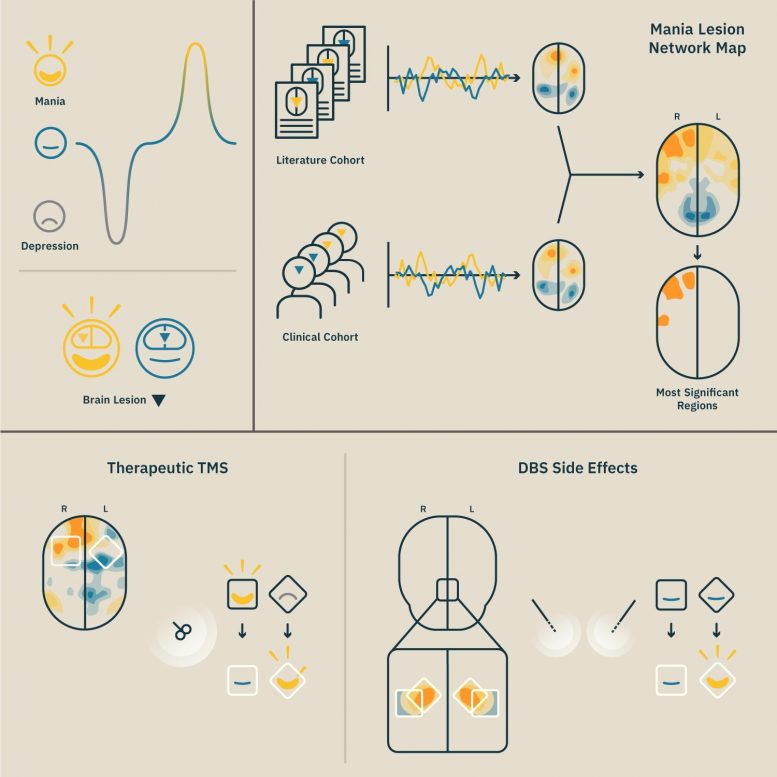
In their latest development, published today (August 24th, 2020) in the Journal of Clinical Investigation, the scientists at the Neuropsychiatry Unit, working in an international collaboration with colleagues from Harvard Medical School, used a novel neuroimaging method, called Lesion Network Analysis, to construct a connectivity map of brain lesions associated with mania. More precisely than ever, this map highlights the circuits connecting brain lesions that induce mania.
The authors thus confirmed that, while no single brain area is lesioned across all cases of secondary manic episodes, lesions are mostly connected to a specific group of regions in the cortex that regulate mood and emotions.
“Lesion locations associated with mania were identified using a systematic literature search and mapped onto a common brain atlas,” the authors write in their paper. “The network of brain regions functionally connected to each lesion location was computed [using functional magnetic resonance images from 1,000 subjects] and contrasted to those obtained from lesion locations not associated with mania [from a group of 79 patients].”
“We found that lesion locations associated with the onset of mania are characterized by a strong connectivity to three right-sided areas, namely the orbitofrontal cortex, inferior temporal cortex, and frontal polar cortex,” summarizes Gonçalo Cotovio, first author of the study, a psychiatry resident and graduate student working under the supervision of Oliveira-Maia, one of the senior authors of the study. These regions have been described, among others, to be included in the so-called limbic circuit, a network in the brain that has been consistently associated with mood regulation and emotional processing. “Furthermore, this unique pattern of functional connectivity was similar across independent groups of patients, and was distinct from those of other neuropsychiatric syndromes,” adds Cotovio.
Stimulating the brain to treat affective disorders?
“Although we still don’t know whether primary mania [characteristic of bipolar disorder] predominantly involves the same brain regions and networks, studying lesional mania may be a valuable approach to understand the neuroanatomy of primary mania in bipolar disorder, since it may highlight brain areas and networks that have been missed in other studies,” Oliveira-Maia points out. “This work may thus contribute towards the development of clinically relevant diagnostic tools, and to find potential brain targets for stimulation treatment of bipolar and other disorders, for example using the technique known as ‘repetitive Transcranial Magnetic Stimulation’ or rTMS.” Repetitive TMS is a non-invasive, painless technique, most widely used for treatment of resistant depression, but also indicated for the treatment of patients with other neuropsychiatric disorders. In repetitive TMS treatments, an electromagnetic coil is applied to a precise location on the head of the patient, to deliver electromagnetic pulses that are capable of modifying neuronal activity in the target brain area. Several brands of these machines have been approved for therapeutic use in the USA, and there is one such machine at the CCU since 2017.
“High frequency rTMS to the right dorsolateral prefrontal cortex may be beneficial in mania, with some right prefrontal sites appearing to be more effective than others,” explains Cotovio. “Our results might be used to guide future brain stimulation trials for mania, since we suggest an optimal target in the right prefrontal cortex, and alternative sites in the right orbitofrontal cortex and right inferior temporal cortex. Confirmation of these potentially therapeutic targets will obviously require clinical validation.”
Finally, given that mania can also occur as a rare complication of Deep Brain Stimulation (DBS), another neuromodulation treatment for neuropsychiatric disorders, the authors explored if their mania lesion network map was consistent with differences in DBS-induced mania risk according to the stimulation site. “Our results indeed suggest that the same brain circuits may be disrupted by brain lesions and by DBS stimulation sites associated with the occurrence of mania,” says Cotovio. And Oliveira-Maia concludes: “future work should address the possibility of using this approach to improve planning of DBS treatments and thus avoid such debilitating side-effects.”
Reference: “Mapping mania symptoms based on focal brain damage” by Gonçalo Cotovio, Daniel Talmasov, J. Bernardo Barahona-Corrêa, Joey Hsu, Suhan Senova, Ricardo Ribeiro, Louis Soussand, Ana Velosa, Vera Cruz e Silva, Natalia Rost, Ona Wu, Alexander L. Cohen, Albino J. Oliveira-Maia and Michael D. Fox, 24 August 2020, Journal of Clinical Investigation.
DOI: 10.1172/JCI136096
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.