
Vitamin A Lowers Pancreatitis Risk During Leukemia Chemotherapy
A diet rich in vitamin A or its derivatives may aid in reducing the likelihood of developing painful pancreatic inflammation in children and young adults with acute lymphoblastic leukemia (ALL) during chemotherapy.
The potential of a dietary solution to prevent a dangerous side effect associated with chemotherapy was highlighted in a study recently published in the journal Science Translational Medicine. The research was conducted under the leadership of Sohail Husain, MD, the head of Pediatric Gastroenterology, Hepatology, and Nutrition at Stanford University and Anil Goud Jegga, DVM, MRes, a computational biologist from Cincinnati Children’s Hospital Medical Center.
For people with ALL, treatment with the enzyme asparaginase helps starve cancer cells by reducing the amount of asparagine circulating in the blood, which the cancer cells need but cannot make themselves. The medication, often used in combination with other chemotherapies, is given via injection into a vein, muscle, or under the skin.
However, an estimated 2% to 10% of asparaginase users develop inflammation of the pancreas in reaction to asparaginase treatment. For a third of these people, the symptoms can be severe.
Jegga and colleagues developed predictive analytics using over 100 million data points encompassing gene expression data, small-molecule data, and electronic health records to understand more of the mechanisms driving asparaginase-associated pancreatitis (AAP) and identify potential interventions to prevent or mitigate AAP.
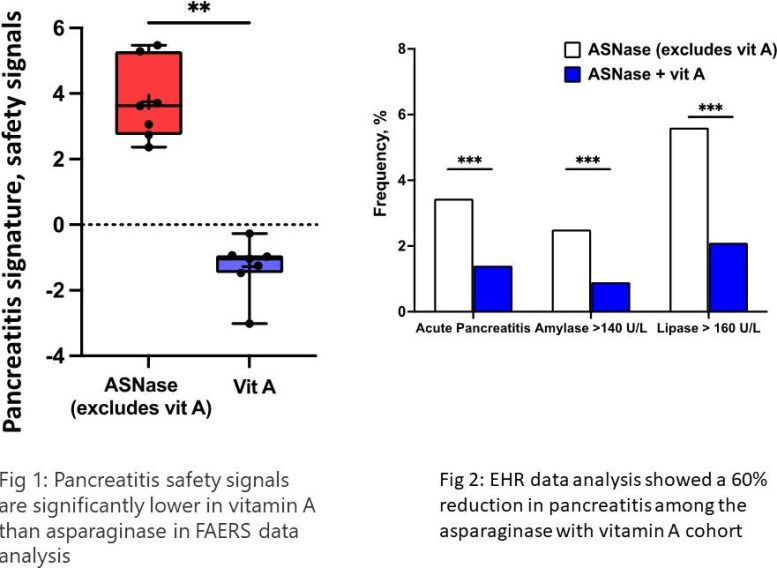
First, they analyzed massive amounts of gene expression data to reveal that gene activity associated with asparaginase or pancreatitis might be reversed by retinoids (vitamin A and its analogs). The team found more supporting evidence by “mining” millions of electronic health records from the TriNetX database and the U.S. Federal Drug Administration Adverse Events Reporting System.
This number crunching and predictive analytics work included the use of the AERSMine software developed at Cincinnati Children’s by Mayur Sarangdhar, Ph.D., MRes, and colleagues. The research team also studied data from mice experiments and compared plasma samples from people with ALL who developed pancreatitis and those who did not.
Real-World Evidence Supporting Vitamin A
Ultimately, the team established two sets of human “real-world” experiences. They found that only 1.4% of patients treated with asparaginase developed pancreatitis when they were also taking vitamin A in contrast to 3.4% of patients who did not. Concomitant use of vitamin A correlated with a 60% reduction in the risk of AAP. Lower amounts of dietary vitamin A correlated with increased risk and severity of AAP.
“This study demonstrates the potential of mining ‘real-world’ data to identify therapy modifiers for improving patient outcomes. In cases where a primary drug induces toxicity but is critical to therapy, such as asparaginase, therapy modifiers, such as vitamin A and its analogs, may be of immediate relevance to patients on asparaginase and ‘at-risk’ for AAP,” says Sarangdhar, a co-first author of the study.
Says Jegga: “Our study highlights the power of heterogeneous data integration and analysis in translational research. By leveraging existing ‘omics and patient-centric data and a systems approach, we were able to identify new insights into the development of AAP and potential interventions to prevent or mitigate this side effect.”
Next Steps
In some ways, learnings from this study could be applied immediately to patient care. However, more clinical research is needed to establish how much vitamin A would be needed to protect ALL patients from pancreatitis; and whether a protective level can be achieved by diet or via supplements. In fact, target vitamin levels may need to vary according to individual differences in metabolism.
Reference: “A systems approach points to a therapeutic role for retinoids in asparaginase-associated pancreatitis” by Cheng-Yu Tsai, Toshie Saito, Mayur Sarangdhar, Maisam Abu-El-Haija, Li Wen, Bomi Lee, Mang Yu, Den A. Lipata, Murli Manohar, Monique T. Barakat, Kévin Contrepois, Thai Hoa Tran, Yves Theoret, Na Bo, Ying Ding, Kristen Stevenson, Elena J. Ladas, Lewis B. Silverman, Loredana Quadro, Tracy G. Anthony, Anil G. Jegga and Sohail Z. Husain, 15 March 2o23, Science Translational Medicine.
DOI: 10.1126/scitranslmed.abn2110
The study was funded by the National Institute of Diabetes and Digestive and Kidney Diseases, the Eunice Kennedy Shriver National Institute of Child Health and Human Development, the Stanford Diabetes Research Center, the National Institutes of Health, Servier Pharmaceuticals, LLC, and the New Jersey Institute for Food, Nutrition, and Health.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.