The identification of separate neural pathways governing itch-scratch responses and chronic itch conditions in mice lays the groundwork for the development of novel therapeutic targets.
Itch serves as a defensive alert in animals, acting to prevent the introduction of potentially harmful pathogens into their bodies by parasites. For instance, when a mosquito alights on a person’s arm, they become aware of its touch and instinctively scratch the area to dispel it. This sensation of itchiness arising from a physical stimulus like a crawling insect is termed as “mechanical,” differing from the “chemical” itchiness provoked by irritants such as a mosquito’s saliva following a bite.
Despite eliciting the same reaction (scratching), recent investigations by scientists at the Salk Institute have discovered that, in mice, there is a specific brain pathway controlling the mechanical sensation which is separate from the neural pathway that is responsible for encoding the chemical sensation.
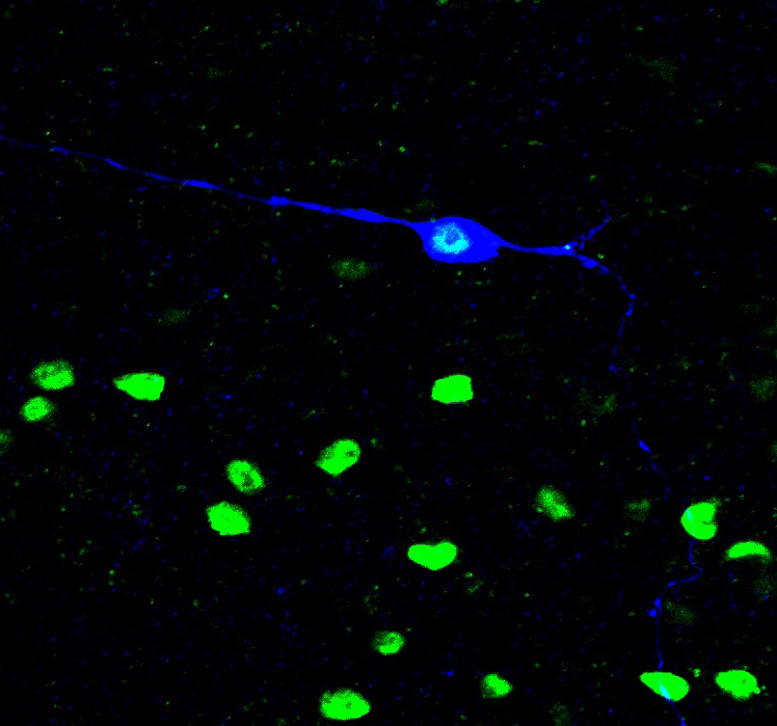
Key Neurons and Neuropeptide Signals Identified
Their findings, recently published in the journal Neuron, show that a small population of neurons relay mechanical itch information from the spinal cord to the brain and identify the neuropeptide signals that regulate both itch types.
“This study provides fundamental insights into how these two forms of itch are encoded by the brain and opens up new avenues for therapeutic interventions for patients that suffer from a range of chronic itch conditions, including ectopic dermatitis and psoriasis,” says co-corresponding author Martyn Goulding, professor and holder of the Frederick W. and Joanna J. Mitchell Chair.
The discovery builds on previous work in Goulding’s lab that had identified the neurons in the spinal cord that control mechanical itch and not chemical itch. Members of Goulding’s lab teamed up with co-corresponding author Sung Han, assistant professor and holder of the Pioneer Fund Developmental Chair, who had previously found that a small region of the brain serves as an alarm center that fields threat signals, both external and internal from within the body.
Han’s team had noticed that a specific group of neurons were crucial for encoding threat signals. Goulding’s lab then decided to focus on these neurons and ask if they play a specific role in relaying mechanical itch signals to this alarm center.

The team used genetic approaches combined with wearable miniaturized microscopes that allowed the researchers to see itch-induced activity in single neurons of mice. The scientists discovered that by removing an inhibitory pathway involved in itch, they could activate a mechanical itch. By observing subsequent activity and changes occurring in the brainstem, they saw that different cells were responding to either mechanical or chemical itch. This allowed the team to classify distinctions between a chemical itch pathway and a mechanical itch pathway and clearly identify the molecules important for regulating them.
Chronic Itch and Its Pathological Drivers
“We found that if you sensitize one pathway, you can stimulate a pathological itch state, and vice versa,” says Han. “This indicates that these two pathways act together to drive chronic itch.”
Next, the scientists plan to examine where in the brain these pathways converge, and then explore the parts of the brain that receive signals that determine the decision of whether to scratch an itch. They also want to better understand how the spinal cord and brainstem differentiate between pain and itch.
“The prevalence of chronic itch increases as we age. For this reason, we would also like to understand more about what is happening to the neural circuits that relay itch as we get older,” says Goulding. “Given that chronic itch is an intractable problem, our findings should help leverage the development of new therapies for treating it.”
Reference: “Identification of an essential spinoparabrachial pathway for mechanical itch” by Xiangyu Ren, Shijia Liu, Amandine Virlogeux, Sukjae J. Kang, Jeremy Brusch, Yuanyuan Liu, Susan M. Dymecki, Sung Han, Martyn Goulding and David Acton, 5 April 2023, Neuron.
DOI: 10.1016/j.neuron.2023.03.013
Other authors include Xiangyu Ren, Shijia Liu, Amandine Virlogeux, Sukjae J. Kang, Jeremy Brusch, and David Acton of Salk, Yuanyuan Liu of the National Institutes of Health, and Susan M. Dymecki of Harvard Medical School.
The study was funded by the National Institutes of Health.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.