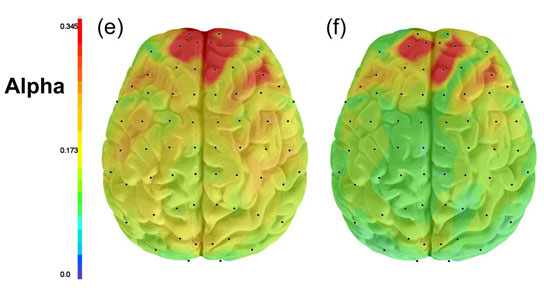
Researchers at UCLA have shown that people with depression have increased connections among most brain areas. While studying the functional connections of the brain in 121 adults diagnosed with MDD, they found that the depressed subjects showed increased synchronization across all frequencies of electrical activity, indicating dysfunction in many different brain networks.
Most of us know what it means when it’s said that someone is depressed. But commonly, true clinical depression brings with it a number of other symptoms. These can include anxiety, poor attention and concentration, memory issues, and sleep disturbances.
Traditionally, depression researchers have sought to identify the individual brain areas responsible for causing these symptoms. But the combination of so many symptoms suggested to University of California, Los Angeles (UCLA) researchers that the multiple symptoms of depression may be linked to a malfunction involving brain networks — the connections that link different brain regions.
Now, for the first time, these UCLA researchers have shown that people with depression have increased connections among most brain areas. Indeed, their brains are widely hyperconnected. The report, published this week in the online journal PLoS One, sheds new light on the brain dysfunction that causes depression and its wide array of symptoms.
“The brain must be able to regulate its connections to function properly,” said the study’s first author, Dr. Andrew Leuchter, a professor of psychiatry at the Semel Institute for Neuroscience and Human Behavior at UCLA. “The brain must be able to first synchronize, and then later desynchronize, different areas in order to react, regulate mood, learn and solve problems.”
The depressed brain, Leuchter said, maintains its ability to form functional connections but loses the ability to turn these connections off.
“This inability to control how brain areas work together may help explain some of the symptoms in depression,” he said.
In the study, the largest of its kind, the researchers studied the functional connections of the brain in 121 adults diagnosed with major depressive disorder, or MDD. They measured the synchronization of electrical signals from the brain — brain waves — to study networks among the different brain regions.
While some previous studies have hinted at abnormal patterns of connections in MDD, the UCLA team used a new method called “weighted network analysis” to examine overall brain connections. They found that the depressed subjects showed increased synchronization across all frequencies of electrical activity, indicating dysfunction in many different brain networks.
Brain rhythms in some of these networks regulate the release of serotonin and other brain chemicals that help control mood, said Leuchter, who is also the director of UCLA’s Laboratory of Brain, Behavior, and Pharmacology and chair of the UCLA Academic Senate.
“The area of the brain that showed the greatest degree of abnormal connections was the prefrontal cortex, which is heavily involved in regulating mood and solving problems,” he said. “When brain systems lose their flexibility in controlling connections, they may not be able to adapt to change.
“So an important question is, to what extent do abnormal rhythms drive the abnormal brain chemistry that we see in depression? We have known for some time that antidepressant medications alter the electrical rhythms of the brain at the same time that levels of brain chemicals like serotonin are changing. It is possible that a primary effect of antidepressant treatment is to ‘repair’ the brain’s electrical connections and that normalizing brain connectivity is a key step in recovery from depression. That will be the next step in our research.”
Reference: “Resting-State Quantitative Electroencephalography Reveals Increased Neurophysiologic Connectivity in Depression” by Andrew F. Leuchter, Ian A. Cook, Aimee M. Hunter, Chaochao Cai and Steve Horvath, 24 February 2012, PLoS One.
DOI: 10.1371/journal.pone.0032508
Other authors of the study include Dr. Ian A. Cook, Aimee M. Hunter, Chaochao Cai and Steve Horvath, all of UCLA. Funding for the study was provided by the National Institutes of Health, Lilly Research Laboratories and Pfizer Pharmaceuticals. The authors report no conflict of interest.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
Has the use of CBD or Epidiolex been used at the same time as this imaging to show what it does to these brain areas? I have a 13yo grandson that has been on brain wave therapy ,Zoloft and clonidine for the last year..I want to try Epidiolex as our next drug to add..too many side effects with antipsychotics..