A newly identified trigger of brain inflammation could offer a fresh target for slowing Alzheimer’s progression.
The brain has its own built-in immune system that identifies threats and responds to them. In Alzheimer’s disease, growing evidence shows that this system becomes persistently overactive. The result is chronic inflammation that damages the connections between brain cells.
In a preclinical study using human Alzheimer’s brain cells, scientists at Scripps Research have identified a molecular trigger behind this process. The finding points to a potential drug target that could help control harmful inflammation.
A Molecular Switch Behind Inflammation
The study, published in Cell Chemical Biology, focuses on a protein called STING. Under normal conditions, STING acts as part of the immune system’s early warning network. In Alzheimer’s brains, however, researchers found that STING undergoes a chemical change called S-nitrosylation (or SNO, a reaction involving sulfur, oxygen and nitrogen). This modification drives the protein into an overactive state. When scientists blocked this change in a mouse model, brain inflammation was reduced.
“This is a new and important therapeutic target for Alzheimer’s disease,” says senior author Stuart Lipton, the Step Family Foundation Endowed Chair at Scripps Research and a clinical neurologist. “It’s exciting to see that blocking this switch in mice reduces inflammation and protects the very brain cell connections that are lost in Alzheimer’s, especially because we found the same pathway to be activated in human Alzheimer’s brain samples and in human stem cell-derived models.”
More than 30 years ago, Lipton, who also co-directs the Neurodegeneration New Medicines Center at Scripps Research, first described S-nitrosylation. In this process, a molecule related to nitric oxide (NO) attaches to a cysteine amino acid in proteins, forming “SNO” and altering how the protein behaves.
His lab later showed that SNO can be triggered by aging, inflammation, and environmental exposures such as air pollution and wildfire smoke. These changes can disrupt many proteins throughout the body. This widespread effect, referred to as a “SNO-STORM,” has been linked to diseases including cancer, Parkinson’s disease, and Alzheimer’s.
Pinpointing STING’s Weak Spot
In the new study, researchers took a closer look at STING, which had already been associated with Alzheimer’s-related inflammation. Lipton’s team, led by postdoctoral researcher Lauren Carnevale, worked with Professor John Yates III, a mass spectrometry expert at Scripps Research and holder of the John Lytton Young Endowed Chair.
They identified the exact location where S-nitrosylation occurs on STING, focusing on a single amino acid known as cysteine 148. When this site is modified, STING forms clusters and sets off inflammatory signaling.
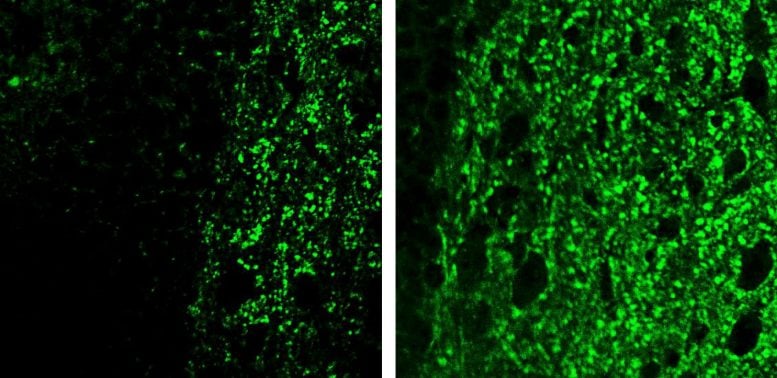
Elevated levels of this altered form, called SNO-STING, were detected in postmortem brain tissue from Alzheimer’s patients, in lab-grown human brain immune cells exposed to Alzheimer’s proteins, and in mice with the disease.
Further experiments revealed that hallmark Alzheimer’s protein clumps, including amyloid-beta and alpha-synuclein, can directly trigger S-nitrosylation of STING. This suggests a feedback loop. Protein buildup, along with aging and environmental stress, may spark inflammation that produces nitric oxide. That, in turn, modifies STING and amplifies inflammation even further.
Protecting Brain Connections
To test this mechanism, the team created a version of STING that lacks cysteine 148, preventing the S-nitrosylation step. When introduced into a mouse model of Alzheimer’s, this modified protein significantly reduced inflammation in brain immune cells.
Importantly, it also preserved synapses, the connections between nerve cells that are essential for memory and thinking. Loss of synapses is closely linked to cognitive decline in dementia, so protecting them is a key goal in Alzheimer’s research.
“What makes this target particularly promising is that we can quiet the pathological overactivation of STING without shutting down the normal immune response,” says Lipton. “You still need STING to protect yourself from infections, and when we target cysteine 148, we’re not blocking the entire molecule; we’re just preventing STING from becoming overactivated.”
Lipton’s team is now developing small molecules designed to block cysteine 148, with plans to test them in future preclinical studies.
Reference: “Redox regulation of neuroinflammatory pathways contributes to damage in Alzheimer’s disease brain” by Lauren N. Carnevale, Piu Banerjee, Xu Zhang, Jazmin Navarro, Charlene K Raspur, Parth Patel, Tomohiro Nakamura, Emily Schahrer, Henry Scott, Nhi Lang, Jolene K. Diedrich, Amanda J. Roberts, John R. Yates and Stuart A. Lipton, 23 April 2026, Cell Chemical Biology.
DOI: 10.1016/j.chembiol.2026.03.017
This work was supported in part by the National Institutes of Health (R35 AG071734, U01 AG088679, RF1 AG057409, R01 AG078756, R01 AG056259, R01 DA048882, DP1 DA041722 and R01 AG077046), and the U.S. Department of Defense/U.S. Department of the Army (AR230101).
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
6 Comments
How might I volunteer to test the reverse? If they can accelerate brain deterioration, wouldn’t that help validate their theory in a quicker way?
I’d be willing to be a guinea pig for this research before my memory gets any worse – its distressing to know what could be ahead for me and so many others.
My son is missing and Dallas life prison. Is under arrest for hisdissapearence and possible brain stealth I’m still looking for my children I think it’s inhumane to experiment on childrens brains .Princess. Constance. Kennedy sincerely
Hilarious
This looks very promising BUT it might be too late for my husband How can we find out about clinical trials Please keep going with this research and updates We are all suffering families PLEASE keep going
That’s great.
The above findings align with my observations that Alzheimer’s Disease is not a disease of patients suffering from Asthma and Diabetes Mellitus.
Intriguingly, salbutamol is known to alleviate cGAS-STING axis, suggesting it’s potential to mange AD. Metformin similarly is an inhibitor of cGAS-STING axis.
Kind regards.