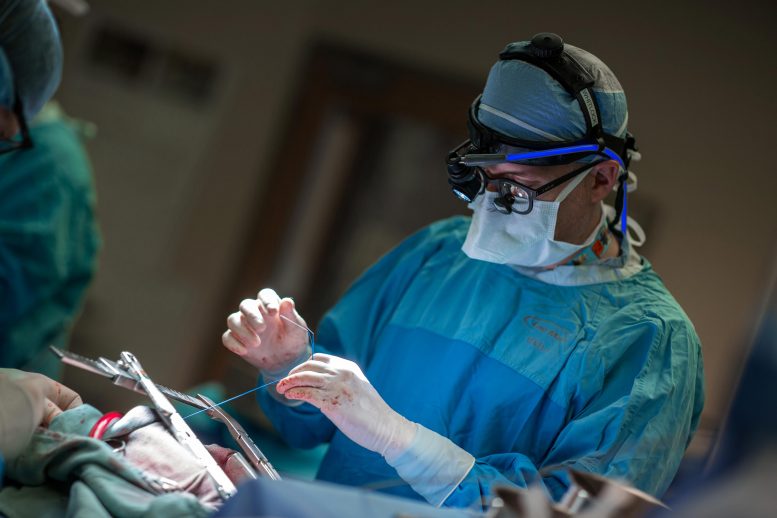
Removing left atrial appendage cuts the risk of strokes by more than one-third in patients with atrial fibrillation.
A simple surgery saves patients with heart arrhythmia from often-lethal strokes, says a large international study led by McMaster University.
Researchers found that removing the left atrial appendage — an unused, finger-like tissue that can trap blood in the heart chamber and increase the risk of clots — cuts the risk of strokes by more than one-third in patients with atrial fibrillation.
Even better, the reduced clotting risk comes on top of any other benefits conferred by blood-thinner medications patients with this condition are usually prescribed.
Proven Safe and Effective in Major Global Trial
“If you have atrial fibrillation and are undergoing heart surgery, the surgeon should be removing your left atrial appendage, because it is a set-up for forming clots. Our trial has shown this to be both safe and effective for stroke prevention,” said Richard Whitlock, first author of the study.
“This is going to have a positive impact on tens of thousands of patients globally.”
Whitlock is a scientist at the Population Health Research Institute (PHRI), a joint institute of McMaster University and Hamilton Health Sciences (HHS); a professor of surgery at McMaster, the Canada Research Chair in cardiovascular surgical trials, a cardiac surgeon for HHS, and is supported by a Heart and Stroke Foundation career award.
The co-principal investigator of the study is Stuart Connolly who has also advanced this field by establishing the efficacy and safety of newer blood thinners. He is a professor emeritus of medicine at McMaster, a PHRI senior scientist, and an HHS cardiologist.

“The results of this study will change practice right away because this procedure is simple, quick and safe for the 15 percent of heart surgery patients who have atrial fibrillation. This will prevent a great burden of suffering due to stroke,” Connolly said.
The study results were fast tracked into publication by The New England Journal of Medicine and presented at the American College of Cardiology conference today.
The study tracked 4,811 people in 27 countries who are living with atrial fibrillation and taking blood thinners. Consenting patients undertaking cardiopulmonary bypass surgery were randomly selected for the additional left atrial appendage occlusion surgery; their outcomes compared with those who only took medicine. They were all followed for a median of four years.

Whitlock said it was suspected since the 1940s that blood clots can form in the left atrial appendage in patients with atrial fibrillation, and it made sense to cut this useless structure off if the heart was exposed for other surgery. This is now proven to be true.
Atrial fibrillation is common in elderly people and is responsible for about 25 percent of ischemic strokes which are caused when blood clots block arteries supplying parts of the brain. The average age of patients in the study was 71.
Combining Medicine and Surgery for Better Outcomes
“In the past all we had was medicine. Now we can treat atrial fibrillation with both medicines and surgery to ensure a much better outcome,” said Whitlock.
He said that the current study tested the procedure during cardiac surgery being undertaken for other reasons, but the procedure can also be done through less invasive methods for patients not having heart surgery. He added that future studies to examine that approach will be important.
Whitlock said the left atrial appendage is a leftover from how a person’s heart forms as an embryo and it has little function later in life.
“This is an inexpensive procedure that is safe, without any long-term adverse effects, and the impact is long-term.”
Reference: “Left Atrial Appendage Occlusion during Cardiac Surgery to Prevent Stroke” by Richard P. Whitlock, M.D., Ph.D.; Emilie P. Belley-Cote, M.D., Ph.D.; Domenico Paparella, M.D.; Jeff S. Healey, M.D.; Katheryn Brady, B.Sc.; Mukul Sharma, M.D.; Wilko Reents, M.D.; Petr Budera, M.D., Ph.D.; Andony J. Baddour, M.D., Ph.D.; Petr Fila, M.D., Ph.D.; P.J. Devereaux, M.D., Ph.D.; Alexander Bogachev-Prokophiev, M.D., Ph.D.; Andreas Boening, M.D.; Kevin H.T. Teoh, M.D.; Georgios I. Tagarakis, M.D., Ph.D.; Mark S. Slaughter, M.D.; Alistair G. Royse, M.D.; Shay McGuinness, M.B., Ch.B.; Marco Alings, M.D., Ph.D.; Prakash P. Punjabi, F.R.C.S., C. David Mazer, M.D.; Richard J. Folkeringa, M.D., Ph.D.; Andrea Colli, M.D.; Álvaro Avezum, M.D., Ph.D.; Juliet Nakamya, Ph.D.; Kumar Balasubramanian, M.Sc.; Jessica Vincent, M.Sc., Pierre Voisine, M.D.; Andre Lamy, M.D.; Salim Yusuf, F.R.S.C., D.Phil. and Stuart J. Connolly, M.D. for the LAAOS III Investigators, 15 May 2021, New England Journal of Medicine.
DOI: 10.1056/NEJMoa2101897
External funding for the study came from the Canadian Institutes of Health Research and the Heart and Stroke Foundation of Canada.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
1 Comment
Not for all AFib patients.
Obliteration or amputation of the LAA may help to reduce the risk of thromboembolism, but this may result in undesirable physiological sequelae such as reduced atrial compliance and a reduced capacity for ANF secretion in response to pressure and volume overload.